Plaque psoriasis is an autoimmune condition. It causes thick patches (plaques) on your skin, including your scalp. There isn’t a cure, but treatments can alleviate related symptoms.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
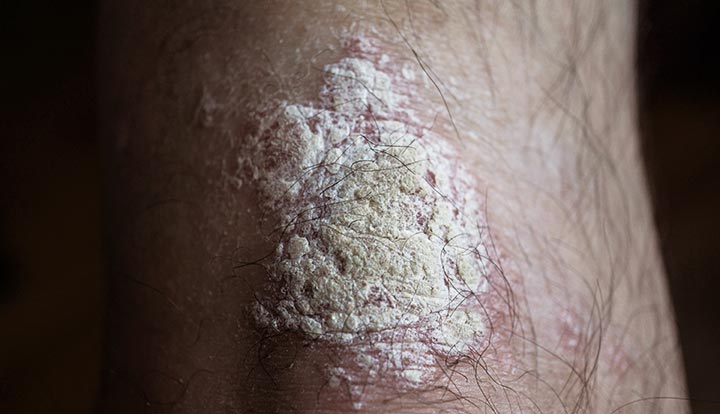
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22842-plaque-psoriasis)
Plaque psoriasis (psoriasis vulgaris) is a long-lasting (chronic) autoimmune disease that causes your cells to reproduce very quickly. It’s a type of psoriasis that causes thick, scaly patches called plaques on your skin. It most commonly affects your:
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Severe cases of plaque psoriasis may affect your entire body, including your:
Plaque psoriasis can affect anyone. But you may be more likely to have plaque psoriasis if you:
Plaque psoriasis is the most common type of psoriasis. It affects about 6.7 million adults. About 80% to 90% of people with psoriasis have plaque psoriasis.
Plaque psoriasis causes thick, rough, scaly, discolored plaques to develop on your skin. The plaques can be itchy or painful — they may feel like a burn or a sting.
Symptoms of plaque psoriasis include:
Plaque psoriasis is an immune system problem. Your immune response overreacts, causing inflammation, which leads to new skin cells growing too fast.
Typically, new skin cells grow every 28 to 30 days. But if you have plaque psoriasis, new cells grow and move to your skin's surface every three to four days. The buildup of new cells replacing old cells creates plaques.
Advertisement
Plaque psoriasis runs in families, so there may be a genetic trigger. Parents may pass it down to their children.
Plaque psoriasis flare-ups differ from person to person. No one knows exactly what causes them. Common plaque psoriasis triggers may include:
Plaque psoriasis isn’t contagious. You can’t spread plaque psoriasis to another person through skin-to-skin contact or unprotected sex.
Your healthcare provider will examine your affected areas, and they’ll look for common signs of plaque psoriasis. They’ll also ask about your symptoms, your family history and if you’ve recently started or stopped using a product or medication just before your flare-up.
Your healthcare provider may perform several tests to rule out other conditions that could cause your plaques, like eczema or dermatitis. This series of tests is a differential diagnosis. The tests may include:
There isn’t a cure for plaque psoriasis. You may have flare-ups and times where the plaques go away (remission). Treatment can provide relief for your symptoms.
Certain foods and drinks may contribute to plaque psoriasis flare-ups. If you have plaque psoriasis, it’s a good idea to keep track of what you eat and drink in a food journal. Keeping track of what you eat and drink can help you and your healthcare provider determine any causes of your flare-ups.
An anti-inflammatory diet may limit your plaque psoriasis flare-ups. Foods that have anti-inflammatory properties include:
Foods and drinks that may cause flare-ups may include:
Your healthcare provider may prescribe the following as a cream, lotion or gel to treat mild cases of plaque psoriasis:
Salicylic acid shampoo treats plaques in your scalp.
In more severe or widespread cases of plaque psoriasis, your healthcare provider may prescribe:
Advertisement
Several home remedies can help you manage the symptoms of plaque psoriasis.
While home remedies are safe for most people, it’s a good idea to check with your healthcare provider before trying some of the following options. You may be at risk of developing an allergic reaction.
Plaque psoriasis may flare up and go into remission throughout your life. But it can generally be well-managed with treatment.
Advertisement
Yes, you can have sex if you have a plaque psoriasis flare-up on your genitals or in your genital region, including your inner thighs, butt crack (intergluteal cleft) or the skin just above your genitals (pubis).
Plaque psoriasis isn’t a sexually transmitted infection (STI). Still, it can look like an STI. It’s a good idea to be honest with your partner if you have a flare-up. If they have any questions, encourage them to talk to a healthcare provider before having sex.
If you have a plaque psoriasis flare-up on your genitals, you may experience discomfort or pain during sex. Sexual lubricants (lubes) and condoms can help ease discomfort, pain or itching.
After sex, carefully clean and dry your genitals and reapply any plaque psoriasis medications.
There isn’t any way to prevent plaque psoriasis. If you have it, it may come and go throughout your life. Treatments can reduce symptoms, even in people with severe plaque psoriasis.
If you have plaque psoriasis, the best way to take care of yourself is to:
Other steps to stay as healthy as possible include:
Advertisement
Contact your healthcare provider if:
Guttate psoriasis and plaque psoriasis look different. Guttate psoriasis looks like small, discolored, drop-shaped scaly spots and usually appears in children and young adults. It typically appears after a sore throat caused by a streptococcal infection. It often goes away after several weeks, even if you don’t seek treatment.
Eczema and plaque psoriasis look and feel different. Eczema is very itchy. Plaque psoriasis may be itchy, but it also may burn or sting.
Eczema irritates your skin and makes it change color, and it may cause tough, swollen, dark patches of skin. Plaque psoriasis patches are often white or silvery, and they rise above your skin. Plaque psoriasis is also thicker than eczema.
Plaque psoriasis is an autoimmune disease that causes thick patches to develop on your skin or scalp. You may feel self-conscious, and it can be unpleasant if it itches or is painful. But it isn’t contagious, and treatments can help your symptoms improve.
It’s important to pay attention to your skin. Contact your health provider as soon as you notice any plaques develop on your skin.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Coping with psoriasis can be frustrating and distressing. Cleveland Clinic experts offer personalized treatment to help you manage this chronic condition.
