Venous thoracic outlet syndrome (VTOS) is a compressed subclavian vein. Your subclavian vein carries blood from your arm to your heart. If you have VTOS, you may have arm swelling, discoloration or heaviness. Treatment usually includes medications to dissolve blood clots. If needed, you may also have surgery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
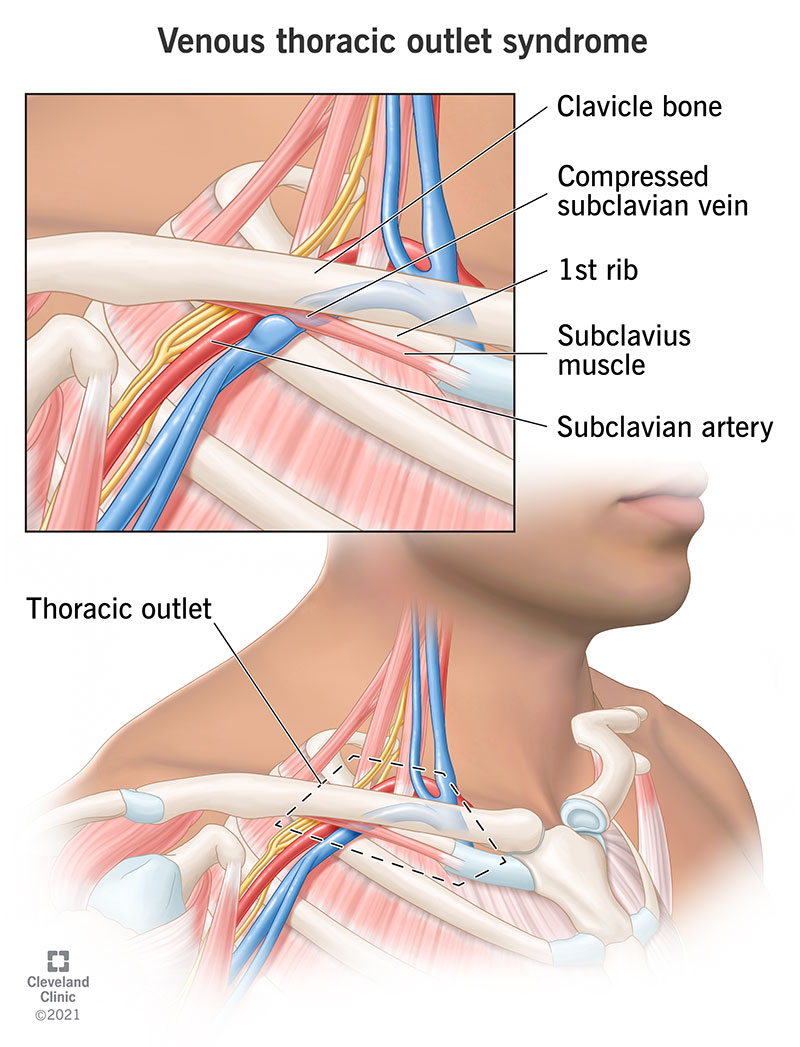
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22317-venous-thoracic-outlet-syndrome)
Venous thoracic outlet syndrome (VTOS) is a condition that affects your subclavian vein. Veins take blood from your tissues back to your heart and lungs to collect oxygen. The subclavian vein is in your arm behind your collarbone (clavicle). The space where this vein runs is the thoracic outlet.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
In VTOS, you have a squeezed (compressed) vein in the thoracic outlet. People with VTOS often have arm soreness, swelling or discoloration. Another name for VTOS is Paget-Schroetter syndrome (PSS).
Women ages 20 to 50 are more likely to get any type of thoracic outlet syndrome. You are also more likely to develop VTOS if you play sports or have a job that requires repetitive motion in your arm and shoulder.
VTOS can be dangerous if you don’t get treatment. The compression from VTOS can cause blood clots to form in the subclavian vein. The clots can block blood flow in your arm or hand or to your lungs. A blood clot that moves to your lungs is a pulmonary embolism.
If you have symptoms of thoracic outlet syndrome, see a doctor for a diagnosis. If you have severe symptoms that could point to possible pulmonary embolism, seek emergency care. A pulmonary embolism causes chest pain, cough and shortness of breath.
Experts don’t know exactly how many people have thoracic outlet syndrome. All types of TOS are rare, and VTOS is one of the least common types of TOS. About 2 in 50 people with TOS have it.
Between your clavicle and first rib, a vein called the subclavian vein carries blood from your arm back to your heart. Most people have plenty of space for the subclavian vein to run from their arm to their heart without being abnormally compressed. But some people have a naturally narrow passageway for the subclavian vein.
Advertisement
If you have a narrow passageway, overusing your arm and shoulder can squeeze (compress) or aggravate the subclavian vein. This compression can block blood flow and lead to clots.
Other causes of venous thoracic outlet syndrome can include:
Most people with VTOS have symptoms that affect one arm and hand. You may have:
If you have VTOS symptoms, your provider will visually examine your shoulder, neck and arm. Your provider may ask you to move your arms in specific ways to check your range of motion.
Your provider will also ask you about symptoms and take your blood pressure. If your provider suspects VTOS, you may have more tests to examine your thoracic outlet.
Venous thoracic outlet diagnosis may involve imaging tests. To view blood flow in your veins and internal structures, you may have:
VTOS treatment can include nonsurgical and surgical options. Typically, your provider prescribes medications to dissolve blood clots. You may take anticoagulants such as warfarin (Coumadin®) or direct oral anticoagulants (Xarelto® or Eliquis®).
After the clot breaks up, you may need surgery to prevent blood clots from occurring again. During surgery, your provider may:
Without treatment, venous thoracic outlet syndrome can cause complications such as blood clots. Thankfully, early treatment helps.
Research shows that getting treatment within the first 14 days of symptoms significantly increases your chances of a successful outcome. If you have any signs of VTOS, see a healthcare provider right away.
There’s no guaranteed way to avoid VTOS. But you can lower your risk of compression injuries by:
Advertisement
You may also want to ask your healthcare provider:
Venous thoracic outlet syndrome affects the subclavian vein. A compressed subclavian vein can lead to arm swelling, discoloration and soreness. You are more likely to get VTOS if you have a naturally narrow passageway for the subclavian vein. Frequent, repetitive shoulder and arm movements also increase your risk of VTOS. If you have VTOS, your provider may prescribe medications to dissolve blood clots. You may also need surgery to widen the area around your subclavian vein.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Vascular disease may affect your life in big and small ways. Cleveland Clinic’s specialists treat the many types of vascular disease so you can focus on living.
