Vocal cord paralysis happens when you can’t control the muscles that move one or both vocal cords. Vocal cords that can’t close may leave a space for food, fluids and saliva (spit) to enter your windpipe and lungs. Problems with breathing, swallowing and speaking can result. Healthcare providers treat this condition with voice therapy and surgery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
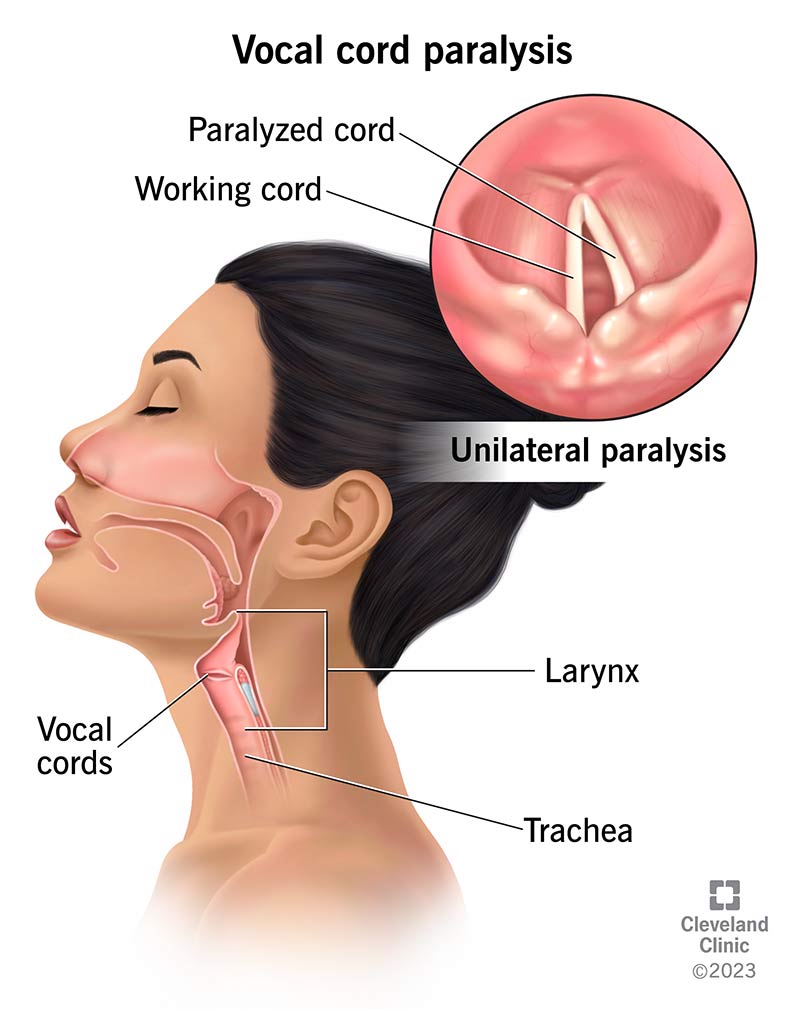
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/vocal-cord-paralysis)
Vocal cord paralysis involves one or both vocal cords (vocal folds) not moving as they should. Your vocal cords are two bands of muscle inside your voice box (larynx) located atop your windpipe (trachea). They open when you breathe so air can pass through. They close when you swallow to prevent food and drink from slipping into your windpipe. When you speak or sing, your vocal cords touch. Your lungs send air through them, causing them to vibrate and make sounds.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
With vocal cord paralysis, nerve damage prevents the muscles inside your vocal cords from opening and closing properly. As a result, you may have trouble speaking, swallowing or even breathing — all functions that depend on your vocal cords moving.
Vocal cord paralysis can affect one vocal cord (unilateral) or both vocal cords (bilateral):
Unilateral vocal cord paralysis is much more common than bilateral vocal cord paralysis. It’s rare for both vocal cords to become paralyzed. Still, both types can affect anyone of any age.
Unilateral vocal cord paralysis ranges in severity from mild to severe. For instance, mild cases may make speaking difficult. In more severe cases, you may experience shortness of breath when speaking. You may cough or choke when eating or drinking.
Advertisement
With bilateral vocal cord paralysis, your vocal cords may get too close together, making it difficult to breathe. Your swallowing can also be affected. Food or drink can slip into your windpipe and lungs, causing aspiration pneumonia.
See a healthcare provider immediately if you’re having trouble breathing or swallowing.
Symptoms depend on the extent of the paralysis and the position of your vocal cords in relation to each other.
Symptoms may include:
You may not feel sensations from the vocal cord directly. Instead, you’ll feel the symptoms resulting from a paralyzed vocal cord. The sensation may feel like fatigue as you exhaust your energy, trying to draw more air into your lungs or get your voice to sound as you’d like. It may feel like choking if food or drink slips into your windpipe. Some people with paralyzed vocal cords feel like they always have mucus in their throats that they can’t clear.
Many people with vocal cord paralysis can still speak, but it may require more effort. You may notice changes in how your voice sounds. You may get winded when you talk. If your paralysis is more severe, you may lose your voice.
Multiple conditions can damage the nerves that control how your vocal cords move, including:
Advertisement
Sometimes, a vocal cord can get paralyzed after a cold or upper respiratory infection. Healthcare providers can’t always determine the exact cause. These cases of vocal cord paralysis are called idiopathic, or post viral.
Medical experts in ear, nose and throat conditions (otolaryngologists), including providers who specialize in conditions involving your throat and voice box (laryngologists), often diagnose and treat vocal cord paralysis. First, they’ll ask about your symptoms and health history. To confirm a diagnosis, your provider may order the following:
Advertisement
Treatment depends on the severity of the paralysis and your symptoms. If paralysis is mild, you may need voice therapy to improve how your vocal cords work. During therapy, you do special exercises that strengthen your vocal cords, help you control muscles that help you speak and improve how you breathe when speaking.
More severe vocal cord paralysis may require surgery.
With unilateral vocal cord paralysis, providers often choose to delay surgery for up to a year to allow time for the condition to improve. Sometimes, the vocal cord is just bruised or strained and needs time to repair itself. This can take months. Voice therapy administered by a speech-language pathologist with expertise in voice care can sometimes be very effective and help strengthen your voice if the problem is mild/moderate.
A laryngologist may recommend surgery or a vocal fold injection to help improve voice, swallowing and breathing problems. The options include:
Advertisement
People with two paralyzed vocal cords can have a dangerously narrow airway. They’ll often need a tracheostomy (tracheotomy or “trach”) to open their airway and help with breathing.
During this procedure, a healthcare provider makes an incision and inserts a tube into your neck. The tube opens the airway and helps you breathe. Sometimes, your provider may remove a portion in the back of one or both vocal cords with a laser to widen the airway, creating more space to breathe through. Another procedure to help you breathe long term if you have a trach, is a tube-free tracheostomy.
Sometimes, the vocal cords repair themselves. This may take months. With voice therapy, vocal cord injections or implants, your voice may get stronger and allow people to hear you better when you talk. You may also feel that treatment improves your swallowing and breathing. Ask your healthcare provider how much of your vocal cord function you’ll likely regain with treatment.
Many cases of vocal cord paralysis can improve by themselves with time. Voice therapy and sometimes filler injections can help make your symptoms better while waiting for your vocal cords to recover. If your vocal cord is permanently paralyzed, an implant to keep your vocal cord in place is the treatment of choice. Rarely, your provider may need to readjust the implant if it moves out of place.
With treatment, many people regain the ability to talk and swallow after vocal cord paralysis. Your prognosis depends on several factors, including whether the paralysis affected one or both vocal cords and if it’s mild or severe.
You can’t always prevent vocal cord paralysis. Talk to your healthcare provider if you have a condition that increases your risk. They may recommend regular checkups to test your vocal cords. You may need voice therapy to improve how your vocal cords work.
Talk to a healthcare provider if you have signs of vocal cord paralysis. Voice changes, unexplained hoarseness, noisy breathing, shortness of breath when talking, or coughing and choking with food or liquids aren’t normal. Starting treatments early can prevent your condition from worsening. In some cases, noninvasive treatments, like voice therapy, can prevent you from having surgery.
Seek care immediately if you’re having trouble breathing or swallowing. Not getting enough air is a sign of bilateral vocal cord paralysis, the most serious type. Inhaling food or drink because your vocal cords aren’t closing properly can lead to aspiration pneumonia, which is fatal without treatment.
See a healthcare provider if you have signs of vocal cord paralysis, including trouble breathing, voice changes or difficulty swallowing. Talk to your provider if you have a condition or illness that increases your risk of vocal cord paralysis. These can include multiple sclerosis or Parkinson’s, or recent chest or neck surgery. Voice therapy may prevent your condition from worsening and improve your vocal cord function.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Vocal cord paralysis can make talking, breathing and swallowing difficult. Cleveland Clinic offers therapies and surgeries to help you find your voice again.
