Spondylolisthesis happens when one of the bones in your spine (your vertebrae) slips out of alignment and presses down on the vertebra below it. Many people can manage symptoms like pain and stiffness without surgery. But your provider will suggest surgical repair if the slip is a high grade or nonsurgical treatments don’t help.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
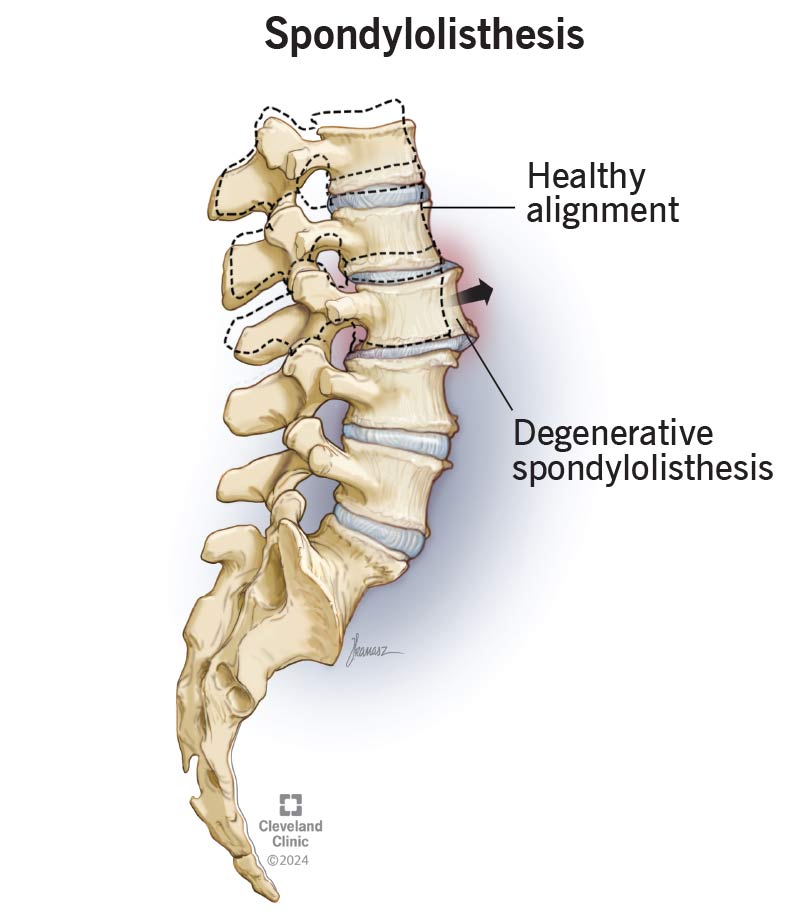
Spondylolisthesis happens when one of the vertebrae in your spine slips out of position and puts pressure on the vertebra below it. Spondylolisthesis is pronounced spohn-di-low-less-THEE-sis.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Your spine is made of 33 stacked bones called vertebrae (the plural form of vertebra). Your vertebrae are linked together but can move a little bit as you move your body and change your posture.
If you have spondylolisthesis, one of your vertebrae moves more than it should and slides out of its usual spot and onto the vertebra below it. This can put pressure on nerves around your spine and cause back pain and other symptoms.
Spondylolisthesis can happen anywhere in your spine, but it’s most common in your lower back (lumbar spine). It can also affect your neck (cervical spine) or your midback from the bottom of your neck to just below your ribs (thoracic spine).
The vertebrae in your spine are links in a chain that constantly support you. It might sound scary to think about one of those links falling out of alignment, but that doesn’t mean the whole chain is in trouble. Spondylolisthesis usually responds very well to treatment. Visit a healthcare provider if you notice new pain in your back, legs or anywhere else that’s making it hard to move throughout your day.
There are several spondylolisthesis types, including:
Advertisement
Less common spondylolisthesis types include:
Some people have spondylolisthesis and never experience symptoms. Very minor (low-grade) slippage may not put enough pressure on the rest of your spine or nerves to cause any symptoms.
If you do have symptoms, they might include:
You might feel pain in other areas of your back, depending on where in your spine the vertebra slips out of place. The pain might spread (radiate) into your butt (buttocks) or thighs.
What makes a vertebra slip out of alignment depends on which type of spondylolisthesis you have. The most common causes include:
Spondylolisthesis can affect anyone, but some people have a higher risk, including:
If it’s not diagnosed and treated, spondylolisthesis can increase your risk of:
A healthcare provider will diagnose spondylolisthesis with a physical exam and imaging tests. They’ll examine your back and spine.
Tell your provider when you first noticed pain or other symptoms, and if any activities or movements make the symptoms worse. Let your provider know what you were doing before symptoms started, especially if you know you experienced a specific injury.
Your provider will use a spinal X-ray to take pictures of your vertebrae. You might also need a CT scan (computed tomography scan) or MRI (magnetic resonance imaging) to look for damage to your disks or nerves.
Your provider will classify the spondylolisthesis with a grade to indicate how far out of position your vertebra slipped. They might use a number grade or simply define it as low or high:
Advertisement
Most people with spondylolisthesis can manage their symptoms with nonsurgical treatments, including:
Advertisement
Not everyone needs surgery to fix spondylolisthesis. It’s possible to live with a low-grade slippage if the out-of-place vertebra doesn’t cause severe symptoms or increase your risk of complications.
Your provider will tell you when it might be time to consider surgery. You’re more likely to need surgery if you:
Your surgeon will probably do a spinal fusion to realign your vertebrae and give the area around them more strength. You might also need a spinal decompression to remove extra pressure on your sciatic nerve.
Your provider or surgeon will tell you which type of surgery you’ll need and what to expect.
Some people who need a spinal fusion have a reduced range of motion or flexibility in their back after surgery. Spinal fusion joins two vertebrae that heal into one bone. For most people, that tradeoff is worth it because they experience much less pain. But don’t be afraid to talk to your surgeon before you decide to have surgery. They’ll help you understand the risks and set realistic goals.
Advertisement
If you have spondylolisthesis, nonsurgical treatments like rest, medication and physical therapy should improve your symptoms. Your provider will take additional X-rays as you start treatment to see if your vertebra moves further out of alignment. Your provider will keep an eye on the out-of-place vertebra. If it moves too much, you might need surgery.
Nonsurgical treatments can’t realign the out-of-place vertebra, but they can help you return to your daily activities without pain. Only surgery can restore your spine’s original alignment.
It can take anywhere from a few weeks to a few months to recover completely after spine surgery. Your surgeon will give you a customized recovery timeline based on your specific needs.
Most people with spondylolisthesis can resume sports and other physical activities after a few weeks of treatment. You’ll usually need to wait until you can safely move without pain.
Talk to your provider or surgeon before resuming any physical activities. They’ll suggest safe ways for you to stay active without increasing your risk of complications.
Your provider will tell you which kinds of activities are safe for you to do. You might have to avoid contact sports or intense physical activities that stretch or put a lot of stress on your spine.
You might not always be able to prevent spondylolisthesis, especially because sudden injuries or the way your spine forms can cause it. You can lower your risk with these tips:
The sooner you see a healthcare provider, the faster they can diagnose and treat spondylolisthesis. Visit a provider as soon as you notice back pain that lasts more than a few days or if you have pain that’s severe enough to stop you from doing your usual activities.
Go to the emergency room if you experience a trauma like a fall or car accident. Go to the ER if you lose feeling in your legs or can’t control your bladder or bowels.
You may want to ask your provider:
Spondylolisthesis and spondylolysis are similar conditions with confusingly similar names. The difference between them is how they affect your spine.
Spondylolisthesis happens when a vertebra slips out of place in your spine and presses on the vertebra below it.
Spondylolysis is a crack (a tiny bone fracture) between two vertebrae. Specifically, it’s a fracture in the pars interarticularis — the small ridges of bone that link your vertebrae together. Spondylolysis is one of the most common causes of isthmic spondylolisthesis. The crack between two vertebrae can make one slip out of alignment.
It’s always scary to hear that something is affecting your spine. Your mind might start racing when you hear that a bone is out of place in such an important part of your body. It’s completely natural to feel surprised or have lots of questions.
Take a second to catch your breath. Spondylolisthesis is hard to spell and pronounce, but (fortunately) not all conditions with complicated names require super-complex treatments. You might only need a few weeks of rest, OTC medications and some physical therapy. Even if you do end up needing surgery, you should be back to all your usual activities after your body has time to heal.
Low back pain can be a constant interruption in your daily life. Cleveland Clinic’s experts can help craft a treatment plan to help you find relief.

Last reviewed on 08/15/2024.
Learn more about the Health Library and our editorial process.