The myelin sheath is a protective membrane that wraps around part of certain nerve cells. Myelin also affects how fast signals travel through those nerve cells. Several diseases and conditions — multiple sclerosis being the most well-known — damage or destroy myelin. Ongoing research is aimed at protecting, repairing or regenerating myelin.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
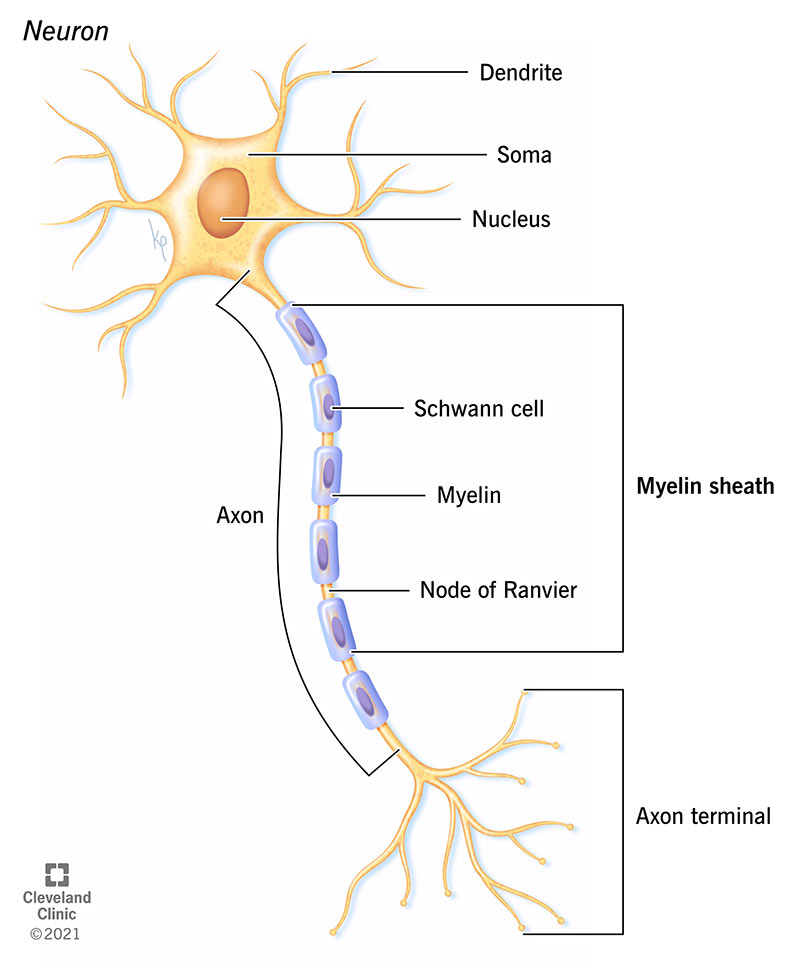
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22974-myelin-sheath)
A myelin sheath is a sleeve (sheath) that’s wrapped around each nerve cell (neurons). It’s a protective layer of fat (lipids) and protein that coats the main “body” section of a neuron called the axon.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A nerve cell is called a neuron. Nerves cells make up your nervous system. Your nervous system is your body’s communication command center. It sends and receives communication from all parts of your body and reacts to changes inside and outside of your body.
Each nerve cell has three sections. The sections of a nerve cell can be thought of like a tree.
Advertisement
The myelin sheath has three functions:
Myelin is made by oligodendrocytes in your brain and spinal cord (your central nervous system [CNS]) and by Schwann cells in your peripheral nervous system. Your peripheral nervous system is the network of nerves outside of your CNS. These nerves communicate between your CNS and the rest of your body.
Your myelin sheath isn’t one solid covering. It’s a lineup of individual sections of myelin, each separated from the next by a tiny gap — like the small amount of space you see between individual box cars on one long train. Each section of myelin is called an internode. Each gap in the myelin sheath — between internodes — is called the nodes of Ranvier. The nodes of Ranvier are rich in positive sodium ions. As the electrical signal or impulse travels along the axon, it jumps from one node to the next. When passing over the gap, the sodium ions recharge the electrical signal so it can continue in its travel without losing its charge or lessening in signal strength.
About 100 billion nerve cells are in constant activity, sending and receiving messages that control every aspect of your body’s functioning. When your myelin sheath on nerve cells is damaged, the electrical signal is slowed or stopped.
Myelin can be damaged when your body’s immune cells think that myelin is a foreign substance. Your body’s immune system produces inflammatory substances that damage myelin and eventually kill the cells (the oligodendrocytes and Schwann cells) that make myelin. The location where the myelin is attacked determines your symptoms. The destruction of the myelin sheath is called demyelination.
Probably the most well-known disease that attacks the myelin in your central nervous system (brain and spinal cord) is multiple sclerosis.
Other central nervous system (CNS) diseases in which myelin is attacked include:
Advertisement
Peripheral nervous system diseases in which myelin is attacked include:
What other conditions can damage or destroy myelin?
A myelin sheath can also be damaged or destroyed in adults by:
In addition, in a few rare inherited diseases, the myelin sheath doesn’t properly form. These diseases include Tay-Sachs disease, Gaucher disease, Hurler syndrome and Niemann-Pick disease.
Damaged myelin can be repaired in both your central and peripheral nerve systems. It’s important to manage the factors that cause demyelination such as inflammation and immune suppression/modulation treatment, including steroids, intravenous immune globulin (IVIG) and other agents.
Advertisement
Scientists are making progress in understanding potential ways to promote myelin repair. Although there have been several promising studies, it still isn’t clear if the benefits seen were meaningful improvements for individuals, and there are currently no approved medications for myelin repair. Here are only some examples of studies:
Advertisement
Myelin is an essential substance that keeps your nerves functioning, sending and receiving communication from all parts of your body. Without the100 billion functioning nerve cells, no part of your body would work. Many diseases and conditions can attack myelin — the best known is multiple sclerosis. Researchers continue looking for ways to protect, repair and regenerate myelin. The good news is that they’re making progress.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
If you have a neurological condition, you want expert advice. At Cleveland Clinic, we’ll work to create a treatment plan that’s right for you.
