The male sling procedure helps men with urinary incontinence (loss of bladder control). In the procedure, synthetic mesh-like tape is placed around the urethral bulb, compressing and moving the urethra into a new position. This treatment helps many men overcome urinary incontinence issues.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
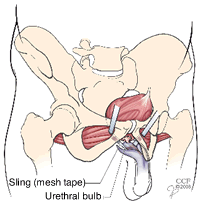
In the male sling procedure, synthetic mesh-like surgical tape is positioned around part of the urethral bulb, slightly compressing the urethra and moving it into a new position. The urethra is the tube through which urine exits the body. This procedure helps many patients with urinary incontinence.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The male sling procedure was developed to help men with urinary incontinence (loss of bladder control) after prostate surgery, particularly for those men requiring radical prostatectomy for prostate cancer. This procedure is best for men with mild to moderate urinary incontinence (wetting one to three pads per day or less).
Before surgery, your doctor may ask you to have a few tests. These tests may include:
Before surgery, you may be asked to see your family physician or anesthesiologist for a preoperative checkup. If necessary, your doctor will do a few tests. These tests could include:
You may also be asked to follow a few rules before surgery. These include:
Advertisement
During the male sling procedure, an incision is made through the perineal tissue (the area between the scrotum and anus). The surgeon will then expose the urethra and use a supportive sling (a mesh-like surgical tape) around part of the urethral bulb that covers the most upper part of the urethra close to where it enters the area of the urethral sphincter. By wrapping the surgical tape around the urethral bulb, the sling gently moves the urethra into a new position and increases resistance in this area. This lends support to the bladder neck. This procedure has been shown to help with mild to moderate urinary incontinence, and is most commonly used after radical prostatectomy.
The male sling procedure is usually performed as an outpatient surgery. However, there are some cases where patients will need to stay in the hospital overnight after surgery. The sling support requires absorbable sutures (stitches) in the perineum (the area between the scrotum and anus). This may cause some pain right after surgery, but overall, the amount of pain is usually mild and well tolerated.
The male sling procedure is not a major surgery. One of the advantages is that the male sling procedure only requires a small incision in the perineum (between the scrotum base and the anus). Because of this small incision, the recovery time is fairly short. Most patients have their catheters stay in for one to three days depending on surgeon preference.
Complications are rare with the male sling procedure. However, if complications do occur, they can include:
Following your surgery, you may have a catheter exiting from the urethra for a short period of time. The catheter is in place to allow you to empty your bladder since there may be swelling after surgery that makes it difficult to urinate. After the swelling goes down, you will gradually be able to urinate on your own and empty your bladder well. However, your normal pattern of urination may not return for a few weeks. You can resume a normal diet after surgery.
The majority of men undergoing the male sling procedure are either cured (pad free) or markedly improved afterward. Men who do not have a good result, or who have recurrent urinary leakage at a later date, are still good candidates for an artificial urinary sphincter (another device used to treat urinary incontinence after prostate surgery). Your doctor will discuss any additional procedures you may need in the future and will help develop a plan with you.
Advertisement
Last reviewed on 09/28/2019.
Learn more about the Health Library and our editorial process.