Trochanteric bursitis happens when something irritates a bursa near your hip joint. Bursae are small, fluid-filled sacs that cushion the bones and tissues around your joints. Trochanteric bursitis is a type of hip bursitis. A healthcare provider or physical therapist can show you exercises and stretches to help your hip heal.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
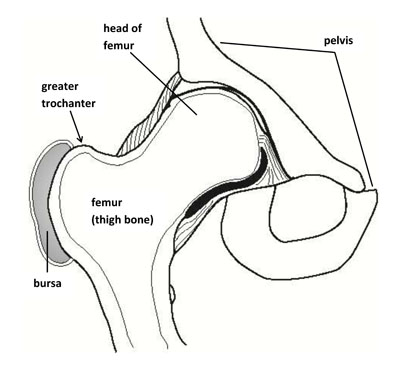
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/4964-trochanteric-bursitis)
Trochanteric bursitis is painful swelling near your hip joint. It’s a specific type of bursitis.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Bursitis is swelling in a small, fluid-filled sac called a bursa. Bursae (the plural of bursa) cushion spaces around bones and other tissue. They’re like bubble wrap that protects structures throughout your body.
Your hip joint is where your thigh bone (femur) connects to your pelvis. The pointed upper, outside edge of your femur is called the greater trochanter. Trochanteric bursitis happens when the bursa that covers your greater trochanter is damaged, inflamed or irritated.
Visit a healthcare provider if you’re experiencing hip pain, especially if the pain gets worse or doesn’t go away in a couple of weeks.
Hip pain is the most common trochanteric bursitis symptom. You might feel pain:
Anything that irritates or damages the bursa near your great trochanter can cause trochanteric bursitis. The most common causes include:
Advertisement
Anyone can develop trochanteric bursitis, especially after a fall or another injury. Some groups of people are more likely to experience bursitis, including:
People with certain health conditions have a higher risk of bursitis, including:
A healthcare provider will diagnose trochanteric bursitis with a physical exam. They’ll ask you about your symptoms and examine the area around your affected hip. Tell your provider what you were doing before you noticed symptoms for the first time and if any jobs or hobbies require you to do a repetitive motion or put stress on your hips.
Your provider might use some tests to diagnose bursitis, including:
Usually, rest is all you’ll need to treat trochanteric bursitis. Avoid the activity or positions that irritated your greater trochanter bursa.
Taking a break from activities that put pressure on your hip will give the bursa time to heal. Ask your provider how long you’ll need to rest and avoid certain physical activities.
Other trochanteric bursitis treatments include:
Trochanteric bursitis usually gets better after a few weeks to a few months of rest and treatment. You might have an increased risk of it coming back (recurring) if a repetitive motion or activity caused bursitis. Talk to your healthcare provider about ways to reduce stress on your hips.
Don’t ignore hip pain. You can increase your risk of making a small injury more serious if you put more stress on your hip before seeing a healthcare provider.
You might need to miss work or school while you’re recovering if a repetitive motion that’s part of your job or studies causes trochanteric bursitis. Tell your provider about your usual routine. They’ll explain which parts of it you need to modify or take a break from while you’re resting your injured bursa.
Advertisement
The best way to prevent trochanteric bursitis is to avoid overusing your hips:
Visit a healthcare provider if you’re experiencing pain that makes it hard to do your day-to-day activities. See a provider if you have hip pain that doesn’t get better in a week or two with rest and at-home treatments.
Technically, hip bursitis and trochanteric bursitis are the same condition. Trochanteric is a specific type of hip bursitis. It happens when the bursa that cushions the greater trochanter part of your femur is swollen. It usually causes hip pain.
Hip bursitis can also affect the other bursa in your hip joint — the iliopsoas bursa near your groin. Iliopsoas bursitis causes groin pain.
Trochanteric bursitis is swelling near your hip joint that makes it hard to move pain-free. The good news is that it usually gets better with a few weeks of rest. Talk to a healthcare provider as soon as you notice hip pain that doesn’t get better in a few days.
Advertisement
Your provider will help you find a combination of treatments that relieves your pain while your hip heals. They’ll also suggest ways to prevent future bouts of bursitis.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Bursitis can make your hobby or your job a real pain. Cleveland Clinic experts can help you find relief and get you back to doing the things you love.
