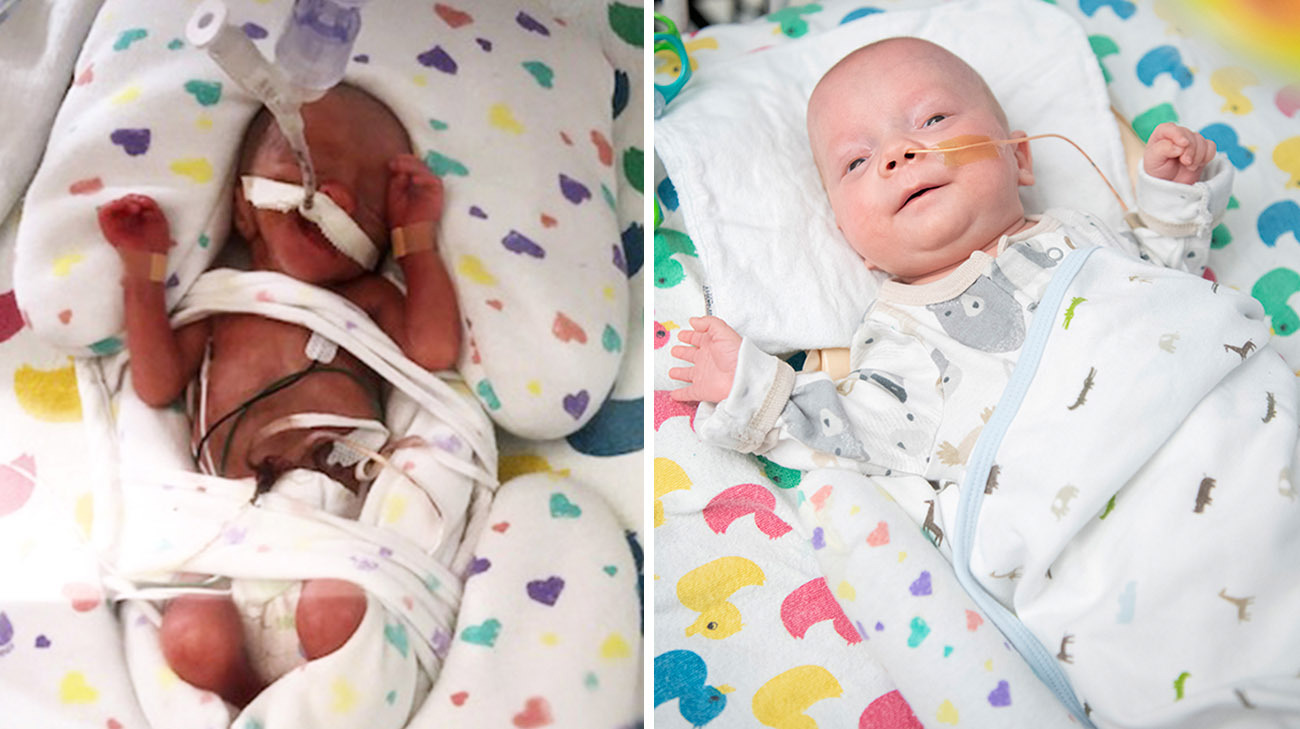
On the day he went home from the hospital, newborn Patrick LaFraniere weighed a hearty 7 pounds, 9 ounces. It’s a far cry from his weight on the day he was born: 1 pound, 3.7 ounces.
“When we brought him home, after 124 days in the NICU (neonatal intensive care unit), he was like a newborn in size,” says mom Meghan LaFraniere, two days after Patrick’s happy homecoming with his parents and three siblings. “It’s a miracle.”

Patrick meets his sisters and brother for the first time. (Courtesy: Meghan LaFraniere)
That joyful day was the culmination of a stressful and death-defying journey for Patrick and Meghan. Early in her pregnancy, she felt “different” and more tired than during her pregnancies with Elizabeth, 12, Lucille, 10, and Timothy, 3. Alarmingly, she experienced several instances of vaginal bleeding, which became heavier and more frequent as she approached 20 weeks gestation.
“At one point, the bleeding was so heavy I thought I’d miscarried,” Meghan recalls. “I was preparing myself that I’d lost him.” But Patrick was doing okay. An emergency room visit to Cleveland Clinic Fairview Hospital revealed the cause of the bleeding was placental abruption. It’s the premature and gradual separation of the placenta from the uterus before childbirth.
According to Jeff Chapa, MD, who specializes in maternal-fetal medicine at Cleveland Clinic, the condition can be life-threatening for baby and mother. Because the baby would not be viable if delivered at 20 weeks, and Meghan’s life was potentially in danger, Dr. Chapa presented her with all available options.
“In these situations, you really try to put yourself in (the patient’s) shoes and be honest with her,” explains Dr. Chapa. “She had to consider the risks involved, because her health as well as the baby’s could be compromised.”
Meghan was determined to move forward and delay Patrick’s birth as long as possible. “He was perfectly healthy,” she says. “I had to hold on.”
Meghan was admitted at Fairview Hospital, hoping constant monitoring and treatment would enable a safe birth, a few weeks later. Throughout her stay, Meghan received blood transfusions, as well as medications to help the fetus: corticosteroids, to speed lung development; and magnesium to prevent cerebral palsy and brain bleeds.
At just over 24 weeks, an ultrasound revealed a decrease in amniotic fluid and abnormal blood flow through the umbilical cord, signs the placenta was failing. It was no longer providing sufficient oxygen and nutrients to the baby through the umbilical cord. Adds Dr. Chapa, “The placental function had deteriorated to the point where we had to get the baby delivered.”
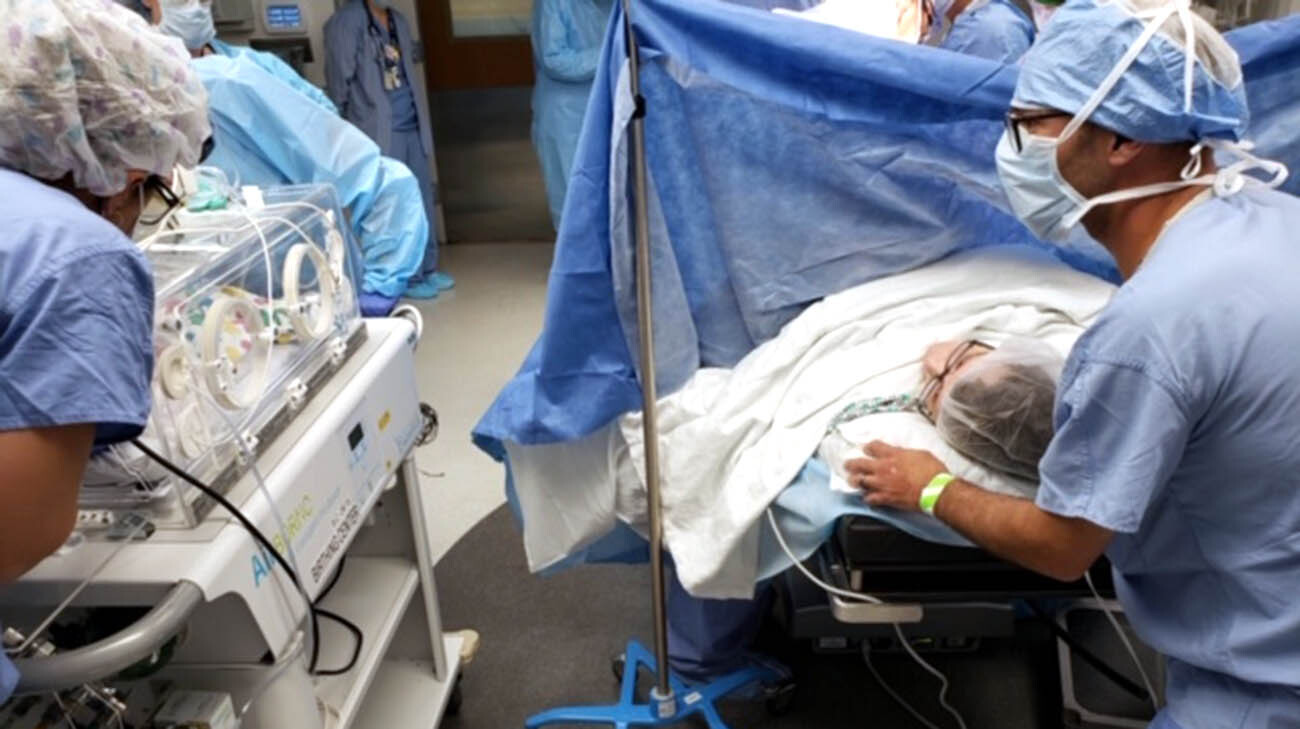
Meghan and Frank see Patrick for the first time. (Courtesy: Meghan LaFraniere)
Jennifer Stefanich, RN, a pediatric nurse, was one of several caregivers in the operating room for the delivery. As she recalls, Patrick was “so very small and fragile. He was right at our low limit, size-wise and gestationally-wise.”
At birth, Jennifer and the NICU team sprang into action, resuscitating Patrick and placing him in a plastic warming bag often used to reduce hypothermia in extremely low birth weight babies. “We’re taking him out of that nice, warm, safe environment in his mom, so we use the plastic bag to help maintain his temperature.”
Once in the NICU, the team inserted a tiny breathing tube into Patrick, since his lungs were underdeveloped, and placed him on a ventilator. Hydration and nourishment was administered through a special tube connected to Patrick’s belly button.
Meanwhile, Meghan recovered well from the birth and was discharged four days later. She and husband, Frank, made the journey to Fairview Hospital from their home, every day, to visit and help care for Patrick.
“We had to worry about his lungs, but everything else was functioning well,” recalls Meghan. “He was on a ventilator, and we couldn’t hold him for 15 days. But it was amazing when I finally got to.”
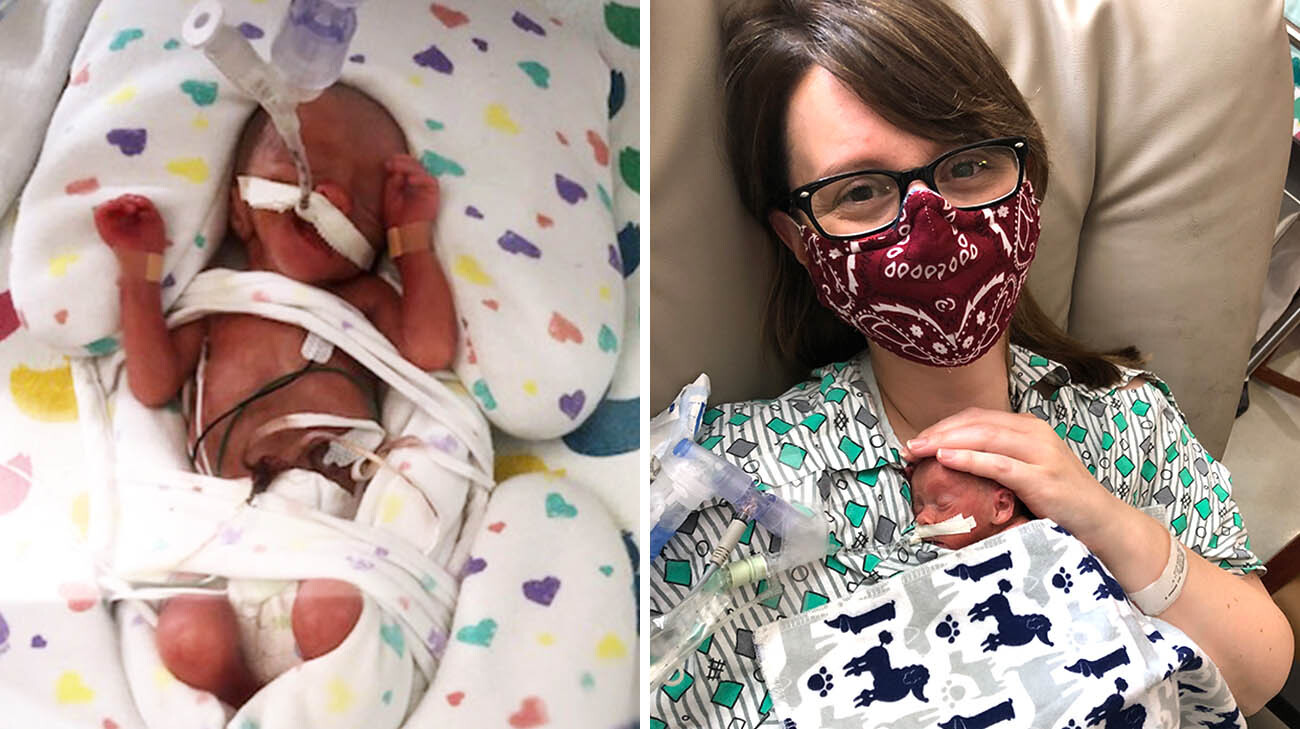
Patrick was on a ventilator during his first days in the NICU. (Courtesy Meghan LaFraniere)
Helping parents – even experienced ones like Meghan and her husband, Frank– care for a premature baby is a rewarding part of Jennifer’s job, “We’re used to seeing babies this small, but it’s shocking for the parents. We show it’s OK to touch them. It’s just that everything is so tiny.”
Meghan relied on the dozens of caregivers involved in Patrick’s care, including doctors, nurses, respiratory therapists, physical and occupational therapists, pharmacists and social workers. “They were there for me in my lowest moments, supporting me and taking care of Patrick and me.”

Frank holds Patrick in the NICU shortly before he was discharged. (Courtesy: Cleveland Clinic)
Meghan and Frank would spend hours at the hospital, holding Patrick and reading to him. His sister Elizabeth couldn’t visit due to COVID-19 restrictions. Instead, she gave Meghan books to read to Patrick, including a middle school-level favorite of hers, “The Seventh Most Important Thing.”
Those one-on-one moments had a palpable difference on Patrick, Jennifer says, “Just being able to be close to them was helpful. His color and oxygen levels improved. The babies that do well get held every day by their parents.”
Throughout Patrick’s four-month stay, Meghan and Jennifer bonded. “It was always fun to come in and work with her and chat. I would joke that I see Meghan more often than my own husband on a lot of days.”
When Patrick was ready to go home, Jennifer gave the family a crocheted baby blanket – adorned with orange pumpkins and fall colors – made by her mother-in-law, who asked that it be given to a special baby. “I’m so happy for them. Home is where the baby should be. But, golly, it’s tough. I miss him.”

Jennifer gives the family a crocheted baby blanket. (Courtesy: Cleveland Clinic)
The family is reveling in Patrick’s arrival. Meghan says, “His homecoming was beautiful. Four months old, and his siblings got to meet him! We’re feeling nothing but happiness.”
November is Prematurity Awareness Month, which focuses global attention on the 15 million babies born prematurely annually.
Related Institutes: Cleveland Clinic Children's , Ob/Gyn & Women's Health Institute

