A Nissen fundoplication is a surgery to treat gastroesophageal reflux disease (GERD). During the procedure, a surgeon wraps the top of your stomach around the bottom of your esophagus. This reinforces your lower esophageal sphincter to keep stomach acid from backing up into your esophagus.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
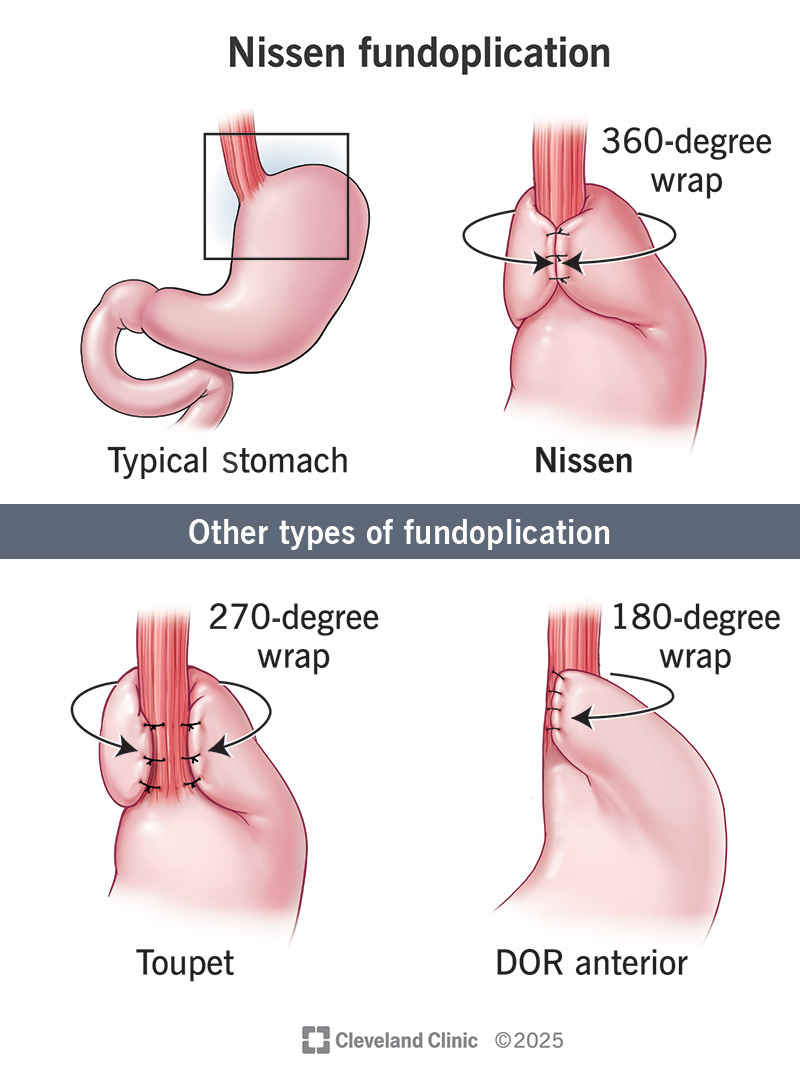
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/4200-nissen-fundoplication.jpg)
Nissen fundoplication is a surgery to treat gastroesophageal reflux disease (GERD). If you have GERD, the acid in your stomach flows back up to your esophagus. This can happen if your lower esophageal sphincter doesn’t work as it should.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Normally, your sphincter relaxes to let food move from your esophagus to your stomach. It then tightens to keep stomach acid out. A Nissen procedure wraps the top of your stomach (fundus) around the bottom of your esophagus. The wrap reinforces your lower esophageal sphincter so stomach acid stays where it belongs.
You or your child may have this surgery when other treatments don’t ease GERD symptoms.
The types of fundoplication vary depending on how much of your fundus wraps around the bottom of your esophagus. Your surgeon will explain the different procedures and recommend the one that’s best for your situation. The procedure types are:
Your surgeon may do tests to check for narrowing in your esophagus. They also check for hiatal hernias. A hiatal hernia is a bulge in your stomach at the top of your esophagus. It can worsen your GERD symptoms. Your surgeon will repair the hernia if you have one. Tests include:
Advertisement
Your surgeon will explain what you should do before your surgery. They may tell you that you or your child shouldn’t eat or drink anything after midnight on the day of your surgery.
You may have an open or laparoscopic surgery. You receive general anesthesia so you’re asleep during surgery. The details below describe a total Nissen fundoplication.
During open surgery, your surgeon:
During laparoscopic surgery, your surgeon:
A procedure typically takes one to three hours to complete.
The procedure eases your acid reflux symptoms when other treatments aren’t successful. Having a Nissen fundoplication also reduces your risk of developing Barrett’s esophagus. This condition can lead to esophageal cancer.
Like all surgeries, there’s a risk of infection. But the most significant risk of a Nissen fundoplication is that your symptoms may come back. You may need to have another procedure.
Common long-term side effects include:
The same procedure that keeps stomach acid out of your esophagus can keep you from throwing up. Your stomach dumps whatever’s upsetting it into your intestines. Eventually, the stuff leaves your body as poop.
Success rates vary depending on the type of procedure that you have. One study shows that 10% of people who had this surgery needed a second one.
You or your child may spend one or more days in the hospital after surgery. You or your child may:
Plan on taking it easy the first few days after surgery. Usually, you can get back to your daily routine after that. But talk to your surgeon if you have a strenuous exercise routine. They may recommend you do light exercise for a few weeks.
Advertisement
Kids who have a Nissen fundoplication may go back to school within a few days. They should avoid strenuous activities for at least three weeks. Ask your child’s surgeon if there are specific activities your child should avoid.
You or your child may have a sore throat after surgery. Your surgeon may recommend that you eat soft foods for the first seven to 10 days after surgery. Start with protein shakes and smoothies and work your way to yogurt, scrambled eggs and pasta.
Contact your provider if your incision bleeds more than you expect or if you have infection symptoms like:
You should also let them know if your symptoms come back after surgery.
You’ve tried medication and changing how and what you eat. And still, you’re coping with GERD symptoms that make you feel miserable and disrupt your daily routine. A Nissen fundoplication may help. The surgery keeps stomach acid from surging into your esophagus. The surgery can ease GERD symptoms or make them go away. If you’re living with GERD, talk to a healthcare provider. They’ll explain the surgery and discuss whether it’s an option for you.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Esophageal disorders can cause many symptoms, including heartburn or trouble swallowing. At Cleveland Clinic, we’ll find a treatment that works for you.
