Tympanoplasty is surgery to treat a ruptured eardrum. Having a rupture (hole) in your eardrum affects your ability to hear, and it can leave you exposed to germs that can cause ear infections. Often, ear drops and antibiotics can aid healing. But if this doesn’t work, you may need tympanoplasty so your provider can patch the hole.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
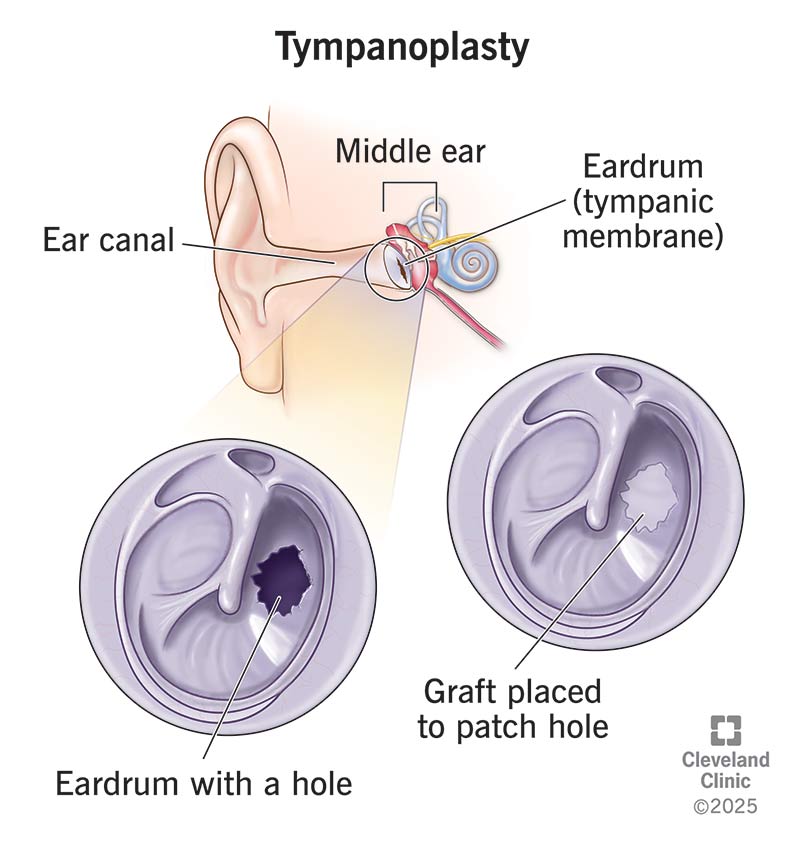
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/24406-tympanoplasty)
Tympanoplasty is surgery to repair a hole in your eardrum. Your eardrum is a membrane that separates your ear canal from your middle ear. It vibrates when sound waves strike it, making sounds louder so you can hear them. But having a hole keeps your eardrum from vibrating. This can make it harder to hear.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
You or your child may need this surgery if an injury or long-term ear infection tears this membrane. Small tears may heal without surgery with the help of ear drops or antibiotics. But if your eardrum doesn’t heal after two to three months, you may need tympanoplasty to prevent problems like hearing loss, more ear infections or ear drainage.
During this procedure, a specialist called an otolaryngologist (ENT) patches the hole in your eardrum. Although tympanoplasty is a major surgery, you’ll likely get to go home the day of your procedure.
Before surgery, your healthcare provider will review your medical history. They’ll check your middle ear and hearing. They may:
Your provider will also explain what happens during the procedure and tell you how to prepare. They’ll tell you:
Advertisement
Your healthcare provider will give you general anesthesia that puts you to sleep. You may also get antibiotics to reduce the chance of an infection.
Once you’re asleep, your provider will access your eardrum. The process depends on the tympanoplasty technique they use:
The next steps involve patching the hole with a graft. This means your provider will use tissue from a different part of your body to patch your eardrum. Sometimes, they use synthetic tissue. If they use tissue from your body, they’ll:
Tympanoplasty may take as little as 30 minutes up to several hours. It depends on how much damage there is inside your ear, how big the hole is and the technique they use.
Sometimes, the tiny bones behind your eardrum get damaged, too. If this happens, your provider will need to fix them. Sometimes, growths called cholesteatomas form behind a ruptured eardrum. Your healthcare provider may have to remove them. This adds to the total procedure time.
Tympanoplasty repairs your damaged eardrum. It can help restore your hearing. The patch also prevents germs from entering your middle ear and causing infections that lead to drainage from your ear.
And tympanoplasty complications are rare. The most common complication is graft failure. This means that the eardrum patch doesn’t solve the problem. Your eardrum may develop another hole during surgery, or your hearing may get worse.
Again, though, negative effects are uncommon. Studies show tympanoplasty successfully treats 90% of people. But this success rate depends on the size and location of the hole.
Most people go home after surgery. Or your healthcare provider may have you stay overnight at the hospital so they can make sure you’re healing OK.
Advertisement
Over the next few days, you may notice:
You may have moderate pain for the first few days after surgery. Most people manage it with over-the-counter pain relievers. But let your healthcare provider know if OTC medicines aren’t helping.
It can take 10 days to two weeks to recover from tympanoplasty. This means that the discomfort and surgery side effects have gone away. But it may take three or more months to get your full hearing back.
Keep a close watch on how your child is doing after tympanoplasty. If they’re feeling OK, they should be safe to return to school three to five days after surgery. Follow their healthcare provider’s guidance.
Follow your healthcare provider’s instructions about at-home recovery. Here are some general dos and don’ts after tympanoplasty:
Advertisement
You’ll see your provider about two to three weeks after surgery. They’ll look at your eardrum to see how it’s healing. Within two or three months, you may need to come back for your provider to check your hearing.
In the meantime, contact your provider if you notice:
Get emergency care if you have:
Anyone can rupture an eardrum. All it takes is going too deep — or with too much enthusiasm — when you clean your ears. Your eardrum can rupture if you develop a middle ear infection. Many times, a hole in your eardrum will heal on its own. But if it doesn’t, you may need tympanoplasty surgery to help you hear and stay connected to the world. Your healthcare provider will let you know if surgery is the best solution for you.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
A ruptured eardrum is treatable. Cleveland Clinic’s head and neck providers have the personalized ear care you need.
