With BCG treatment, your healthcare provider delivers immunotherapy drugs directly to your bladder through a catheter. Unlike oral or injectable drugs, BCG treatment targets cancer cells inside of your bladder without having a negative impact on the rest of your body. BCG treatment is the main immunotherapy used to treat early-stage bladder cancer.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
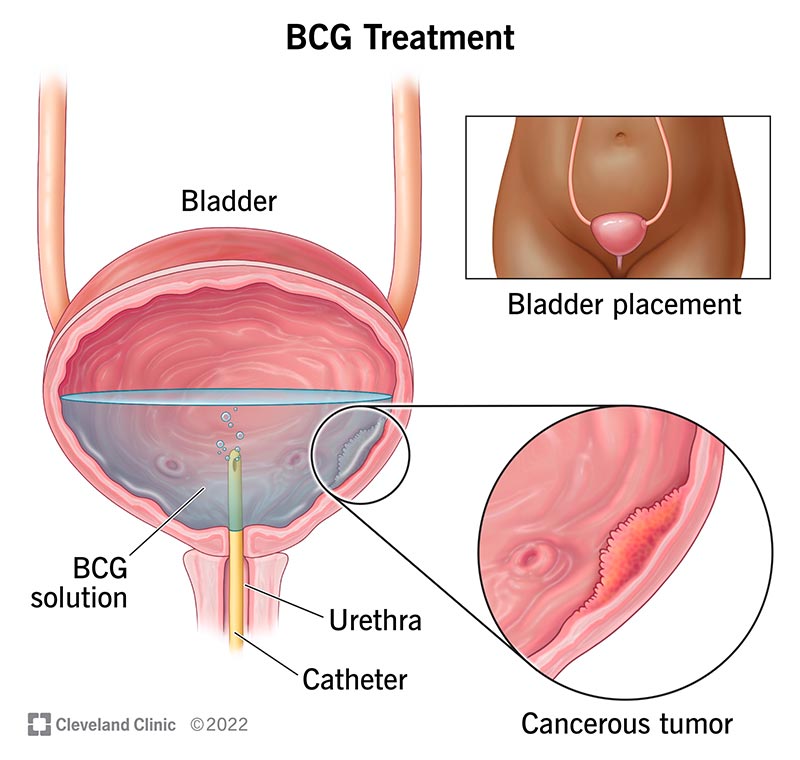
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/17908-bcg-treatment)
Bacillus Calmette-Guerin (BCG) treatment is a type of intravesical (in your bladder) immunotherapy. This liquid drug is made from a strain of Mycobacterium bovis — the same bacterium used to create the tuberculosis vaccine. When used in medicine, Mycobacterium bovis is weakened to reduce harm to your body.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
BCG treatment is usually given after TURBT (transurethral resection of bladder tumor), which is a bladder surgery to remove any visible cancer.
BCG treatment is used to address early-stage bladder cancer. This includes bladder cancers that haven’t invaded your bladder wall muscle, like carcinoma in situ (in its original location) bladder cancers and non-muscle invasive bladder cancers (NMIBCs). BCG treatment isn’t effective against bladder cancer that has metastasized (spread to other parts of your body).
Clinical trials are currently underway to explore BCG treatment for fibromyalgia and diabetes. Experts believe that BCG treatment may increase cytokines (immune-signaling molecules), which could potentially benefit people with these conditions. More research is needed in these areas, though.
No. Although intravesical immunotherapy and intravesical chemotherapy are given the same way, these two treatments use different types of drugs. While chemotherapy drugs attack cancer cells directly, immunotherapy drugs harness the power of your immune system.
BCG treatment is currently the most common intravesical immunotherapy used to fight early-stage bladder cancer.
Prior to BCG treatment, your healthcare provider will give you a list of specific guidelines to help you prepare. In general, you should avoid caffeinated beverages and diuretics (water pills) for four hours before your appointment. When you arrive for your procedure, you should pee to ensure that your bladder is empty.
Advertisement
Before beginning BCG treatment, local anesthesia is given to numb the area and keep you comfortable. Next, your healthcare provider will place a catheter into your urethra (the hole you pee from) and inject the liquid BCG solution into your bladder. When the process is complete, you’re free to leave your appointment. But you should avoid peeing for at least one more hour.
Once the BCG solution is injected into your bladder, you’ll hold it for a total of two hours. After this point, you’ll be able to pee.
When the BCG solution enters your bladder, your immune system cells begin to attack the cancer cells in your bladder.
The initial BCG cancer treatment occurs weekly for six weeks. This is called induction therapy.
If the treatment is working, your doctor may prescribe BCG maintenance therapy. Maintenance therapy is given once a week for three weeks at the three-, six- and 12-month marks. For some people, this may be continued up to three years.
Yes. The drugs used for BCG treatment contain live bacteria, which can be passed to other people. To reduce the risk of contamination, follow these instructions for six hours after every BCG treatment:
Typically, you’ll need to refrain from having sex for a few days after each BCG treatment session. In addition, use a condom any time you have sex throughout the entire course of treatment. Ask your healthcare provider about specific guidelines regarding sex.
When performed in combination with TURBT, BCG treatment is the most effective treatment for early-stage bladder cancer. BCG cancer treatment can slow tumor growth and reduce your chance of needing a cystectomy in the future.
It’s normal to develop certain side effects within the first 24 hours after BCG treatment. These side effects may include:
Your healthcare provider will give you medications to manage these side effects. You can also take over-the-counter (OTC) pain relievers to reduce fever and ease your discomfort.
Less commonly, you may experience additional complications, including:
Advertisement
If you develop severe pain, high fever or signs of infection, call your healthcare provider right away.
Most BCG treatment side effects go away in two to three days. If your symptoms are severe — or if they last longer than 72 hours — call your healthcare provider for guidance.
In general, most people can return to work or school in one to two days. But, everyone’s experience is different. Talk to your healthcare provider about what’s right for you.
Like most cancers, bladder cancer can potentially return after treatment. Statistically, cancer will recur (return) in up to 40% of people who receive BCG treatment. It’s important to note, however, that even if the cancer comes back, it may not progress.
Low-grade bladder cancer usually doesn’t spread to other areas of your body. But people who have low-grade bladder cancer have a higher risk of developing other low-grade cancers throughout their lifetimes.
Less often, aggressive bladder cancer can develop after BCG treatment. If this happens, cystectomy (surgery to remove your bladder) is usually recommended.
It’s normal to have a low-grade fever and mild achiness after BCG treatment. However, you should call your healthcare provider if you develop:
Advertisement
For people with early-stage bladder cancer, BCG cancer treatment is the go-to approach. Before deciding on treatment, talk with your healthcare provider about benefits, as well as potential risks and complications. A bladder cancer diagnosis can feel overwhelming. Consider joining a support group to get to know others who’re going through the same thing. Learning all you can about your treatment options can help you make an informed decision regarding your health.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Immunotherapy can take cancer treatments to new, powerful heights. And Cleveland Clinic is here to help with the latest advances.
