An oophorectomy is a surgical procedure where one or both of your ovaries are removed. This procedure can be done through a laparoscopic approach, a vaginal approach or a laparotomy. Removing both ovaries will cause menopause to begin immediately.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Video content: This video is available to watch online.
View video online (https://cdnapisec.kaltura.com/p/2207941/sp/220794100/playManifest/entryId/1_7746xkkj/flavorId/1_5f3sgelj/format/url/protocol/https/a.mp4)
Learn more about surgery to remove your ovary.
An oophorectomy is surgery to remove one or both of your ovaries. Your ovaries are reproductive glands that make hormones to control your menstrual cycle and promote bone and heart health. Ovaries also contain and help grow eggs that can lead to pregnancy. Women have two ovaries, one on each side of their pelvis. An oophorectomy is most commonly performed to treat a disease or reduce your risk of developing certain cancers.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
There are several different types of oophorectomies. Your surgeon will recommend one of these based on your medical history and symptoms:
An obstetrician-gynecologist (Ob/Gyn) typically performs an oophorectomy. You’ll get general anesthesia, so you are asleep for the surgery. Less often, the surgery is done under local or regional anesthesia, which means certain areas are numb and you’re awake.
A surgeon may remove one or both of your ovaries for several reasons, including:
Advertisement
You won’t be able to get pregnant naturally if both of your ovaries and fallopian tubes are removed. If your uterus remains, you can carry a pregnancy using technologies like IVF (in vitro fertilization). These are important factors to consider if you have a strong desire for children. There may be ways you can preserve your fertility before the procedure. For example, some people can freeze their eggs. Your healthcare provider may recommend you discuss your options with a fertility specialist.
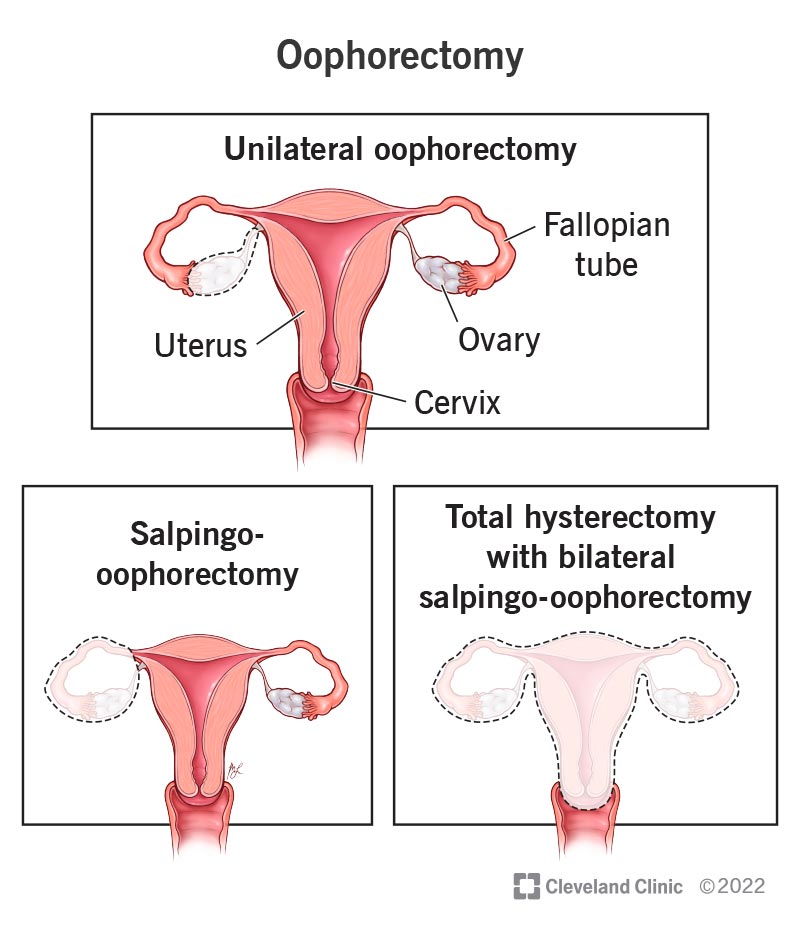
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17800-oophorectomy)
Your surgeon will review the procedure with you and go over any instructions for pre-and post-operative care. Make sure you understand the risks of surgery, the expected recovery time and how the procedure is performed. Before scheduling the surgery, your surgeon may ask you to have the following tests:
There are various ways a surgeon can remove an ovary. Each procedure carries its own risk and recovery time.
Laparoscopic and vaginal surgery may involve an overnight stay in the hospital, but can typically be performed as an outpatient procedure. This means you’ll return home several hours after surgery. A laparotomy (or open abdominal procedure) may require up to three days in the hospital. Everyone recovers differently, but you can expect three to six weeks of restricted activities. Your surgeon will schedule a follow-up appointment and discuss when you can resume your day-to-day activities.
Your body will go through different changes depending on the type of oophorectomy you had. If you haven’t reached menopause and had both ovaries removed, you’ll enter menopause immediately. Before surgery, talk to your surgeons about ways to prepare for the hormonal changes you may experience.
It depends on what type of oophorectomy you’ve had. If one ovary was removed and the other is still functioning, you’ll still get your menstrual period from the functioning ovary.
No, your ovaries can’t grow back.
An oophorectomy benefits people who have specific medical conditions or diseases, or people who are at higher risk of developing ovarian cancer. Getting an oophorectomy can treat or minimize symptoms of these diseases or conditions, and prevent ovarian cancer in certain high-risk individuals.
Advertisement
An oophorectomy, like any other surgery, carries some risks. These can include:
If your surgeon performs your surgery using laparoscopy or a vaginal approach, you may be able to leave the hospital the same day. If you had a laparotomy, you will spend a few days in the hospital. Before leaving the hospital, you will be told how to clean and care for your incisions.
Everyone heals at different rates, but generally, you can expect at least two weeks of restricted activities. In the case of a laparotomy, it may take up to six weeks until you can resume your normal lifestyle. Some general rules after surgery may include:
Advertisement
Removing one ovary won’t change your chances of becoming pregnant, assuming your other ovary and fallopian tube work normally. Removing both tubes and ovaries will mean that you’re not able to get pregnant on your own. You may need a treatment like IVF. People who have both fallopian tubes and ovaries removed and wish to have children should talk to a fertility specialist before the procedure about freezing eggs for future use.
Ovaries produce estrogen and progesterone, which help control the menstrual cycle. Removing both ovaries will cause menopause to begin immediately. It’s important to be prepared for symptoms of menopause before surgery.
In addition to no longer having periods, menopause can cause:
Your provider may treat you with hormone replacement therapy, depending on why the ovaries were removed.
Most people resume their normal routines two to six weeks after surgery. Hormone replacement therapy can help you deal with symptoms caused by menopause. Depending on your age and health history, your provider may discuss other ways to manage the side effects.
If you’ve had an oophorectomy, you should watch for these signs:
Advertisement
Contact your healthcare provider immediately if you experience these symptoms.
A hysterectomy is a procedure to remove your uterus. Your uterus is where a baby grows during pregnancy and where blood and tissue are shed during your menstrual period. A hysterectomy is often performed at the same time as an oophorectomy. An oophorectomy is a procedure to remove one or both ovaries.
An oophorectomy can be a scary procedure, especially if you’re not done having children or are worried about menopause or cancer. Talk to your healthcare providers about any concerns you have about the procedure and what you can expect afterward. They can help you cope with the side effects of an oophorectomy and how it may impact your life. Take time to understand the procedure and ask any questions you have. Your surgeon and healthcare team are there to help you.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
From routine pelvic exams to high-risk pregnancies, Cleveland Clinic’s Ob/Gyns are here for you at any point in life.
