An endovascular aneurysm repair procedure can save your life. Healthcare providers use tiny punctures to insert special devices called stent grafts. The grafts create a new lining for your artery, lowering the risk of a rupture.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
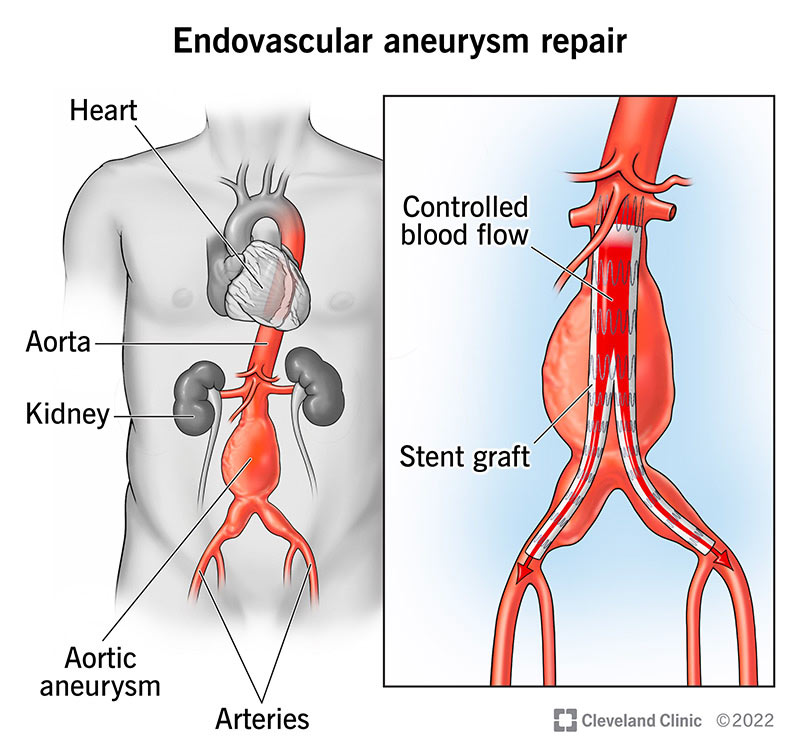
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22291-endovascular-aneurysm-repair)
Endovascular aneurysm repair (EVAR) is a minimally invasive procedure that can be used to manage abdominal aortic aneurysms. The aorta is the largest artery that carries blood from your heart to other parts of your body. For abdominal aortic aneurysms, EVAR uses small punctures and sophisticated instruments to repair bulges in blood vessels (aneurysms) located there.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The goal of endovascular aneurysm repair is to prevent the abdominal aortic aneurysm from bursting, which is a life-threatening event.
The force of blood flow against a weak spot in the wall of the blood vessel (here the aorta) causes the aortic walls to balloon outward, creating an aneurysm. This can lead to a burst, disrupting blood flow to your organs. Life-threatening complications can occur in minutes.
EVAR lowers the chances of a rupture by re-lining the aneurysm with a new tube, which takes the pressure off the aneurysm. The tube is called a stent graft, and it’s made of fabric with a metal mesh frame.
You may benefit from EVAR if you have an aortic aneurysm. Aortic aneurysms affect the body’s largest artery, the aorta.
Not all aneurysms need treatment. Your healthcare provider may consider EVAR if you:
Fenestrated endovascular aneurysm repair (FEVAR) is a specialized EVAR technique that repairs complex aneurysms. Your abdominal aorta is like a tree trunk that has many branches coming out of it. These branches are the arteries that carry blood to organs in your belly. If an aneurysm occurs near one of those branching points, it’s harder to treat. That’s where FEVAR comes into play.
Advertisement
FEVAR uses a fenestrated stent graft, meaning a graft with small openings. Those openings give rise to additional stent grafts that go into branching arteries. This special device fits the tree-like structure of your aorta and its branches. EVAR, by comparison, uses a graft that doesn’t have little openings for branches. It’s a standard tube shape.
Your provider will decide which procedure you need depending on where your aneurysm is located.
EVAR treats aneurysms in your abdomen (belly). Thoracic endovascular aneurysm repair (TEVAR) treats aneurysms in your thorax (chest). TEVAR is especially suited to treat aneurysms in your descending aorta – the part that moves down through your chest toward your belly. Aneurysms very close to your heart, in your aortic root or ascending aorta, usually require open surgery.
As a minimally invasive procedure, EVAR is gentler on your body. Benefits include:
Endovascular aneurysm repair is a safe procedure with a high success rate. But there’s always a chance of complications. These include:
If EVAR is right for you, here’s what to expect:
Advertisement
It takes days to months until you feel back to normal. Expect to stay in the hospital for a few days. You can start eating and drinking shortly after the anesthesia wears off. Nurses will help you get out of bed and start walking as soon as it is safe to do so.
Once you get home, you may tire easily and need pain medications for a few days. You shouldn’t drive until you are off pain medications. Most people return to work within a month. Avoid lifting anything heavy for four to six weeks after your procedure.
A small number of people experience issues with the implanted devices, like endoleaks. These can occur even years after undergoing endovascular aneurysm repair. Even with successful treatment, it’s possible to experience another aneurysm. Ongoing monitoring and imaging studies help healthcare providers determine whether additional treatments are necessary.
Contact your healthcare provider if you experience:
Endovascular aneurysm repair (EVAR) offers a less invasive option compared with traditional open surgery. You’ll have a shorter hospital stay and recovery. But you still need to care for your aorta and your heart after you’ve recovered. Lifestyle changes like exercising and reducing salt intake can help avoid future problems. It’s also important to keep all your follow-up appointments so your provider can check how your new stent graft is working and fix any problems if they come up.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When you come to Cleveland Clinic for aortic disease treatment, you’ll get industry-leading care and support from our heart and vascular specialists.
