Fibrocystic breast changes are a common noncancerous condition that can cause painful, lumpy breast tissue. Symptoms often fluctuate with your menstrual cycle or other hormonal changes. Most women don’t need treatment. You should always contact a healthcare provider if you have concerns about lumps in your breast or breast pain.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
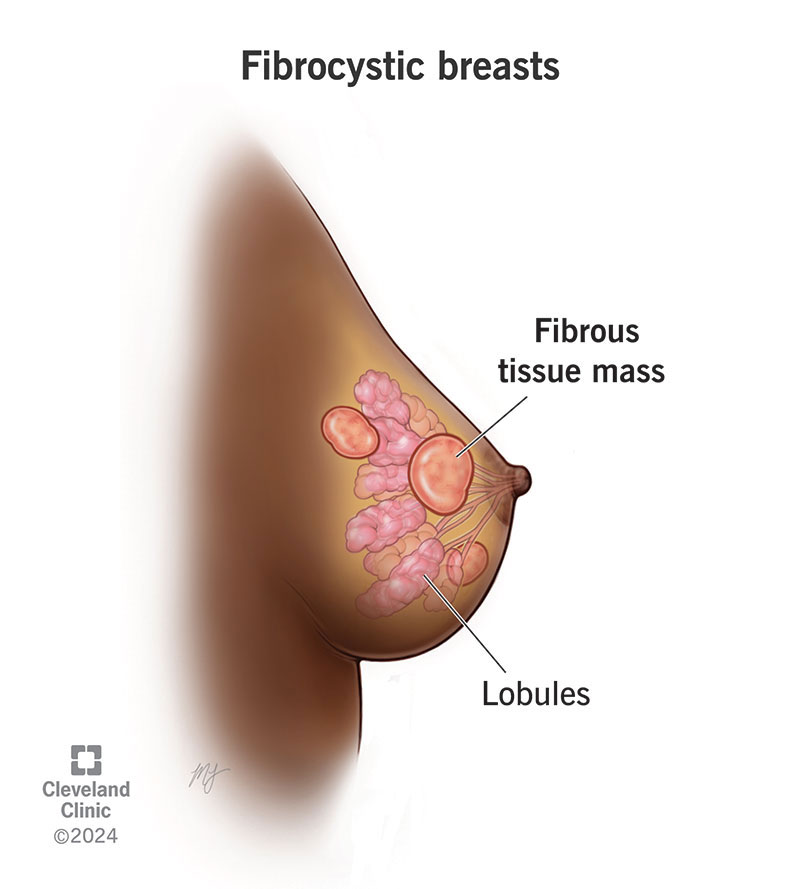
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22080-fibrocystic-breasts)
Fibrocystic breasts are a common, noncancerous condition that causes painful, lumpy breast tissue. These changes to your breast are usually harmless and don’t require treatment. Fibrocystic breast changes tend to be most noticeable just before your menstrual period when hormone levels fluctuate. Up to 50% of all females between ages 20 and 50 experience fibrocystic breast changes.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The lumps develop when fibrous tissue in your breast collects in one area, creating a mass. Fibrous tissue can be found in many parts of your body like your skin, joints and ligaments. Lumps can also form when fluid collects in a certain spot and creates a cyst.
The condition was previously called “fibrocystic breast disease,” but healthcare providers don’t use this term anymore for a couple of reasons. First, it’s common to have fibrocystic breast changes due to changes in hormones. Second, just because you have fibrocystic breasts doesn’t mean it’s a disease.
One of the best ways to identify changes to your breasts is getting to know them. Take time to regularly examine your breasts and look at their shape and size and how they feel when you touch them. You should also inspect your nipples and note their direction or if there is any discharge when you squeeze them. These steps are a great way for you to identify when something about your breasts seems different.
As changes to your breasts can be hard to identify on your own, it’s always a good idea to contact a healthcare provider if you notice any changes to them, such as new lumps, lumps that are getting bigger and breast pain that doesn’t go away. A provider can perform a clinical breast exam or order imaging tests to rule out other causes of breast lumps.
Advertisement
You may notice the following symptoms if you have fibrocystic breast changes:
For some women, the symptoms feel more intense just before their period starts. For others, the symptoms tend to stay about the same throughout their menstrual cycle. Still, others have very mild or unnoticeable symptoms. Fibrocystic breast changes can affect one breast or both breasts, too.
Lumpiness is the most common way to describe fibrocystic breast changes. Other ways to describe fibrocystic breasts may be rubbery, ropey (like there is a rope under your skin) or uneven. The lumps tend to be firm but can range in size. For example, some lumps can be the size of a raisin while others feel more like a grape. The lumps are also movable, so you can feel them move under your skin when you push them.
While experts aren’t entirely sure what causes fibrocystic breasts, they believe it relates to fluctuating levels of hormones — especially estrogen — during your menstrual cycle. Flare-ups of fibrocystic breasts tend to be most common just before your period when estrogen levels are lower.
Fibrocystic breasts can affect anyone, but it’s most common in before menopause. It’s rare to have fibrocystic breast changes after menopause unless you’re taking hormone replacement therapy.
Other factors may increase your risk of having fibrocystic breasts, but these factors are still up for debate in the medical community:
There aren’t any serious complications to fibrocystic breasts. These changes occur regularly and often coincide with hormonal fluctuations. There aren’t any studies that show fibrocystic breast changes increase your risk for cancer or contribute to breast cancer. The only correlation is that it might be harder to spot precancerous or worrisome breast tissue in fibrocystic breasts.
A healthcare provider can tell you for sure if you have fibrocystic breast changes or if your symptoms are or aren’t due to something more serious.
They’ll begin by asking about your symptoms and taking your full medical history. Then, they may perform all or some of the following:
Advertisement
If the lump is large, your provider may recommend draining the cyst (needle aspiration) to improve your symptoms. Your provider will use the findings from these tests to determine if further tests are necessary. Sometimes, they’ll want to perform a breast biopsy if a lump looks suspicious.
Masses can recur in women with fibrocystic breast changes. If you develop more masses in the future, tell your healthcare provider right away.
Most women don’t need treatment for fibrocystic breast changes. You can manage your pain at home and take steps to feel more comfortable. Some ideas to help you feel better are:
If your symptoms are predictable and follow your menstrual cycle, your healthcare provider may prescribe birth control pills to regulate hormone levels.
Advertisement
Vitamin E and evening primrose oil supplements may reduce breast pain in some women with fibrocystic breasts, but these treatment methods haven’t been fully studied. Talk to your healthcare provider before experimenting with supplements for breast pain.
Having fibrocystic breasts doesn’t change your lifespan or quality of life. In most cases, they aren’t a cause for concern. Most women find they can manage symptoms at home.
These types of breast changes alone don’t increase your risk of breast cancer. But it’s always a good idea to be sure that any breast changes aren’t cancerous or a sign of a serious health problem. Your healthcare provider is the best person to tell you if breast changes are concerning or normal. Be sure to visit your provider regularly and discuss your breast cancer risk. They’ll let you know how frequently you should be getting mammograms to check on your breast health.
Fibrocystic breast changes are normal and common. You can’t prevent it, but you can take steps to manage the symptoms it causes.
Any changes in your breasts should be brought to the attention of a healthcare provider to rule out serious issues. Contact them if you notice:
Advertisement
While fibrocystic breast changes and breast cancer share a few symptoms (like swelling and developing a lump), there are some distinct differences. Common symptoms of breast cancer that are uncommon with fibrocystic breasts are:
Your risk for breast cancer isn’t any higher if you have fibrocystic breasts. But changes in your breast tissue from fibrocystic breasts could make it slightly harder to detect tissue that may be cancerous. You should talk to your healthcare provider about your individual risk for breast cancer and see what they recommend.
Finding a lump in your breast or having breast pain can be alarming. It’s normal for your mind to think the worst. But not all changes to your breast mean something is wrong. Fibrocystic breast changes are normal and common and don’t increase your risk of breast cancer or other diseases.
Still, you should always inform a healthcare provider of any new growths or lumps in your breast tissue. They’re the best person to determine if changes to your breast should be checked out. The best thing you can do for your breast health is to get to know your breasts by checking their size, shape and texture regularly. Then, you’ll be more able to detect changes and alert your provider.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
From routine pelvic exams to high-risk pregnancies, Cleveland Clinic’s Ob/Gyns are here for you at any point in life.
