A third nipple, or a supernumerary nipple, is a fairly common condition in which you have an extra nipple. Researchers don’t know why they occur, but third nipples form during embryonic development. There are several different types. They usually aren’t a cause for concern, but your healthcare provider can remove a third nipple through surgery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
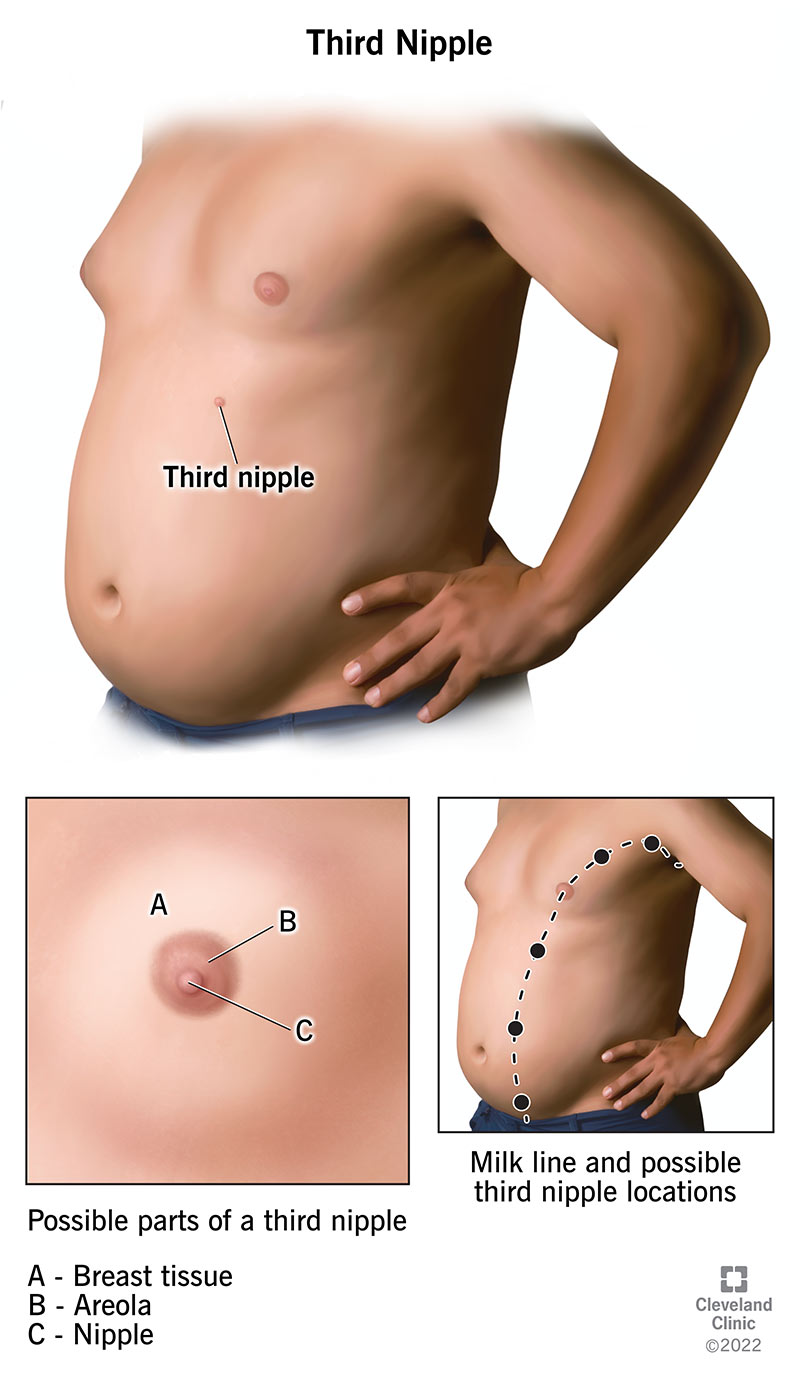
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/25167-third-nipple)
A third nipple is a condition in which you’re born with an extra nipple. Healthcare providers call this having a supernumerary nipple. You may also hear it called an accessory nipple or an ectopic nipple. While one extra nipple is the most common occurrence, you may have up to eight extra nipples.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Third nipples form during embryonic development. They most commonly appear along the milk lines (mammary ridges), which extend from your armpits down to your groin region. However, they sometimes appear in other areas of your body.
Third nipples are usually harmless and not a cause for concern. However, if you have one, you should keep up with regular checkups with your healthcare provider. That way, they can monitor your condition for any changes that may indicate an issue. Supernumerary nipples don’t usually require treatment, but your provider can remove a third nipple through surgery.
Healthcare providers classify supernumerary nipples based on their size, shape and tissue makeup. The main types include:
Advertisement
Supernumerary nipples can affect anyone. Humans develop milk lines during embryonic development. However, third nipples are less common in women than in men.
The rate of supernumerary nipples varies around the world. In Hungary, they affect less than 0.22% of the population. But in the United States, supernumerary nipples affect up to 6% of the population. Researchers estimate about 200,000 people living in the U.S. have one or more extra nipples.
A third nipple often looks like a birthmark or a mole. You may not even notice it. They typically appear on either side of the front of your body along your milk lines, where breast tissue could appear. These lines stretch from above your armpits down to your groin.
Most often, supernumerary nipples appear alone. They may look like small pink or brown bumps. But they’re usually much smaller than regular nipples.
Researchers don’t know the exact cause of third nipples. However, they typically form along the milk lines during early embryonic development. The milk lines run along both sides of your body from your armpits to your genitals. Breast tissue can potentially form anywhere along these lines.
During the fourth or fifth week of an embryo’s development, the milk lines begin to form from thickened skin tissue. Soon after, breast tissue starts to develop. As breast tissue continues to develop, the milk lines form your nipples and the rest of the thickened tissue softens up. When the milk lines don’t completely soften again, supernumerary nipples may form where the tissue stayed thick.
Third nipples usually appear along the milk lines, but about 5% of them form outside this area, along the skin on your neck, back, genitals, thighs or feet.
Most cases of supernumerary nipples are random. There have been some reports of the condition being passed down through families. In these cases, the condition appears to be inherited in an autosomal dominant pattern. However, researchers haven’t determined any kind of hereditary link.
Your healthcare provider will ask questions about your medical history and perform a physical exam. They’ll note the number of extra nipples you have and where they are on your body. They’ll also check for any abnormalities.
You don’t normally need to seek treatment for a third nipple, but it’s important to keep up with regular checkups to monitor for any changes. In rare cases, a third nipple can indicate an underlying medical condition. If you’re experiencing any of the following symptoms, reach out to your provider immediately:
You usually won’t need treatment for a third nipple. They typically aren’t a sign of any underlying medical conditions. However, some people opt for third nipple removal for cosmetic reasons or if they’re causing pain or discomfort.
Advertisement
A healthcare provider can perform a noninvasive surgery to remove your third nipple. The surgery is normally quick and fairly painless. Your provider will likely use a local anesthetic to numb the area. Then, they’ll make a few cuts (incisions) in the area and remove the nipple.
You may experience some swelling after the surgery. This should go away within two weeks. You may also develop a red or brown scar in the area that could take up to two years to thin and brighten.
Supernumerary nipples are usually harmless and not a cause for any concern. If they’re bothering you, you can speak with a healthcare provider about removal.
In rare cases, a third nipple is a sign of an underlying medical condition. These may include:
You can’t prevent a third nipple because it’s a condition that forms during embryonic development. Researchers don’t know the exact cause.
You should see your healthcare provider if your third nipple is causing you pain or discomfort. You should also check in with them if the area around the nipple hardens, forms new lumps or develops a rash. In addition, you should report any abnormal discharge to your provider.
Advertisement
You should get regular physical exams and let your provider know if you develop any changes in your extra nipples. This allows them to monitor for signs of potential complications.
Having a third nipple, or a supernumerary nipple, is more common than you think. These typically harmless extra nipples form during embryonic development. While they’re usually not a cause for concern, you should see your healthcare provider so they can monitor you for any changes that may indicate an issue. You usually don’t need treatment for a supernumerary nipple, but your provider can remove it through a noninvasive surgery.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s primary care providers offer lifelong medical care. From sinus infections and high blood pressure to preventive screening, we’re here for you.
