Macrocephaly means your baby’s head is larger than other babies of the same age and sex. Having a larger head size can be harmless, if a larger head size is a family trait, or it can be a sign of a serious medical condition. Common medical conditions include an enlarged brain, brain bleed, fluid on the brain and genetic disorders. Treatments are specific to the cause.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
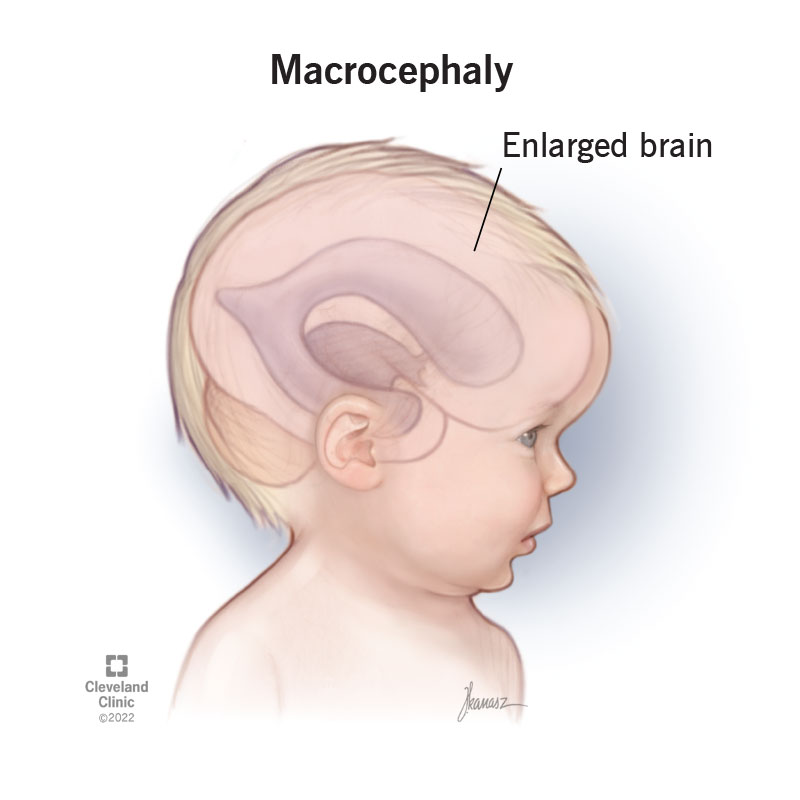
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22685-macrocephaly)
The term macrocephaly means “large head.” If your infant has macrocephaly, they have a head circumference that’s much larger than others of the same age and sex. Technically, your child’s head circumference (measurement around the widest part of their head) is greater than the 97th percentile. This means their head is larger than 97% of children of the same age and sex.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Macrocephaly can be a sign of a condition that requires treatment. However, your baby’s larger head size might also be something that runs in your family, and is harmless and doesn’t need to be treated. This condition is called benign familial macrocephaly.
Macrocephaly is diagnosed in about 2% to 5% of the U.S. population.
Common signs and symptoms include:
If your child has benign familial macrocephaly, they won’t have symptoms other than an unusually large head circumference.
Causes of macrocephaly range from benign (harmless) to severe. If your child has benign familial macrocephaly, they simply have a larger-than-normal-sized head. Their larger head size is inherited and is similar to the head size of another family member.
However, there are other, more harmful causes of macrocephaly, some are congenital (born with), while others may develop over time. These include:
Advertisement
Your healthcare provider can determine if your baby has macrocephaly before they’re born by reviewing the results of routine ultrasound tests done late in your second trimester or early in your third trimester.
Your child’s healthcare provider will measure your baby’s head circumference during each well-child visit, up to the first five years of life. Your child’s healthcare provider will compare your child’s head size to an expected growth chart of children of the same age and sex. They’ll also consider the head size of birth parents and grandparents.
If macrocephaly is found, the next step is to determine the cause. Their healthcare provider will perform several types of exams and tests.
During a neurologic exam, your child’s healthcare provider will:
During a physical exam, in addition to measuring your child’s head circumference, your healthcare provider will look for:
Advertisement
Imaging tests may include:
Complications include:
Treatment depends on the underlying cause.
Advertisement
If your child has a larger-sized head but has otherwise met normal developmental milestones and a normal neurologic exam, the macrocephaly is often harmless and the outcome is good. No treatment is needed. This is usually the case if your child is diagnosed with benign familial macrocephaly.
If your child has macrocephaly due to an underlying cause, what to expect depends on the specific cause. Your child’s treatment plan will be specialized for them.
Macrocephaly is a term that means “large head.” The word doesn’t denote a harmful condition. A large head can be a completely normal and healthy condition if a large head size is typical in your family. Your child’s healthcare provider will determine if a medical condition is causing the macrocephaly.
There’s nothing that can be done to prevent macrocephaly. However, there are treatments to help manage many of its causes.
Contact your child’s healthcare provider right away if you notice:
Advertisement
These symptoms could mean that your infant's condition could be changing and your child’s healthcare provider will want to investigate and determine if treatment is needed.
Here’s a simple chart of average head circumference increase by age:
| Age of child | Average centimeter increase in head circumference |
|---|---|
| 0 to 3 months | 2 centimeters/month |
| 3 to 6 months | 1 centimeter/month |
| 6 months to 1 year | 0.5 centimeters/month |
| Total during the first year of life | 12 centimeters |
| 1 year to 3 years | 1 centimeter/6 months |
| 3 years to 5 years | 1 centimeter/year |
| 1 centimeter = 0.39 inch | |
| Age of child | |
| 0 to 3 months | |
| Average centimeter increase in head circumference | |
| 2 centimeters/month | |
| 3 to 6 months | |
| Average centimeter increase in head circumference | |
| 1 centimeter/month | |
| 6 months to 1 year | |
| Average centimeter increase in head circumference | |
| 0.5 centimeters/month | |
| Total during the first year of life | |
| Average centimeter increase in head circumference | |
| 12 centimeters | |
| 1 year to 3 years | |
| Average centimeter increase in head circumference | |
| 1 centimeter/6 months | |
| 3 years to 5 years | |
| Average centimeter increase in head circumference | |
| 1 centimeter/year | |
| 1 centimeter = 0.39 inch | |
| Average centimeter increase in head circumference | |
Macrocephaly is a broader term. It simply means an unusually large head. It includes megalencephaly as a possible cause. Megalencephaly is a distinct term that means an unusually large brain.
This condition, also called benign external hydrocephalus, means there’s a small amount of fluid between your infant’s brain and skull. It’s very common in children with large heads. It usually doesn’t require treatment. Your child’s healthcare provider will closely follow your child. Usually, children outgrow this condition.
Macrocephaly is a word that means your baby has a larger than normal head circumference. Macrocephaly is often present at birth. The cause can be harmless if you have other family members with larger heads and there aren’t any other signs or symptoms present. But macrocephaly can also be a sign of a serious condition. Your child’s healthcare provider will do a careful physical and neurologic exam and order any necessary imaging tests of your child’s head. Based on the findings, your child’s healthcare provider can determine the cause and develop an appropriate treatment plan.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
If you have a neurological condition, you want expert advice. At Cleveland Clinic, we’ll work to create a treatment plan that’s right for you.
