Bronchospasms happen when the muscles that line the airways in your lungs tighten. It causes wheezing, coughing and other symptoms. Many things cause bronchospasm, including asthma. Medications can usually manage bronchospasm. If you’re having symptoms, call 911 or go to the nearest ER.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
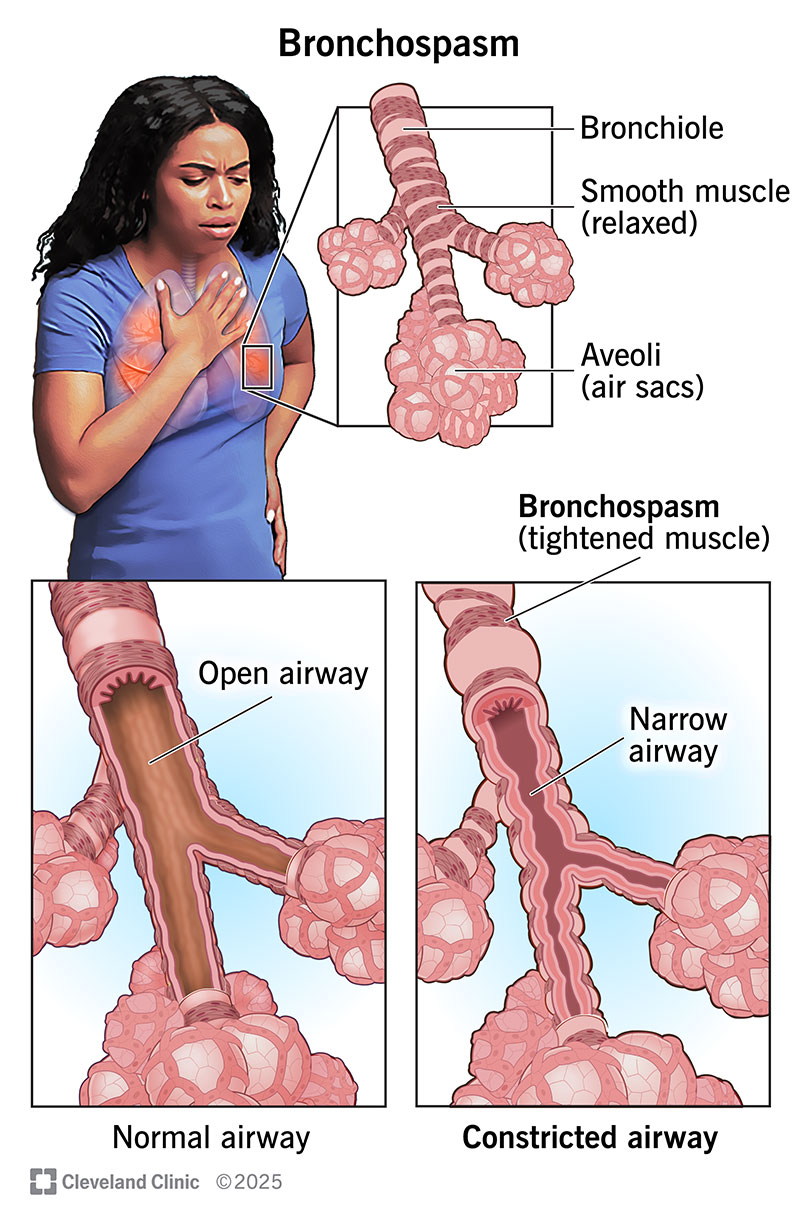
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/bronchospasm)
A bronchospasm (pronounced “BRONG-kuh-spaz-uhm”) is when the muscles that line your bronchi tighten. Your bronchi are the tubes that air travels through to get to your lungs. They connect your windpipe (trachea) to your lungs. If the muscles in your bronchi tighten or squeeze, your airways narrow. This limits how much oxygen your body receives. Bronchospasms can occur alongside many different lung conditions, including:
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
They can be scary because it feels like you can’t get enough air to breathe. Go to the nearest emergency room if you have sudden or severe breathing problems.
The main symptom of bronchospasm is the feeling that you can’t catch your breath. Other bronchospasm symptoms include:
Asthma is the most common cause of bronchospasm. But many other things can also cause irritation and swelling in your airways. Irritation and swelling can cause bronchospasm. These include:
Just because you have a condition or are around a trigger, it doesn’t mean you’ll have a bronchospasm. In rare cases, bronchospasm medications like albuterol can actually make your symptoms worse. This is a paradoxical bronchospasm. If this happens, stop using your bronchodilator immediately and tell your healthcare provider. They’ll work with you to find a different treatment.
Advertisement
No, bronchospasms aren’t contagious. But some bronchospasm causes are contagious, like bacterial or viral infections.
A healthcare provider can diagnose bronchospasm. They’ll review your medical history, ask about your symptoms and perform a physical exam. During the exam, they may listen to your lungs with a stethoscope. If they think you’re having bronchospasms, they may refer you to a pulmonologist or allergist.
Healthcare providers listen to your lungs with a stethoscope. Stethoscopes pick up very quiet sounds. When they use one, they listen for high-pitched whistling sounds.
Your healthcare provider may recommend pulmonary (lung) function tests to see how well your lungs work. These may include:
Depending on your history, your provider may also recommend:
Bronchospasm treatment usually starts with bronchodilators. Bronchodilators are available as inhalers, nebulizer solutions and tablets. There are short-acting bronchodilators and long-acting bronchodilators.
Short-acting bronchodilators offer quick “rescue relief” for bronchospasm symptoms. They can widen your airways in a matter of minutes. The effects can last up to six hours. Common short-acting bronchodilators are albuterol and levalbuterol.
Long-acting bronchodilators reduce your risk of bronchospasms in the future. Except for formoterol, they don’t offer quick relief. But they last for up to 12 hours. Other common long-acting bronchodilators include salmeterol and vilanterol. Providers may use formoterol for rescue or quick relief instead of albuterol or levalbuterol.
Other forms of long-acting bronchodilators include anticholinergics. They’re available as short-acting inhalers (ipratropium) and long-acting inhalers (tiotropium, umeclidinium, aclidinium). They’re also available as nebulizers (glycopyrrolate, revefenacin).
Providers commonly prescribe inhaled steroids, too. Inhaled steroids help reduce inflammation in your airways and prevent bronchospasm. In cases of severe bronchospasm, go to the ER or a hospital. They may give you steroids as a pill or through a peripheral IV if they can’t manage your symptoms.
Advertisement
There aren’t any home remedies that can stop a bronchospasm once it starts. You need a short-acting bronchodilator to ease the symptoms of an attack. You likely have a bronchodilator if a provider has diagnosed you with bronchospasm. But if this is your first bronchospasm and you don’t have a bronchodilator, go to the nearest ER for treatment.
Some providers believe breathing exercises can reduce your risk of bronchospasm. But research is ongoing, and it needs more evidence. Even so, breathing exercises can’t stop a bronchospasm once it has started.
If you get bronchospasms, your provider will tell you how to best manage them.
Get to the ER or call 911 if you have bronchospasm symptoms and don’t have a bronchodilator. Symptoms may include:
Contact your provider if you develop bronchospasm symptoms that linger. You should also reach out if your symptoms affect your daily activities.
If a provider diagnoses you with bronchospasm, they’ll likely prescribe a short-acting bronchodilator. You use this in case of an attack. They may also prescribe you a long-acting bronchodilator along with an inhaled steroid. This helps reduce your risk of bronchospasms in the future. Bronchodilators alone won’t prevent future bronchospasms.
Advertisement
How long a bronchospasm episode lasts can vary. It depends on the underlying cause, severity and your response to treatment. Episodes can last minutes to days. Bronchodilators can help you manage your symptoms during this time.
Yes. Without treatment, severe bronchospasm can be fatal. But with quick treatment, your symptoms will usually go away within minutes. If you develop bronchospasm symptoms, use your bronchodilator as soon as possible. If you don’t have a bronchodilator and can’t breathe, call 911 or go to the ER.
No, you can’t prevent bronchospasm. But you can help reduce your risk by:
Your provider may also recommend that you use bronchodilators before you exercise.
Bronchospasm is a symptom of asthma and other conditions. People with asthma can get bronchospasm. But not everyone with bronchospasm has asthma. Bronchospasm and asthma result from irritated or inflamed airways.
Advertisement
No. Bronchospasm and bronchitis are similar but not the same. Bronchitis is when inflammation causes your bronchi and windpipe to swell and fill with mucus. It may cause bronchospasm. But not everyone who has bronchitis has bronchospasm.
Bronchospasm episodes are alarming, especially the first time you have one. But medications can reduce your risk and ease your symptoms should one occur. They can also help many people enjoy active lifestyles. Talk to a healthcare provider if you have asthma, COPD or other respiratory conditions that make you more likely to have bronchospasms.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Breathing issues can affect your life in many ways. Cleveland Clinic’s respiratory therapy program treats your symptoms so you can feel better day to day.
