Oligohydramnios is when you have low amniotic fluid during pregnancy. Your healthcare provider diagnoses low amniotic fluid using an ultrasound. Oligohydramnios can cause pregnancy complications or be a sign of an underlying health condition. Treatment depends on how far along you are in pregnancy and how low your amniotic fluid is.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
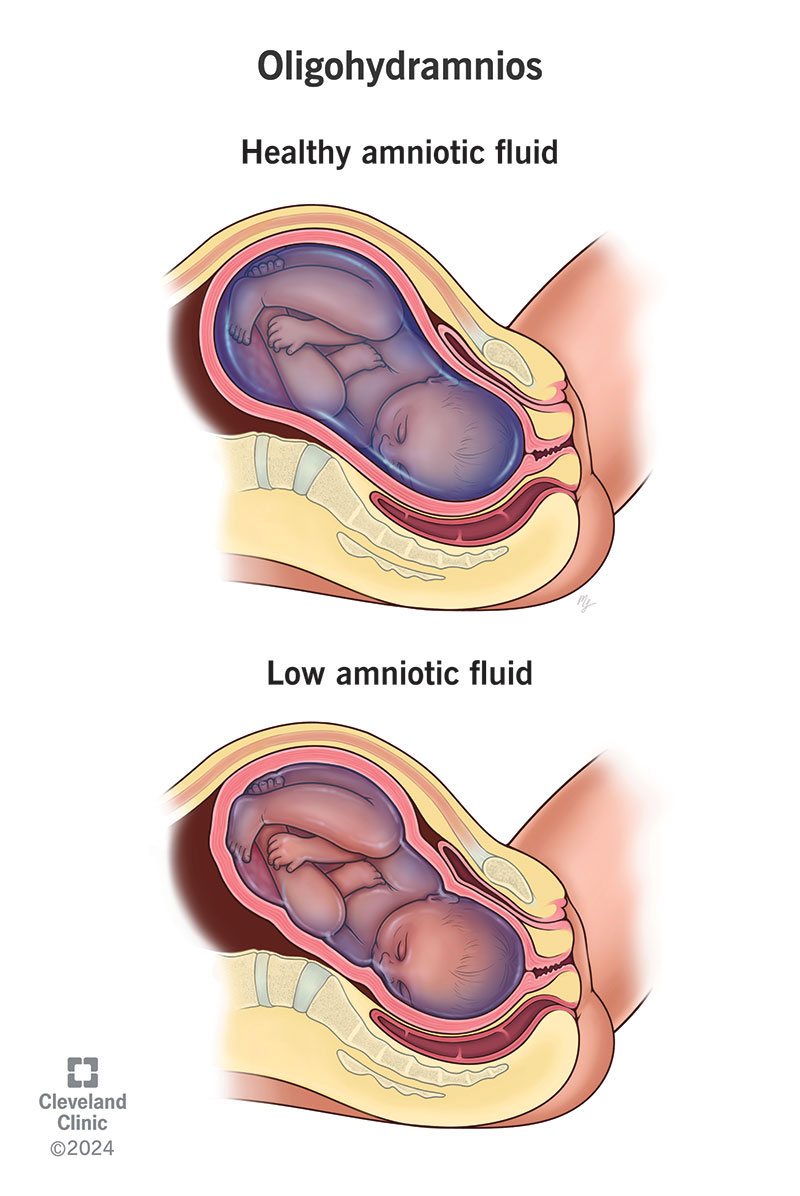
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22179-oligohydramnios)
Oligohydramnios is a condition during pregnancy when your amniotic fluid is lower than it should be. Amniotic fluid is a water-like fluid that surrounds a fetus during pregnancy. It protects it from infection and umbilical cord compression and cushions their movements. Amniotic fluid also helps develop a fetus’ digestive and respiratory system, as well as regulate its temperature.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Too little amniotic fluid can cause health issues in the fetus or be a sign of an underlying problem in the pregnancy. These conditions could affect fetal development or cause complications during labor and delivery.
Often, you don’t know your amniotic fluid is low. This is typically detected on ultrasounds being done for other reasons, like measuring a fetus’ growth. It can come as a surprise, and you may find yourself worried about how this will affect your pregnancy. Try not to panic. Most people with low amniotic fluid will deliver healthy babies. Treatment depends on how far along you are in pregnancy and if you have other pregnancy complications.
Low amniotic fluid affects about 4% of women during pregnancy. It’s most common in the last three months of pregnancy (third trimester). This rate rises to about 12% if you go past your due date because amniotic fluid levels tend to decline to low levels past that point.
It depends on how many weeks pregnant you are. You begin making amniotic fluid about 12 days after conception. Early in pregnancy, the amniotic fluid comes from the placenta. Starting at around 15 weeks, the amniotic fluid is pee from the fetus. The amount of amniotic fluid you produce increases until its peak at 36 weeks of pregnancy. After that, your levels of amniotic fluid start slowly decreasing. The amount of fluid in your uterus at any time will fluctuate as the fetus drinks the fluid and produces more pee.
Advertisement
You may not know you have low amniotic fluid. However, your healthcare provider may suspect it if:
Often, the cause of low amniotic fluid is unknown. It can happen randomly in a healthy pregnancy. But other times, your healthcare provider can link low amniotic fluid to a specific cause.
Some possible causes of oligohydramnios are:
Having any of the above conditions or risk factors can make you more likely to have low amniotic fluid levels. You’re also at higher risk for low amniotic fluid if you’ve had low amniotic fluid in prior pregnancies.
Low amniotic fluid in the first six months of pregnancy is generally more dangerous. These complications could include:
If you receive an oligohydramnios diagnosis in the last trimester (weeks 28 to 40) of pregnancy, complications could include:
Your pregnancy care provider measures the amount of amniotic fluid in your uterus a few times during pregnancy using an ultrasound. If the amount of fluid is less than the recommended amount for the gestational age of the fetus, you may have oligohydramnios.
There are two ways to measure amniotic fluid: amniotic fluid index (AFI) and maximum vertical pocket (MVP).
It depends on how far along you are in your pregnancy and if you have other pregnancy complications. If you’re close to full term (37 weeks of pregnancy), your healthcare provider may decide that inducing labor is the safest option for your baby.
Advertisement
Your healthcare provider will schedule extra prenatal visits to monitor you closely and make sure the fetus is growing. These visits could include:
Other treatment options depend on the cause of the oligohydramnios. If there is concern for ruptured membranes or if the fluid is persistently low, you may need to go to the hospital for close monitoring.
Maybe. Some studies show that drinking water can help increase amniotic fluid levels in women who are pregnant.
Yes, your baby will likely be born healthy. Low amniotic fluid can be serious, but in most cases, babies do well after birth.
There isn't anything you can do to prevent oligohydramnios. Attend all prenatal check-ups and be upfront with your healthcare provider about your symptoms and medical history. Knowing if you’re at risk for low amniotic fluid is your best chance for diagnosing and treating the condition.
Call your healthcare provider if you experience any of the following:
Hearing you have low amniotic fluid can be shocking and leave you with lots of questions. What does this mean for my baby? Can you fix it? These are all valid questions. But try to remain calm — most people with low amniotic fluid go on to have healthy babies.
Advertisement
Your healthcare provider will monitor you closely throughout the rest of your pregnancy. They’ll work with you to determine the safest treatment plan. Their goal is for both you and your baby to be healthy. Attending all of your prenatal appointments and sharing your pregnancy symptoms is the best way for your provider to detect potential issues with amniotic fluid volume.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Worried about your high-risk pregnancy? Want the best maternal and fetal health care? Look no further than Cleveland Clinic. We’re here for all your needs.
