Elephantiasis is an infectious disease that spreads through mosquito bites. It can lead to fluid retention and, in some cases, disfigurement. Elephantiasis is common in many tropical and sub-tropical climates. It’s very rare in the United States.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Elephantiasis (pronounced “eh-luh-fuhn-TAI-uh-suhs”) is a type of infectious disease that causes skin thickening and (in some cases) disfigurement. You get elephantiasis through tiny parasitic worms (filarial worms) that infect your lymphatic system. These parasites block your lymphatic capillaries and cause fluid (lymph) to accumulate.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
People with elephantiasis may also develop inflammation, swelling and fever. Without treatment, elephantiasis can cause health complications.
Another name for elephantiasis is lymphatic filariasis (pronounced “fil-ur-AI-uh-suhs”).
About 120 million people worldwide — 1.5% of the world’s population — have a lymphatic filariasis infection. The condition is most common in tropical climates. Countries in Asia, Africa and South America have higher cases.
Elephantiasis is rare in North America. The worms that cause it don’t live in the United States.
It’s rare to get an elephantiasis infection during a short visit to one of these countries. You’re more likely to get the condition if you stay in a high-risk area for months or years.
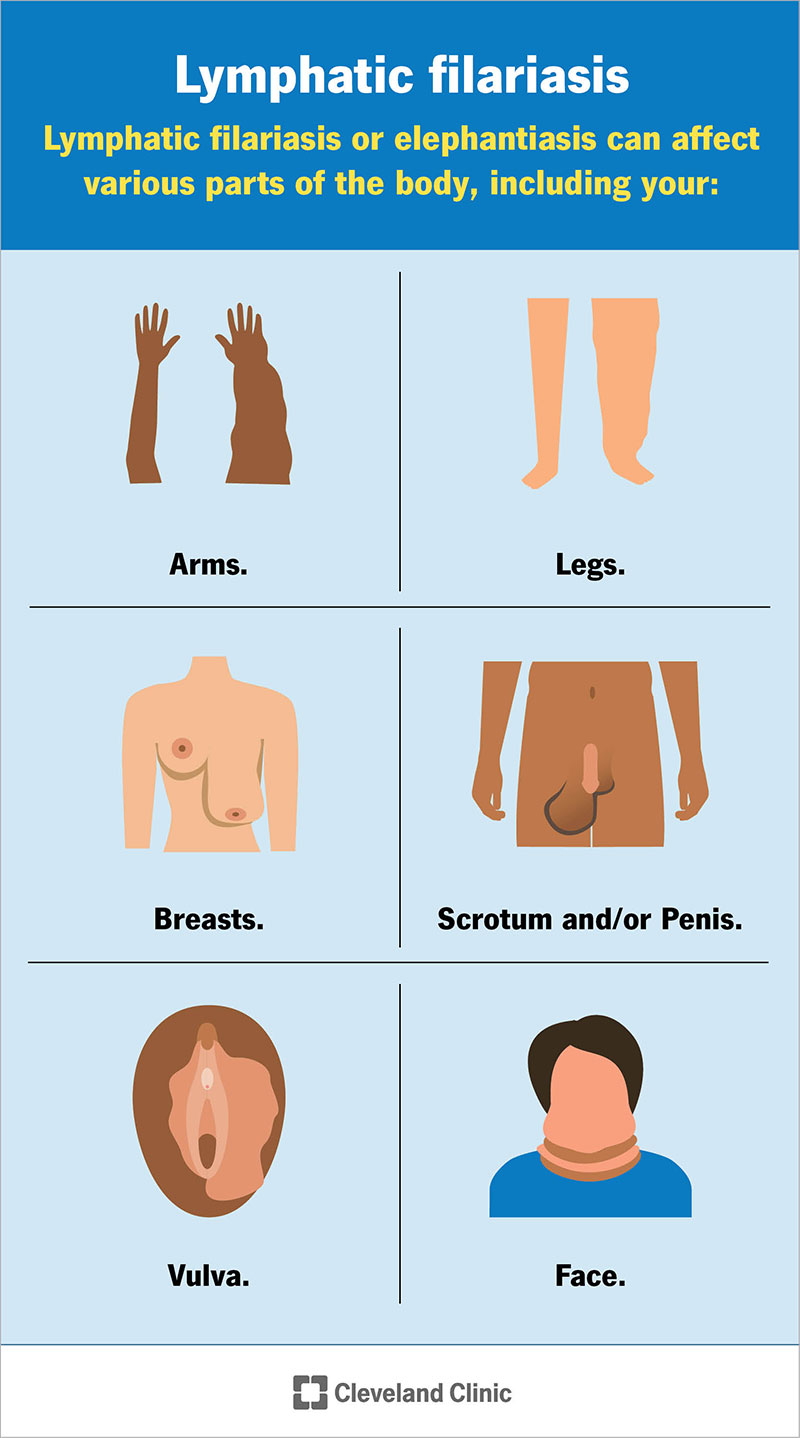
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/elephantiasis-lymphatic-filariasis.jpg)
About 2 in every 3 people who have lymphatic filariasis don’t have severe symptoms. But filariasis usually leads to a weakened immune system.
Some people may experience:
Elephantiasis can affect various parts of the body, including your:
Advertisement
Elephantiasis can occur when a person has filariasis — a parasitic infection by a type of roundworm. Tiny worms, too small to see with the naked eye, invade your body. Under a microscope, the filarial worms look like threads.
There are several types of filarial worms:
Lymphatic filariasis spreads through mosquito bites. When a mosquito bites someone who has filariasis, the filarial worms in the person’s blood infect the mosquito. Then, when the infected mosquito bites another person, the worms pass into that person’s bloodstream.
In general, a person won’t get filariasis from a single mosquito bite. It usually takes repeated mosquito bites over several months (or even years) for a person to get the condition.
When these worms enter your bloodstream, they travel to your lymphatic system. There, they grow into adult worms. The adult worms stay alive for up to seven years. The filarial worms reproduce and release millions of worms into your bloodstream.
Over time, damage to your lymphatic system may make it difficult for your body to fight infections. Because of this lowered immune response, you may develop:
To diagnose elephantiasis, healthcare providers need to examine a blood sample. They may use:
Your treatment plan varies depending on what symptoms you have and how severe they are. In general, elephantiasis treatment may include:
Advertisement
If you’re taking filariasis medications, you need careful monitoring from a healthcare provider. Antiparasitic drugs can lead to severe side effects, including:
There isn’t a cure for lymphatic filariasis. Medication can kill many of the worms and keep you from spreading the infection to someone else. Treatment can also reduce your symptoms.
People with elephantiasis often experience negative social impacts. If they have very visible, severe symptoms like extreme swelling, they may experience social stigma. Chronic swelling or pain may also impact a person’s ability to work. While elephantiasis has no cure, you can manage the condition and reduce its symptoms.
The best way to prevent elephantiasis is to avoid mosquito bites, particularly in tropical areas. If you live in or travel to places where a filariasis infection is possible, take the following steps to prevent mosquito bites:
In parts of the world where filariasis is common, the World Health Organization (WHO) recommends treating whole regions with preventive chemotherapy. With this prevention strategy, people at risk of infection take an annual dose of specific chemotherapy drugs.
Advertisement
The medications have a small effect on adult worms but can keep younger worms from reproducing. They can also prevent the parasites from spreading to mosquitoes.
If you develop unexplained swelling or thickening of your skin — particularly in your arms, legs, breasts, scrotum or vulva — let a healthcare provider know. They can run tests to confirm or rule out a diagnosis.
You may also want to ask your healthcare provider:
Even if medication kills the filarial worms, you can still develop lymphedema. To manage lymphedema symptoms, you can:
Elephantiasis is common in sub-tropical and tropical climates, where filarial worms thrive. It usually takes repeated bites from infected mosquitos for a person to get the condition. So, most cases occur in people who live in high-risk regions. It’s rare for short-term tourists to get elephantiasis. Still, if you develop symptoms, it’s important to tell a healthcare provider. A simple blood test can confirm whether you have a parasitic infection.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Have a virus, fungus or bacteria? Some of these “bugs” won’t go away on their own. Cleveland Clinic’s infectious disease experts are here to help.
