Mania is a spike in mood and activity that lasts at least a week. You may feel wired, need little sleep, talk fast or take big risks. It’s common in bipolar disorder. A healthcare provider can help you manage it with medications, therapy and support.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
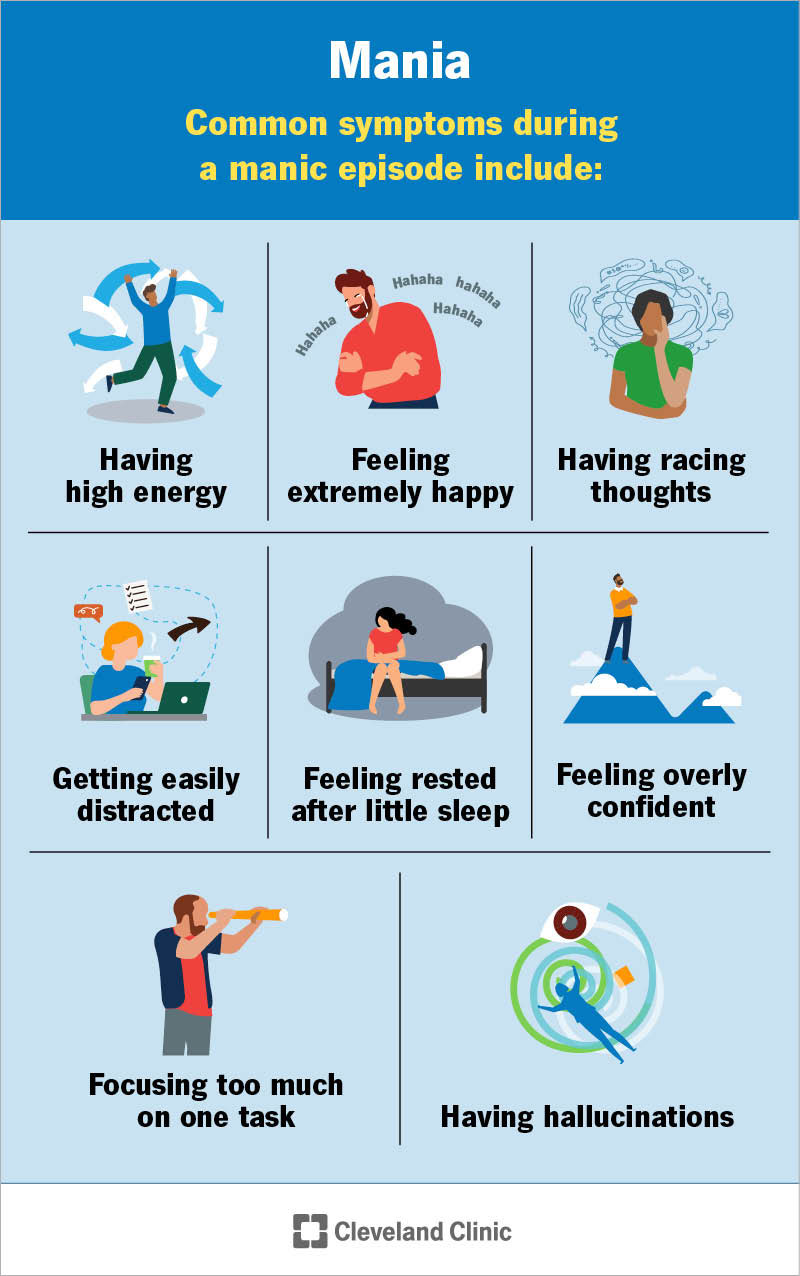
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/mania)
Mania is when your mood, energy or activity level becomes much higher than usual. You may feel overly excited, irritable or full of energy. You might not feel like you need much sleep. You may take risks or act on impulses without thinking them through.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
These changes are different from how you usually feel and act and are noticeable to people around you. Mania often happens in bipolar disorder, but it can occur in other conditions, too.
A healthcare provider can help you manage this symptom and its underlying cause.
A manic episode is a period when your mood, behavior and energy level become much higher or more intense than usual. These symptoms last most of the day, almost every day, for at least one week.
In some cases, the symptoms can be severe enough that you may need hospital care. Sometimes, hospital care is the safest way to help you rest, reset your mind and keep you safe while symptoms improve.
Healthcare providers don’t use specific “types” of mania to make a diagnosis. Still, they may describe your symptoms in the following ways:
Advertisement
During a manic episode, it can be hard to notice the symptoms yourself. People close to you may see the changes first. Common signs of mania include:
Mania feels different for everyone. Common symptoms during a manic episode include:
After a manic episode, you may feel:
Scientists aren’t completely sure what causes mania. Research shows it likely develops from a mix of genetic, psychological and social factors. Experts are still studying how these factors work together.
Possible causes include:
You may be more at risk of developing mania if you have:
Certain things can make a manic episode more likely to happen. These are known as triggers. Common triggers include:
Advertisement
Manic episode triggers are different for each person. You may need to look closely at your mood and behavior to learn what affects you. Keeping a mood diary can help you track how you feel before and during an episode. You can also ask trusted family members or close friends to help. They may notice changes in your behavior sooner than you do.
Knowing your triggers may help you prepare for an episode.
Many cases of mania are linked to an underlying mental health disorder, including:
Your provider can help you understand which condition fits the symptoms you have.
A healthcare provider will ask about your medical history and your family's medical history. They’ll also ask about any prescriptions, over-the-counter medicines, herbal products or supplements you take.
Your provider may order blood and urine tests or imaging scans to rule out conditions that can cause mania. Once conditions are ruled out, your provider may refer you to a mental health specialist.
To diagnose mania and its underlying cause, a mental health provider will compare your symptoms to the criteria in the Diagnostic and Statistical Manual of Mental Disorders, 5th edition. The criteria include:
Advertisement
A healthcare provider may offer medications and therapy to help manage mania. Treatment is unique to each person and may change over time.
Common mania medications include:
If these medications aren’t effective, your provider may try:
Each medication comes with possible side effects. Your provider will let you know what these are so you can watch for them. Let your provider know if you’re pregnant or plan on starting a family. Some medications may cause birth defects.
Advertisement
Your provider may recommend talk therapy to help you understand mania, its cause and learn healthy coping skills. Different types of therapy may support you in different ways:
A manic episode lasts at least seven days. It can continue for several weeks or even months. Some episodes last three to six months. Treatment may shorten the length of an episode.
You can’t always prevent mania. But you can make a plan to manage symptoms early and keep them from getting worse.
Early signs, also called prodromal symptoms, are the first changes you might notice. Your mood may shift, your sleep pattern may change or your energy may slowly increase.
Here are some steps you can try during this time:
You should seek immediate medical care if you notice:
You should also contact your provider if you:
Tell someone right away if you have thoughts of harming yourself. Contact family, friends, your provider or the Suicide and Crisis Lifeline at 988 (U.S.). Someone is available 24/7.
Mania can be confusing — for you and the people around you. When your energy shoots up, sleep fades away and your mind feels like it’s moving a mile a minute, it can seem exciting at first — or really uncomfortable. Either way, it’s a sign that your brain is in overdrive.
If your symptoms feel intense, scary or out of control — especially if sleep disappears for days, or you’re seeing or believing things that others don’t — reach out for help. Getting care quickly can shorten an episode and keep you safe. That might mean calling your provider, going to an emergency room or calling/texting 988 if you’re worried about hurting yourself.
Mania is treatable, and many people find a plan that helps them feel steady again.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Your mental well-being is just as important as your physical well-being. Cleveland Clinic’s mental health experts can help you live life to the fullest.
