Keratosis pilaris is a common condition where small bumps develop on your skin, especially your arms, legs or butt. Excess keratin in your skin causes bumps to form. This condition is harmless and typically doesn’t need treatment, and usually fades by age 30. Treating dry skin with a gentle skin care routine can help.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
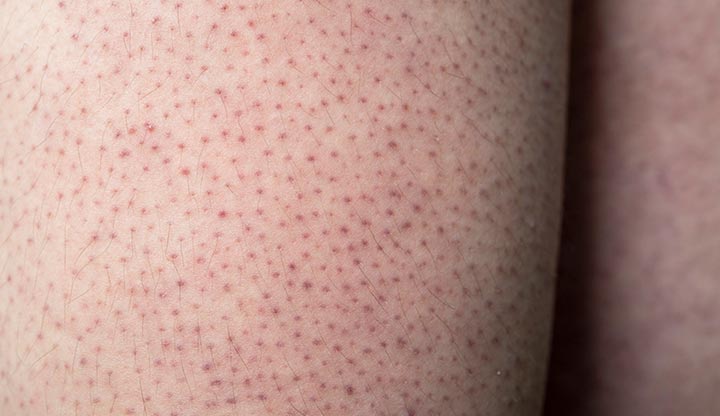
Keratosis pilaris is a benign (not harmful) skin condition that looks like small bumps. If you have this condition, you may notice small, painless bumps on your skin around hair follicles. The bumps consist of excess keratin, which is a protein that helps form your hair, nails and skin’s outer layer (epidermis). Keratosis pilaris bumps may look red, brown or white, or they may look the same color as your skin. Other names for keratosis pilaris include KP or “chicken skin” because it looks like goose bumps.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Keratosis pilaris typically appears on your upper arms, but it can also appear on any other part of your body that has hair follicles.
Keratosis pilaris is typically more common in babies, toddlers, children and teenagers, and it often worsens around puberty.
You’re more likely to have keratosis pilaris if someone in your family has it. As a result, healthcare providers and medical researchers believe that certain genetic traits may cause it.
You’re also more likely to have keratosis pilaris if you have:
Keratosis pilaris is so common that many dermatologists consider it a skin type instead of a medical condition. About 50% to 80% of teenagers and 40% of adults will develop these bumps at some point during their lives.
Keratosis pilaris causes small, discolored bumps to develop around your hair follicles. The palms of your hands and soles of your feet don’t have hair follicles, so keratosis pilaris won’t appear in these areas of your body.
Keratosis pilaris doesn’t hurt, but it may make you feel self-conscious or insecure about your appearance.
Advertisement
The main feature of keratosis pilaris that you’ll notice is patches of tiny, rough, discolored bumps on your skin that resemble the dotted skin of a strawberry. You may notice the appearance of the bumps but don’t have any other symptoms. If you do experience symptoms, they may include:
Other conditions can sometimes cause these symptoms, such as itchy, dry skin. Eczema, psoriasis, allergies and fungal infections cause similar symptoms. If you’re concerned about your symptoms, or if they linger, it’s a good idea to contact your healthcare provider.
The bumps you see when you have keratosis pilaris are actually collections of the protein keratin. These bumps are sometimes mistaken for clusters of small pimples. Keratosis pilaris bumps happen when keratin clogs (blocks) your pores instead of flaking off. Your pores are openings in your skin where hairs come through your skin (hair follicles).
Healthcare providers don’t know why keratosis pilaris affects some people and not others. There could be a genetic factor, meaning your genes could affect your chances of developing this condition.
If you have a skin condition like eczema, you’re more likely to get keratosis pilaris. Eczema is a common chronic skin condition that causes your skin to have discolored, itchy patches that come and go over time.
Keratosis pilaris may have a link to vitamin A deficiency. Taking vitamin A supplements or using moisturizers or creams with small amounts of vitamin A may help treat keratosis pilaris.
Keratosis pilaris isn’t contagious. Out of the many types of skin bumps and growths you may develop, keratosis pilaris is a harmless one.
Your healthcare provider will typically diagnose keratosis pilaris with a simple physical examination of your skin where you have bumps. Keratosis pilaris is easy to recognize, so medical testing isn’t usually necessary. The location and characteristics of the bumps can help you identify whether you have keratosis pilaris. But if your healthcare provider isn’t sure, they may conduct an allergy test or a biopsy.
Keratosis pilaris bumps most often show up on your arms — especially your upper arms. However, they can appear wherever hair follicles are on your body, including your:
Advertisement
How your skin bumps look and feel can reveal a lot about their cause. Keratosis pilaris bumps are:
In most cases, your family doctor can diagnose keratosis pilaris. Some people may see a dermatologist to treat their keratosis pilaris.
Keratosis pilaris isn’t harmful, so you usually don’t need to treat it. For some people, the bumps go away on their own or become less noticeable by about age 30. You may also notice that the bumps go away in the summer and only become noticeable in the winter.
If the bumps bother you, treatment with moisturizers, creams and gentle skin care may help your symptoms.
Treatments your healthcare provider may recommend can include:
Dry skin can make keratosis pilaris worse. Applying an over-the-counter moisturizer keeps skin hydrated, minimizing and softening the bumps. Apply moisturizer several times each day, especially after showering while your skin is still damp. Moisturizers with ammonium lactate and alpha hydroxyl acids, such as AmLactin® or CeraVe SA® cream, are the best choices for rough, bumpy skin and people with keratosis pilaris.
Advertisement
Your healthcare provider can tell you if prescription-strength moisturizers may be right for you. The ingredients urea, alpha hydroxy acids, salicylic acid and glycolic acid can sometimes improve the look of keratosis pilaris. Medicated vitamin A creams, such as Retin-A®, can help decrease the buildup of keratin that causes keratosis pilaris. Be careful not to use too much. Overuse of these medicated creams can irritate your skin.
Use a loofah, washcloth or exfoliating gel or scrub and small, circular motions to gently wash the affected areas of your skin while you shower or bathe. Make sure not to scrub too hard. Scrubbing can irritate your skin and make your symptoms worse.
Laser treatments can help improve the discoloration associated with keratosis pilaris. Dermatologists perform laser treatments.
Most people find their keratosis pilaris improves when they change their routine to avoid dry skin. Changes can include:
Home remedies won’t make your keratosis pilaris go away, but they can help your affected skin look healthier, which may minimize the appearance of bumps.
Advertisement
Though home remedies are safe for most people, it’s a good idea to check with your healthcare provider before trying some of the following options. You may be at risk of developing an allergic reaction.
Keep in mind that these keratosis pilaris treatments are temporary. You’ll need to continue treatments to see continued improvements. Some people don’t see any benefit from treatment. Fortunately, keratosis pilaris isn’t harmful, only annoying. It doesn’t lead to long-term damage to your skin.
To prevent scarring or infection, you shouldn’t pick at, scratch or try to pop your keratosis pilaris.
Even with treatment, it may take time for keratosis pilaris bumps to go away. If you follow your treatment plan, you should start seeing improvement within four to six weeks.
Even without treatment, most cases of keratosis pilaris start to clear around your mid-20s, and usually completely disappears by age 30.
You can’t prevent keratosis pilaris. But avoiding dry skin by maintaining a gentle skin care routine can help minimize the appearance of keratosis pilaris.
If you don’t start seeing improvement four to six weeks after starting a treatment plan, or if your keratosis pilaris affects your self-esteem, reach out to your healthcare provider.
One of the symptoms of gluten intolerance is a skin rash that looks similar to keratosis pilaris. No research indicates that gluten intolerance causes keratosis pilaris, though.
Keratosis pilaris is often a temporary skin condition that goes away over time. It usually doesn’t cause any symptoms. But if you experience any discomfort like itchy or dry skin, or if it affects your mental health (self-esteem), reach out to your healthcare provider. There are ways to treat keratosis pilaris. Talk to your healthcare provider about the best ways to care for your skin.
Every day, people see your skin, hair and nails. At Cleveland Clinic, our expert and caring dermatology team will make sure they’re healthy and strong.

Last reviewed on 04/15/2022.
Learn more about the Health Library and our editorial process.