Deep vein thrombosis is a blood clot in a vein located deep within your body, usually in your leg. Get treatment right away so you can prevent serious complications. Treatments include medicines, compression stockings and surgery. Be patient. You may need to take medicine for a few months and wear compression stockings for two years.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
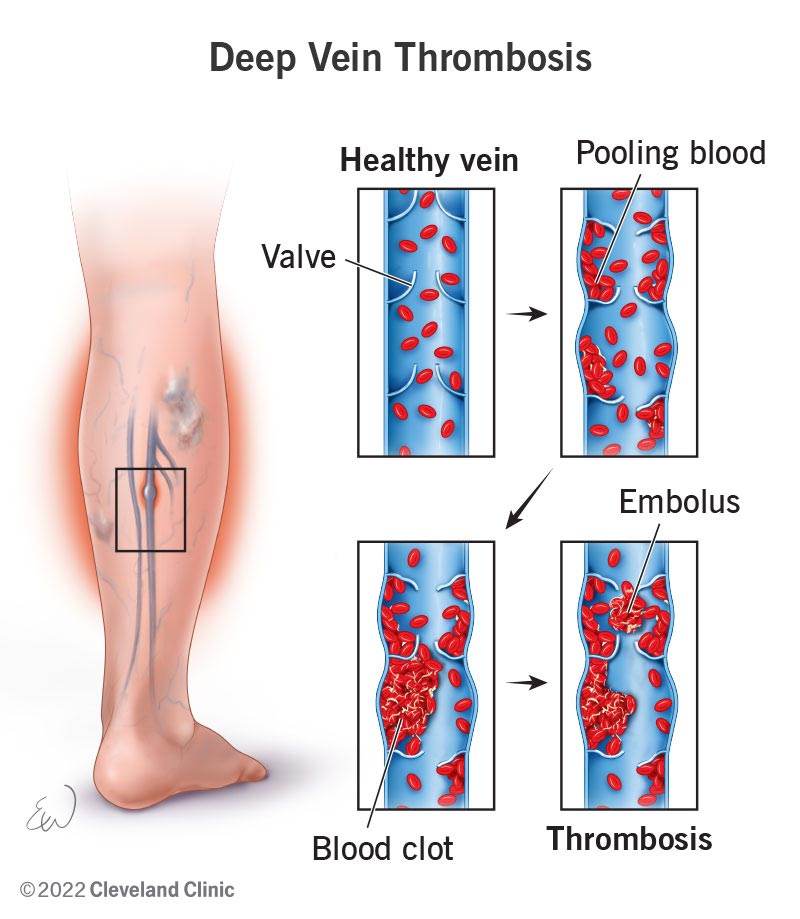
Deep vein thrombosis (DVT, also called venous thrombosis) occurs when a thrombus (blood clot) develops in veins deep in your body because your veins are injured or the blood flowing through them is too sluggish. The blood clots may partially or completely block blood flow through your vein. Most DVTs happen in your lower leg, thigh or pelvis, but they also can occur in other parts of your body including your arm, brain, intestines, liver or kidney.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Even though DVT itself is not life-threatening, the blood clots have the potential to break free and travel through your bloodstream. A pulmonary embolism (PE) happens when the traveling blood clots (emboli) become lodged in the blood vessels of your lung. Since this can be a life-threatening condition, you need a quick diagnosis and treatment.
As many as half of those who get a DVT in their legs develop symptoms of intermittent leg pain and swelling that may last months to years. These symptoms are called post-thrombotic syndrome and can happen because of damage to the valves and inner lining of your veins leading to blood “pooling” more than it should. This increases the pressure inside your veins and causes pain and swelling.
Characteristics of this condition include:
A superficial venous thrombosis (also called phlebitis or superficial thrombophlebitis) is when blood clots develop in a vein close to the surface of your skin. These types of blood clots rarely travel to your lungs unless they move from the superficial system into the deep venous system first. While a physician can diagnose superficial vein clots with a physical exam, they can only diagnose DVT with an ultrasound.
Advertisement
Each year, approximately 1 to 3 in every 1,000 adults develop a DVT or pulmonary embolism in the United States, and up to 300,000 people die each year as a result of DVT/PE. It’s the third most common vascular disease, behind heart attacks and strokes. Acute DVT/PE can occur at any age, but are less common in children and adolescents and more common in those over the age of 60. More than half of all DVTs happen as a result of being in the hospital from a medical illness or following surgery. The reason why DVTs are more common after a hospital stay is because you’re lying in bed most of the time instead of moving around like you normally would.
A DVT usually forms in the veins of your legs or arms. Up to 30%of people with a DVT don’t have symptoms, but sometimes the symptoms are very mild and may not raise concern. The symptoms associated with an acute DVT include:
Some people don’t know they have a DVT until the clot moves from their leg or arm and travels to their lung. Symptoms of acute PE include chest pain, shortness of breath, cough with blood, lightheadedness and fainting.
It’s important to call your doctor right away or go to the emergency room if you have symptoms of a DVT. Don’t wait to see if your symptoms go away. Get treatment right away to prevent serious complications.
These conditions can increase your risk of a deep vein thrombosis:
Advertisement
Your healthcare provider will do a physical exam and review your medical history. You’ll also need to have imaging tests.
Duplex venous ultrasound. This is the most common test for diagnosing a DVT because it is non-invasive and widely available. This test uses ultrasound waves to show blood flow and blood clots in your veins. A vascular ultrasound technologist applies pressure while scanning your arm or leg. If the pressure doesn’t make your vein compress, it could mean there’s a blood clot. If the results of the duplex ultrasound aren’t clear, your provider can use another imaging test
Venography. In this invasive test, your provider numbs the skin of your neck or groin and uses a catheter to inject a special dye (contrast material) into your veins to see if any blood clots are partially or completely blocking blood flow inside your veins. Venography is rarely used nowadays, but sometimes it is necessary
Magnetic Resonance Imaging (MRI) or Magnetic Resonance Venography (MRV). MRI shows pictures of organs and structures inside your body. MRV shows pictures of the veins in specific locations in your body. In many cases, MRI and MRV can offer more information than a duplex ultrasound or CT scan.
Advertisement
Computed tomography (CT) scan is a type of X-ray that shows structures inside your body. Your provider may use a CT scan to find a DVT in your abdomen, pelvis or brain, as well as blood clots in your lung (pulmonary embolism).
If your doctor thinks you may have a genetic or acquired clotting disorder, you may need to have special blood tests. This may be important if:
A DVT may make it harder for you to get around at first because of leg pain and swelling. But you’ll be able to slowly return to your normal activities. If your legs feel swollen or heavy, lie in bed with your heels propped up about 5 to 6 inches. This helps improve circulation and decreases swelling.
In addition:
Advertisement
Some people with a DVT may need to be treated in the hospital. Others may be able to have outpatient treatment.
Treatments include medications called anticoagulants (blood thinners), compression stockings and elevating your affected leg(s) at different times throughout the day. In a minority of cases, when the DVT is extensive, invasive treatments (catheter-based procedures) may be required.
The main goals of treatment are to:
Anticoagulants (blood thinners)
This type of medication makes it harder for your blood to clot. Anticoagulants also stop clots from getting bigger and prevent blood clots from moving. Anticoagulants don’t destroy or “melt” blood clots. Your body may naturally dissolve a clot, but sometimes clots don’t completely disappear. When they don’t, they usually shrink and become little “scars” inside your veins. Sometimes these “old” clots may result in leg swelling, but oftentimes they don’t cause symptoms.
There are different types of anticoagulants: warfarin, heparin and oral Xa inhibitors. Your doctor will talk to you about the best type of medication for you.
If you need to take an anticoagulant, you may have to take it for only a few months (usually three to six months) or you might take it indefinitely. Your treatment time may be different depending on the specific situations of each individual, including if:
Bleeding is the most common side effect of anticoagulants. You should call your doctor right away if you notice that you bruise or bleed easily while taking this medication.
You‘ll probably need to wear graded elastic compression stockings to either improve or completely get rid of leg swelling. Damage to the small valves inside your veins often causes this swelling. You may also have swelling because the DVT is blocking blood flow in your vein. You wear most compression stockings just below your knee. These stockings are tight at the ankle and become looser as they go away from your ankle. This causes gentle pressure (compression) on your leg. Some people need to wear these for two years or more. Several clinical studies have shown that compression stockings improve the symptoms of leg pain and swelling by at least 50% as long as they’re worn daily from morning to evening (they don’t have to be worn overnight).
After surgery, your providers may put compression devices on your calves to put pressure on them. These machines squeeze and release the fabric-covered devices around your calves while you’re lying in bed. These devices help prevent a DVT if you’re in the hospital, but they aren’t prescribed outside of the hospital. In addition, unlike compression stockings that you can wear safely when a leg DVT is present, you shouldn’t use these devices for DVT prevention if you have a DVT.
When you can’t take medications to thin your blood or you have blood clots while taking blood thinners without missing doses, a surgeon may have to do a procedure to put in an inferior vena cava (IVC) filter. The procedure is done under local anesthesia. Your surgeon inserts the IVC filter through a catheter into a large vein in your groin or neck, and then into your vena cava (the largest vein in your body). If blood clots in the veins of your legs break off and travel, the IVC filter is designed to prevent large blood clots (emboli) from reaching your lungs and causing a pulmonary embolism. While an IVC filter helps prevent a pulmonary embolism, it doesn’t keep more blood clots from forming in your veins.
A DVT can take several months to a year to come apart, so you’ll need to keep taking blood thinner medicines as instructed and keep wearing compression stockings until your provider tells you to stop. You may need blood tests to make sure you’re getting the right dose of blood thinners. Your provider may want to do more ultrasounds later to find out if your blood clot is still in the same place, improving or getting larger.
After you have a DVT, you’ll need to reduce your risk of future DVT/PE clots by:
If you’ve never had a DVT, but have an increased risk of developing one, be sure to:
Tell your healthcare provider if your symptoms aren’t getting better. You should also tell them if you’re bruising too easily or have heavy periods.
You should get emergency care if the blood thinners you’re taking make you bleed too much, or cause problems like bright red blood in vomit or poop.
If you have a deep vein thrombosis, you’re not alone. Every year, at least 1 million Americans get one. Several treatments can help, and your healthcare provider can customize your care to your situation. If they prescribe blood thinners, be sure to keep up with all of your follow-up appointments so you know you’re getting the correct dose.
Vascular disease may affect your life in big and small ways. Cleveland Clinic’s specialists treat the many types of vascular disease so you can focus on living.

Last reviewed on 03/28/2022.
Learn more about the Health Library and our editorial process.