Heat-related illnesses include heat stroke, heat exhaustion, heat cramps and heat rash. Heat stroke and heat exhaustion involve an abnormally high body temperature (hyperthermia) and need immediate treatment. You can lower your risk of heat illness by staying hydrated and limiting physical activity in hot weather.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Heat-related illness (also commonly called hyperthermia) refers to a group of conditions that happen when your body has trouble cooling itself down.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Normally, your body has safeguards in place to cool you down when you get too hot. For example, your sweat glands produce sweat that evaporates from your skin, lowering your body temperature before it can get to dangerous levels. But sometimes, the weather is so hot and humid, or your body produces so much internal heat (for example, from a vigorous workout) that your natural cooldown system gets overwhelmed.
Picture trying to cool an entire house with a single fan on a hot day — it just won’t work. There’s too much heat building up and not enough cooling action from the fan. It’s similar with heat-related illnesses. Your body gets overwhelmed by heat and needs some extra help to cool itself down.
Heat-related illnesses occur on a spectrum from mild to severe. Mild heat-related illnesses — like heat rash and heat cramps — usually go away with rest or at-home treatments. But moderate or severe heat-related illnesses — like heat exhaustion and heat stroke — require prompt medical attention to avoid serious complications.
Hyperthermia is a medical term that means your internal (core) body temperature is higher than normal. This generally means your temperature is higher than 98.6 degrees Fahrenheit (37 degrees Celsius). Some people have a baseline temperature that’s a bit higher or lower than that. Anything above your baseline is hyperthermia.
Advertisement
Not all heat-related illnesses cause a spike in your body temperature, or hyperthermia. But the most serious forms — heat exhaustion and heat stroke — typically do. That’s why people often use the terms hyperthermia and heat-related illness interchangeably.
The four main types of heat illness, in order from mildest to most severe, include:
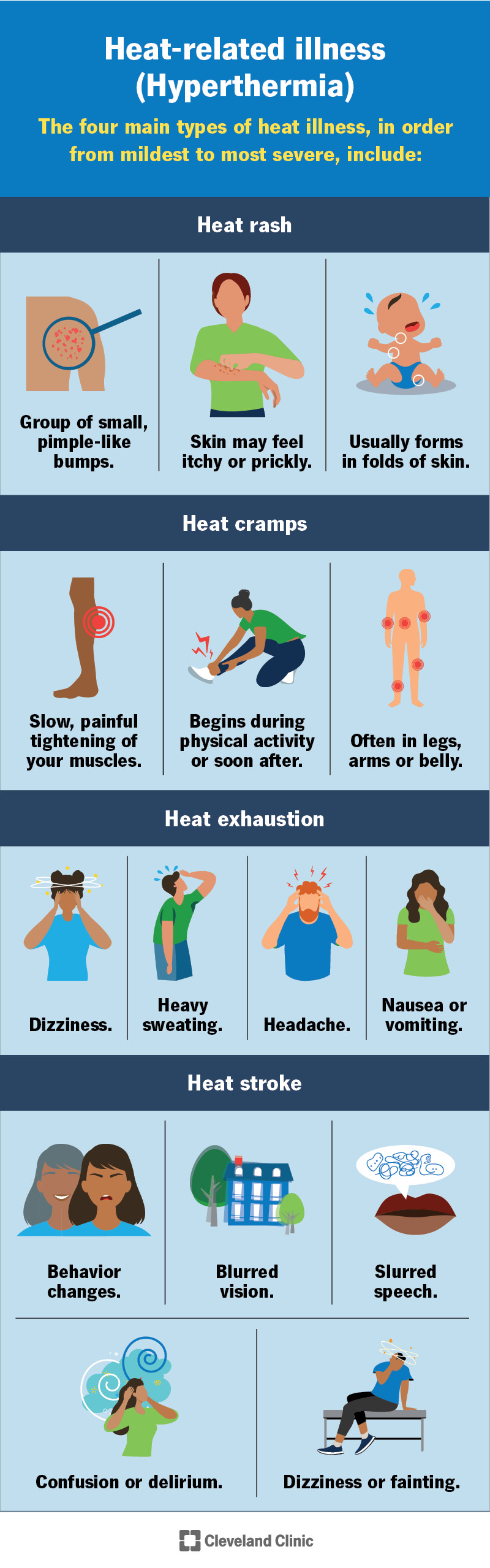
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22111-hyperthermia.jpg)
Hyperthermia symptoms vary according to the specific condition you have. The infographic below lists the signs and symptoms of the four main types of heat illness.
Heat stroke, unlike other heat illnesses, affects your brain function. Besides physical symptoms, it causes changes to your thinking and behavior. Often, bystanders are the ones who notice heat stroke symptoms in a person and call for medical help. If you have heat stroke, you may be confused, delirious or unconscious and have difficulty seeking help for yourself.
Heat-related illnesses happen when your body’s usual mechanisms for managing heat get overwhelmed. This can occur due to hot and humid weather, metabolic heat (heat your body makes) or both. As a result, your body can’t get rid of heat efficiently enough to keep your temperature at a normal level. Sometimes, your temperature stays normal but you develop other, uncomfortable symptoms — like a rash or muscle cramping.
You may have an increased risk of heat-related illness if you:
Advertisement
Not all heat illnesses receive an official diagnosis. You may recognize the signs and symptoms of milder conditions, like heat rash or heat cramps, and manage things on your own. But you may choose to see a provider for those conditions if symptoms are severe or won’t go away. If you have signs of heat exhaustion or heat stroke, seek medical care immediately.
In general, a healthcare provider will diagnose your condition by doing a physical exam and talking to you about your symptoms — including what makes them better or worse. Heat exhaustion and heat stroke are often diagnosed and treated in the emergency room. There, providers check your vital signs and review your symptoms. They’ll begin treatment right away to prevent complications.
Treatment depends on the type of heat-related illness. You can usually manage heat rash and heat cramps on your own. You should seek medical attention for heat exhaustion and heat stroke while taking measures to cool your body.
The table below lists common treatments for each type of heat illness.
| Heat rash | Keep your skin cool and dry. Wear loose clothing. Limit time in the heat. Use anti-itch creams. Avoid emollients (moisturizers). Contact a provider if you have signs of an infection, like warm-feeling skin or pus drainage. |
|---|---|
| Heat cramps | Get out of the heat. Rest. Replenish fluids and electrolytes. Don’t do anything physically taxing in the heat for at least two days. |
| Heat exhaustion | This could progress to heat stroke. Seek immediate medical attention. Meanwhile, get out of the heat. Loosen or remove excess clothes. Lie down with your legs elevated. Slowly sip water. Cool down by pouring water on your skin and fanning yourself; applying ice packs to your skin; soaking towels in ice water and applying them to your skin. |
| Heat stroke | This is a medical emergency. Seek immediate medical attention. Bystanders may need to help you by moving you out of the heat and using any available means to cool you down. Don’t drink any fluids (you may inhale them, which is dangerous). Don’t take any fever-reducing medications (they won’t help and may worsen complications). You’ll need care at a hospital, which may include rapid body cooling and supportive treatment for your organs. |
| Heat rash | |
| Heat cramps | |
| Keep your skin cool and dry. Wear loose clothing. Limit time in the heat. Use anti-itch creams. Avoid emollients (moisturizers). Contact a provider if you have signs of an infection, like warm-feeling skin or pus drainage. | |
| Get out of the heat. Rest. Replenish fluids and electrolytes. Don’t do anything physically taxing in the heat for at least two days. | |
| Heat exhaustion | |
| Keep your skin cool and dry. Wear loose clothing. Limit time in the heat. Use anti-itch creams. Avoid emollients (moisturizers). Contact a provider if you have signs of an infection, like warm-feeling skin or pus drainage. | |
| This could progress to heat stroke. Seek immediate medical attention. Meanwhile, get out of the heat. Loosen or remove excess clothes. Lie down with your legs elevated. Slowly sip water. Cool down by pouring water on your skin and fanning yourself; applying ice packs to your skin; soaking towels in ice water and applying them to your skin. | |
| Heat stroke | |
| Keep your skin cool and dry. Wear loose clothing. Limit time in the heat. Use anti-itch creams. Avoid emollients (moisturizers). Contact a provider if you have signs of an infection, like warm-feeling skin or pus drainage. | |
| This is a medical emergency. Seek immediate medical attention. Bystanders may need to help you by moving you out of the heat and using any available means to cool you down. Don’t drink any fluids (you may inhale them, which is dangerous). Don’t take any fever-reducing medications (they won’t help and may worsen complications). You’ll need care at a hospital, which may include rapid body cooling and supportive treatment for your organs. |
Your outlook depends on many factors, including:
Advertisement
Some heat illnesses — like heat rash — are typically mild and won’t affect your outlook much. But heat exhaustion can quickly turn into heat stroke, which can be life-threatening. Your healthcare provider can tell you more about what to expect in your situation.
You can lower the risk of your body overheating by:
Call 911 or your local emergency services number if you have signs of heat exhaustion or heat stroke. The sooner you get treatment, the better your chances of recovering.
You may not need medical care for heat cramps or heat rash. But if symptoms bother you a lot or get worse, contact a healthcare provider. They can rule out other causes and make sure you get proper treatment.
Advertisement
Talking about heat-related illness with your provider is the first step toward preventing it. Here are some questions you may want to ask your provider to stay one step ahead of the heat:
If you’re recovering from a heat illness, it may help to ask your provider:
You can have a raised body temperature without having a heat-related illness. Hyperthermia can also happen due to:
Hyperthermia is the medical term for an elevated body temperature. This can have many causes, including infections and heat exposure.
When an infection causes a raised temperature, you have a fever. Your hypothalamus triggers activity within your body that makes your temperature go up. This is a bit like turning up the setting on a thermostat. It’s intentional and your body is in control. Once the infection clears, your hypothalamus turns the setting back down so you return to a normal temperature.
When you’re overheated from hot weather or physical exertion, your body temperature rises, but we don’t say you have a fever. This is because your hypothalamus isn’t raising your internal “thermostat.” Instead, heat overwhelms your body, and your body’s normal cooling mechanisms (primarily sweating) struggle to keep up. It’s like on a hot day when you have the A/C on full blast but the room temperature still isn’t lowering to where you want it to be.
So, a fever is always hyperthermia, but hyperthermia doesn’t always mean a fever.
Heat-sensitive diseases are conditions that heat exposure triggers or worsens. Examples include:
If you have one of these conditions or any risk factors, talk to your healthcare provider about ways to protect yourself in hot weather.
Hot weather can be lovely and relaxing. But with the heat come certain risks that might not always be obvious. Heat-related illness can happen to anyone. Even if you’ve exerted yourself in the heat before and felt fine, that doesn’t mean you’ll avoid heat illness in the future. It’s always important to stay hydrated, limit physical activity in extreme heat and take steps to protect others around you.
If you can’t avoid heat exposure due to work or other obligations, talk to your healthcare provider. They can help you come up with a plan for lowering your risk of heat illness. They’ll also explain which signs or symptoms to look out for and when to seek medical care.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s primary care providers offer lifelong medical care. From sinus infections and high blood pressure to preventive screening, we’re here for you.
