Paronychia (nail infection) usually results from bacteria. Bacteria get into the skin through cuts in the cuticle and the nail fold (the skin around the nail). Most nail infections get better with antibiotics. Paronychia doesn’t usually cause serious health problems. In some cases, the infection lasts a long time or comes back after treatment.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
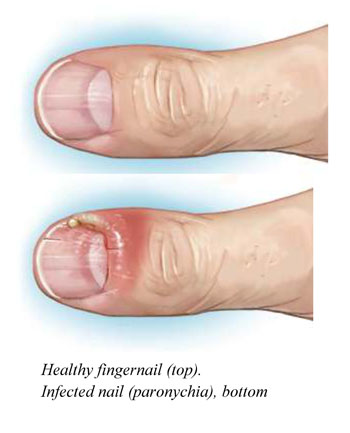
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/15327-nail-infection.ashx)
Paronychia is nail inflammation that may result from trauma, irritation or infection. It can affect fingernails or toenails.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Paronychia can develop when bacteria enter broken skin near the cuticle and nail fold, causing an infection. The cuticle is the skin at the base of the nail. The nail fold is where the skin and nail come together.
Healthcare providers treat paronychia with antibiotics to kill the infection. Providers may also drain pus (thick, infectious fluid that builds up around a wound). They may also culture the fluid to see what specific bacteria might be causing the infection.
Sometimes, the infection comes back or symptoms last for weeks (chronic paronychia). Chronic paronychia is more commonly caused by irritation from occupational or environmental exposures. Less often, it may be caused by a chronic bacterial or fungal infection.
Paronychia is a common nail condition. Anyone can get a bacterial nail infection, but it’s more common among people who:
Advertisement
Symptoms of paronychia usually develop over several hours or days. Sometimes they take longer to develop. Symptoms appear where the nail meets the skin (the nail fold and cuticle). The sides of the nail can also be affected.
Paronychia symptoms include:
Untreated, the nail can start to grow abnormally and may have ridges or waves. It may look yellow or green, and it can be dry and brittle. The nail can detach from the nail bed and fall off.
Most commonly, infectious paronychia results from a staph infection. Staphylococcus aureus bacteria cause staph infections. Other bacteria (such as Streptococcus pyogenes) can also cause the infection. Bacteria get into the skin through:
There are two types of paronychia. Both types have similar signs and symptoms:
Your provider will ask about your symptoms and do a physical exam. Healthcare providers usually don’t need to order tests to diagnose a nail infection. Occasionally, providers may take a sample of the tissue and send it to a lab to test for specific infectious causes such as bacteria or fungi. Rarely, if the infection is severe, imaging (such as an X-ray) may be ordered to check for involvement of the underlying bone.
You may be able to treat mild cases of paronychia at home. Soak the infected area in warm water for about 15 minutes a few times a day. Be sure to dry the area thoroughly. Soaking the cuticle and nailbed helps pus drain from under the skin.
Advertisement
If symptoms don’t get better after a day or two of home remedies, see your provider. You may need other treatments, such as antibiotics, to clear up the infection and help you heal. You may also need minor procedures such as drainage if an abscess has formed.
Most bacterial nail infections go away with antibiotics. These medications kill bacteria that cause infections. Be sure to follow your provider’s instructions and finish the entire course of antibiotics so the infection doesn’t return.
If pus has built up around the nail bed and isn’t draining on its own, your provider may drain the pus. After cleaning the area, your provider makes a small cut so the pus can drain. Your provider places a bandage over the cut. You should keep the area clean and replace the bandage when necessary.
Paronychia usually clears up with treatment. Some people get more than one infection, or the infection comes back after treatment (chronic paronychia). Untreated, the infection can cause damage to the nail.
Rarely, untreated paronychia can go deeper into the finger or toe and lead to a serious infection. The infection may progress to involve the underlying bone. In severe cases, providers need to remove a finger or toe to make sure the infection doesn’t spread to the rest of the body. Severe, chronic paronychia most often affects people who have diabetes or conditions that cause problems with blood circulation.
Advertisement
To prevent a nail infection, you should:
If you have diabetes or another condition that affects your circulation, or are immunosuppressed, call your provider as soon as you notice signs of infection. You should seek immediate care if you have a condition that affects your body’s ability to fight infection.
See your provider if symptoms are severe or don’t go away after a few days. If symptoms return after treatment, call your provider for an evaluation.
Nail infections can be painful, but they don’t usually cause serious health problems. If your job requires you to work with chemicals or detergents, or if your hands are frequently wet, talk to your provider. You can protect your hands and avoid an infection by wearing waterproof gloves that do not irritate the skin. Seek treatment right away if you have diabetes or difficulty fighting infections. Also, see your provider if paronychia comes back after treatment, or if your symptoms worsen or don’t go away.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s primary care providers offer lifelong medical care. From sinus infections and high blood pressure to preventive screening, we’re here for you.
