Plantar fasciitis is caused when you overuse or put too much stress on your feet. You can usually treat plantar fasciitis at home with over-the-counter medications, icing, rest and stretching.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
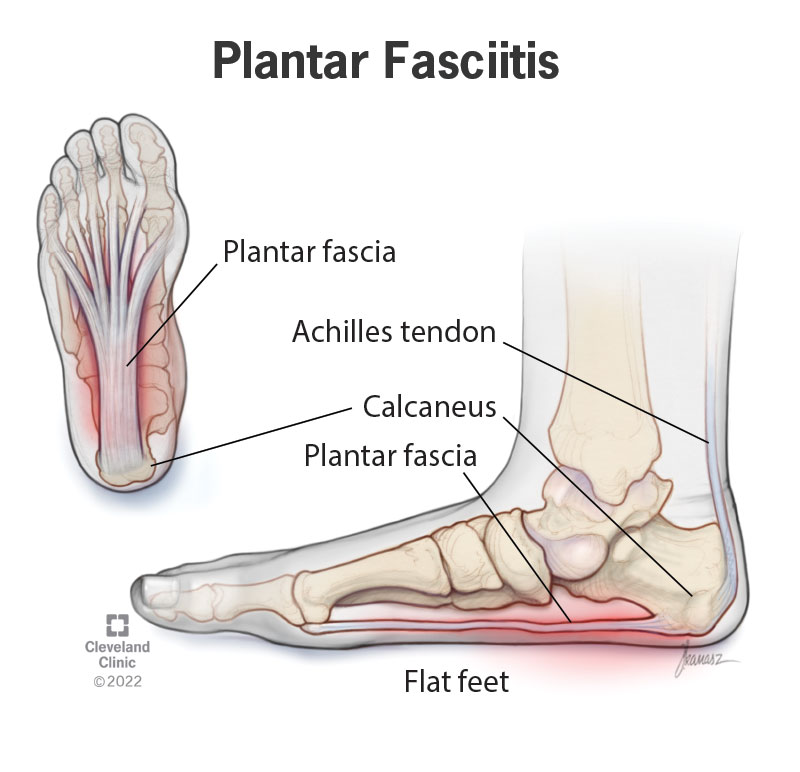
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/14709-plantar-fasciitis.jpg)
Plantar fasciitis is inflammation in the plantar fascia in your foot. It’s the most common cause of heel pain.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The plantar fascia is a strong, fibrous attachment (similar to a ligament) that runs from your heel to the ball of your foot and your toes. It's stretchy like a thick rubber band. The plantar fascia connects the bones in your foot together and forms the arch on the bottom of your foot.
Plantar fasciitis happens when your plantar fascia is overused or stretched too far. Anything that damages your plantar fascia can make it swell. This inflammation makes it painful to walk or use your foot. Most people experience plantar fasciitis in one foot at a time, but it’s possible for it to affect both your feet at once.
Visit a healthcare provider if you’re experiencing heel or foot pain for more than a week.
Plantar fasciitis is extremely common. More than 2 million people in the U.S. are treated for it each year. Around 1 in 10 people will develop plantar fasciitis at some point throughout their life.
The most common symptoms of plantar fasciitis include:
Plantar fasciitis usually causes an achy pain in your heel or along the bottom of your foot. The pain can change depending on what you’re doing or the time of day. Some types of pain you might feel include:
Advertisement
Anything that irritates or damages your plantar fascia can cause plantar fasciitis, including:
Some health conditions can cause plantar fasciitis, including:
A healthcare provider will diagnose plantar fasciitis with a physical exam. They’ll ask you about your symptoms and look at your foot. They might lightly press on your plantar fascia to feel for inflammation and check your level of pain.
Tell your provider about the pain you’re experiencing in your daily routine. Tell them where on your foot it hurts and when it’s the most painful throughout the day.
A healthcare provider usually won’t need any tests to diagnose plantar fasciitis. They might use imaging tests to take pictures of your foot if they think another issue or condition is causing the pain. Some imaging tests you might need include:
Video content: This video is available to watch online.
View video online (https://cdnapisec.kaltura.com/p/2207941/sp/220794100/playManifest/entryId/1_4ucn3bof/flavorId/1_5f3sgelj/format/url/protocol/https/a.mp4)
Try these stretches for plantar fasciitis.
You can usually manage plantar fasciitis with at-home treatments and over-the-counter (OTC) medicine.
Your healthcare provider will suggest options for relieving your symptoms and supporting your feet to reduce the chances you’ll experience plantar fasciitis again in the future.
The most common treatments for plantar fasciitis include:
Advertisement
The treatments listed above are usually all you’ll need to relieve your symptoms and treat plantar fasciitis. It’s very rare to need surgery. The two most common types of surgery include:
Your healthcare provider or surgeon will tell you which type of surgery you’ll need to treat plantar fasciitis.
You should notice your plantar fasciitis symptoms improving as soon as you start treating them. But it can take anywhere from a few weeks to a few months for your plantar fascia to heal.
If you feel better but then your symptoms return, try the same at-home treatments you used before. Talk to your provider if your symptoms feel different or worse than before.
You might need to miss work or school for at least a few days while you’re recovering if an activity you do often caused the plantar fasciitis. Tell your healthcare provider about your daily routine — especially if you need to be on your feet all day for work.
You should avoid playing sports and other activities that put pressure on your feet for at least a week. Talk to your provider before resuming intense physical activity.
Advertisement
The best way to prevent plantar fasciitis is to avoid overusing your feet. In general:
If you have a health condition that makes you more likely to develop plantar fasciitis, you might not be able to prevent it.
Visit a healthcare provider if:
Plantar fasciitis and heel spurs both cause pain in your heel, but they’re different conditions.
A heel spur is a bony growth that pokes out from the bottom of your heel where your heel bone connects to your plantar fascia. It can happen as a reaction to stress and inflammation caused by plantar fasciitis. Most people don’t feel pain from a heel spur, but when they do, the pain is like plantar fasciitis pain.
Advertisement
Visit a healthcare provider if you’re experiencing pain in your foot or heel.
Plantar fasciitis is the most common cause of heel pain. Talk to a healthcare provider if you’re experiencing pain in your heel or foot that doesn’t get better on its own in a week. They’ll help you find at-home treatments to reduce the pain and inflammation in your foot.
It’s always annoying to find out you need to skip a week (or more) of your favorite sport or activity. But don’t rush back onto the field or court. You might re-injure your plantar fascia if you put too much stress on your foot before it’s healed.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Heel pain or pain in your foot’s arch can really affect your daily life. Cleveland Clinic specialists can get you back on your feet again, as pain-free as possible.
