Actinic keratosis is a precancerous skin condition that shows up as rough or discolored areas on sun-exposed skin. It’s common and treatable. Without treatment, it can turn into squamous cell carcinoma (SCC) skin cancer. An early diagnosis and sun protection can make a big difference.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
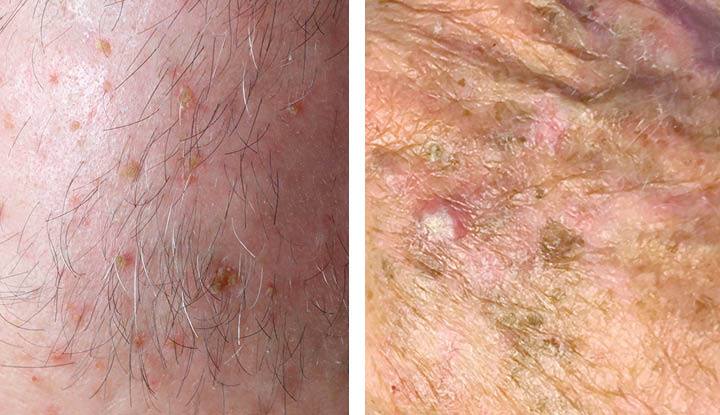
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/14148-actinic-keratosis)
Actinic keratosis (pronounced ak-TIN-ik ker-uh-TOH-sis), also known as solar keratosis, is a skin condition that happens with too much sun exposure. It causes rough, scaly spots of skin. They commonly appear on your:
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
But it can form on other sun-exposed areas, too.
It’s the most common type of skin precancer. It can lead to a type of skin cancer called squamous cell carcinoma. Treatment is available to prevent actinic keratosis from turning into skin cancer.
Each year, more than 40 million Americans develop actinic keratosis.
There are several types. Some of the most common include:
If you have this skin condition, you might notice an area of skin that’s:
Many types feel like sandpaper. Some could look like an acne breakout at first. You might mistake it for a scab or sore that won’t go away.
Too much exposure to ultraviolet (UV) light causes actinic keratosis. It’s most often from the sun. It can also develop from frequent use of indoor tanning equipment, like tanning beds.
Advertisement
UV rays damage the DNA in your skin cells. It targets the outer layer of cells called keratinocytes. Over time, repeated sun exposure causes these cells to grow abnormally. This leads to a rough or scaly spot on your skin.
You may be more likely to get this skin condition if you:
Actinic keratosis can sometimes turn into skin cancer (called squamous cell carcinoma). Most cases receive treatment before they reach the cancer stage, but there’s still a risk. A healthcare provider can help you if you notice any skin changes.
A primary care physician or a dermatologist (a skin specialist) can usually diagnose this condition by examining your skin. They may use a special tool that magnifies your skin to get a better look. This exam is quick and painless.
Sometimes, your provider may need to take a small sample of your skin to send to a lab for testing. This is called a skin biopsy.
Treatment options depend on how many actinic keratoses (AKs) you have and where they are on your body. Your provider may recommend removing them during an office visit. Options include:
Your provider may also suggest using removal treatments and medicated creams for the best results.
There are different medicated creams or gels that you can apply at home. You may need to use these for several weeks to a few months. Your provider will prescribe these for you.
Some examples include:
Advertisement
Some treatments can cause skin discoloration, peeling or irritation as they work. Your provider will give you instructions on how to use these and what to expect.
Let your healthcare provider know if you have any changes to your skin, like:
Most actinic keratoses heal within a few weeks after treatment. The exact timing depends on the type of treatment you receive. Your provider will explain what to expect.
Actinic keratosis can sometimes come back after treatment. To prevent this, it’s important to protect your skin from the sun, both during treatment and afterward.
Even if AKs go away, you should still see your provider once or twice a year for regular skin checkups. Because there’s a risk of skin cancer or returning spots, keeping up with these visits helps catch any problems early. If you notice a new or unusual spot, get it checked as soon as possible.
The best way to prevent actinic keratosis is to limit your exposure to sunlight. You can protect your skin by:
Advertisement
That rough patch on your hand or scaly spot on your face isn’t something you should ignore. An itchy or stinging sensation could be your skin’s way of saying it got too much sun exposure. A healthcare provider can look over your skin to let you know exactly what’s going on under the surface.
Fortunately, treatment options are available to remove actinic keratosis spots. Treatment also lowers your risk of developing skin cancer.
Your skin is one of your body’s most important organs. Taking care of it now helps keep it healthy for years to come.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s primary care providers offer lifelong medical care. From sinus infections and high blood pressure to preventive screening, we’re here for you.
