Gingivitis is the earliest stage of gum disease. It happens when plaque and bacteria build up on your teeth and cause infection. Common symptoms include red, swollen, bleeding gums. Treatments include regular dental cleanings and improved oral hygiene at home between visits.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
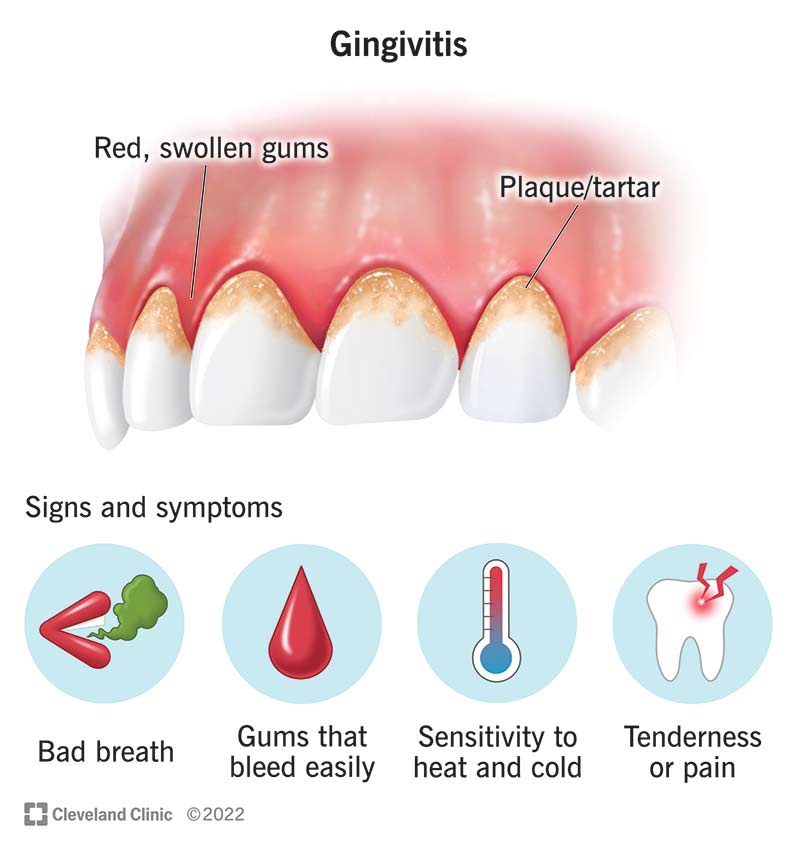
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/10950-gingivitis)
Gingivitis is the earliest stage of gum disease (periodontal disease). It develops when plaque, tartar and bacteria build up on your teeth, causing red, swollen, bleeding gums.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
You can successfully manage gingivitis, especially with the help of a dentist. But left untreated, gingivitis can lead to periodontitis (a more severe type of gum disease involving bone loss in your jaw).
Gum disease is more likely to occur in:
Gingivitis is very common. Almost half of all adults older than 30 have some kind of gum disease.
Gingivitis symptoms aren’t always obvious in the early stages, so you may have it and not know it. As the condition worsens over time, you may develop:
Video content: This video is available to watch online.
View video online (https://cdnapisec.kaltura.com/p/2207941/sp/220794100/playManifest/entryId/1_vsrdjs12/flavorId/1_5f3sgelj/format/url/protocol/https/a.mp4)
Learn what causes gum disease, the symptoms and how to treat it.
Gingivitis is your body’s inflammatory response to plaque and tartar on your teeth. When plaque and tartar remain on your teeth for too long, your gums become irritated, red and swollen.
Advertisement
You may face a higher risk of developing gingivitis if you:
Also, some prescriptions and over-the-counter medications can reduce the flow of saliva (spit), resulting in dry mouth (xerostomia). Saliva helps keep your mouth clean, so this change may contribute to gingivitis. Examples of such medications include:
The bacteria that cause gingivitis are transmissible from one person to another. So, even though experts agree that gingivitis itself isn’t contagious, people who have the condition can spread bacteria through saliva-to-saliva contact.
The bottom line? You’re not likely to get gingivitis from kissing or sharing utensils. But if you have saliva-to-saliva contact with someone who has gingivitis, you’re more likely to develop the condition yourself. This is especially true if you have poor oral hygiene or have health conditions that make you more susceptible to disease, such as HIV/AIDS or leukemia.
If you have gingivitis symptoms, you should see a dentist for a checkup. Your dentist will inspect your mouth for:
If your dentist suspects gum disease, dental X-rays can show if it has affected your jawbone underneath. Your dentist may also refer you to a periodontist (a gum disease specialist).
Treatment of gingivitis aims to control the infection and restore healthy teeth and gums. Your dentist or periodontist will thoroughly clean your teeth to remove harmful bacteria, plaque and tartar. Additional gingivitis treatments include:
Advertisement
The earlier you catch gum disease, the more you can manage it. Gingivitis is reversible with proper care and maintenance, but it can come back. You must take good care of your teeth and gums between office visits.
If you don’t treat gingivitis, it can turn into a more serious gum disease. Known as periodontitis, this gum disease damages the structures that keep your teeth anchored.
Unlike the other stages of gum disease, gingivitis is curable as long as you treat it early enough. If you notice symptoms of gingivitis, you should schedule an appointment with a dentist and immediately begin practicing better oral hygiene at home.
Untreated gingivitis can worsen and turn into periodontitis. At this stage of gum disease, you start to lose bone around your teeth — a permanent side effect that results in a domino effect of oral health issues.
The fastest way to get rid of gingivitis is to see a dentist for a cleaning and improve your oral hygiene habits at home between visits.
You can reduce your risk for gingivitis with good oral hygiene:
Advertisement
If people in your family have gum disease, you may face a greater risk of developing it. You may need more checkups and cleanings to prevent gum disease. Ask your dentist about a cleaning schedule that’s right for you.
If you have one or more of the symptoms of gingivitis, call your dentist. They may examine you at your next checkup or make a special appointment. It depends on how long you’ve had symptoms and how severe they are.
Consider asking your dentist the following questions:
The good news is that early treatment can reverse gingivitis. But left untreated, gingivitis can progress into advanced gum disease. Detecting and treating the issue early can save you a lot of time, worry and money in the future.
Everyone’s mouth is full of bacteria. Good oral hygiene can stop bacteria from causing gingivitis, the first stage of gum disease. If you find and treat gingivitis early, you can avoid permanent damage to your teeth and gums. See a dentist regularly for cleanings and checkups, not just when you have a toothache or another dental issue.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
At Cleveland Clinic, we have expert knowledge when it comes to slowing and reversing gum disease. We’ll craft a treatment plan that focuses on you and your needs.
