Blepharitis, the medical term for irritated, swollen eyelids, is a common eye condition. It’s a chronic condition, but it’s not contagious. If you have oily skin or certain skin conditions, you may be more likely to develop blepharitis.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
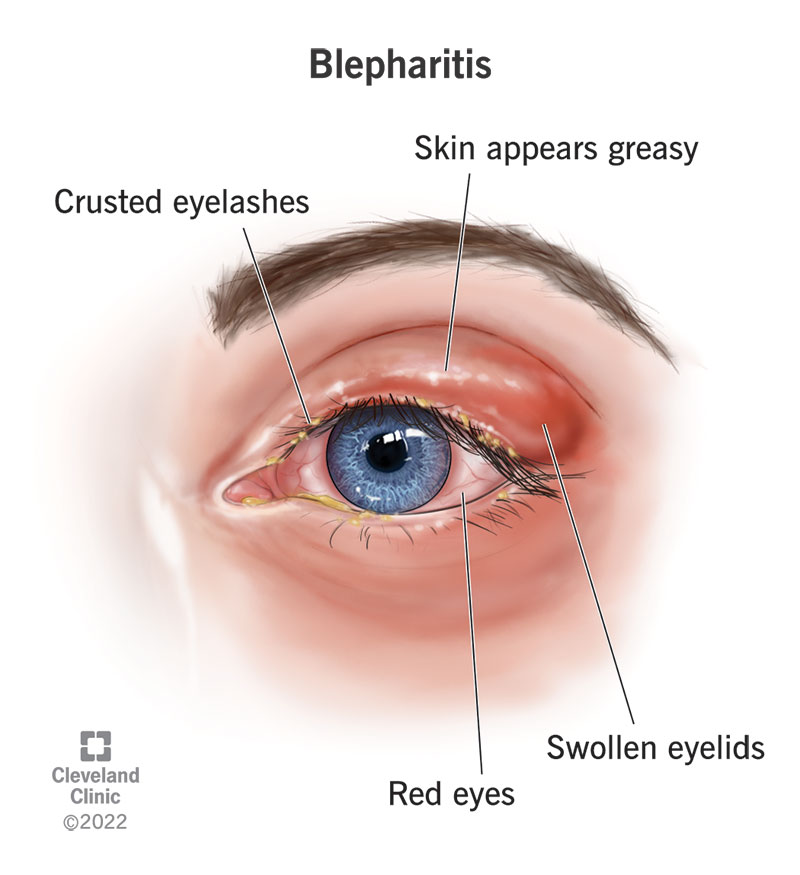
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/10032-blepharitis.jpg)
Blepharitis, pronounced bleh-fur-RY-tis, means inflammation of the eyelid. The edges of your lids turn red or dark in color and become swollen and scaly. Blepharitis usually affects both eyes. It can happen when a skin condition causes irritation, when you develop an infection or when oil glands become clogged. All of these things can even happen at once.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Blepharitis is a term for inflammation, but it can lead to an infection in your eye. However, most cases of blepharitis aren’t contagious. They aren’t likely to lead to blindness.
A survey of ophthalmologists and optometrists reported that nearly half of the people they see showed symptoms of blepharitis. The condition is common and symptoms are manageable.
Blepharitis typically affects adults and children of both sexes equally. However, one form — staphylococcal blepharitis — mainly affects females. This is true of about 80% of cases.
There are two types of blepharitis, depending on where it’s located on your eyelids. They are:
There are several signs and symptoms of blepharitis. They may include:
Advertisement
Other signs and symptoms may include:
Blepharitis can happen if you have issues with the meibomian glands that produce the oils found in tears, certain skin conditions or infections.
The symptoms you have may indicate a particular type of blepharitis: staphylococcal, seborrheic, ulcerative or meibomian. For instance:
In addition to having rosacea and dandruff, you may be more at risk of developing blepharitis if you:
Poor hygiene can be a factor in blepharitis, but it’s not as simple as saying that only people with poor hygiene can get blepharitis. Hygiene is just a part of the reason that some people get blepharitis.
If you think about it, most people don’t clean their eyelids and lashes every day or night. However, people with risk factors may have to make eyelid and eyelash hygiene a priority.
There’s no single test for blepharitis. Here are a few steps your eye care provider may take to find out if you have blepharitis and what type it is:
Advertisement
For some types of blepharitis, self-care at home may help soothe the symptoms. If you believe you have blepharitis, try these tips:
Alternatively, you can make your own lid scrubs at home. Follow these steps:
Advertisement
If cleaning your eyelids carefully for several days doesn’t get rid of the crusts, you should see an eye care provider.
Your blepharitis treatment will depend upon the type you have. After examining your eyelid swelling and running tests, your provider may prescribe treatments that include some or all of the following.
You may get a prescription for an antibiotic ointment — such as erythromycin, bacitracin ophthalmic or Polysporin® for your eyelid — or for antibiotic eye drops, such as a combination of polymyxin B and trimethoprim (Polytrim®). These treatments may help resolve the bacterial infection and reduce irritation. Cases that persist may require an oral antibiotic, such as doxycycline or azithromycin.
Your provider may add a steroid eye drop or cream to your treatment plan if you need stronger medicine. Steroids reduce inflammation. Your provider may prescribe both antibiotics and anti-inflammatories to treat underlying conditions or secondary infections.
Adding an immunomodulatory drug, such as cyclosporine ophthalmic (Restasis®) in cases of posterior blepharitis, has been shown to reduce inflammation. These drugs block your body’s natural immune response and therefore reduce inflammation.
Advertisement
It’s important to treat root causes that trigger blepharitis, in addition to soothing symptoms. Skin conditions (such as rosacea) or eye ailments (such as dry eye) can lead to blepharitis recurring more often. In these cases, certain pills, skin creams, or eye drops for dry eyes may help.
Your provider can do some newer procedures in their office. These include:
You can’t cure blepharitis. However, it can be treated and controlled through proper eyelid hygiene. Left untreated, blepharitis may lead to other more serious eye conditions, including corneal problems, which may be significant.
Complications include:
Many blepharitis cases aren’t preventable. Some risk factors for blepharitis, such as certain skin conditions, are beyond your control. Here are some steps you can take every day to help with the symptoms:
Blepharitis, with its symptoms of swollen, red, itchy eyelids, is never fun. However, in most cases, blepharitis is a condition that you can manage. If you can treat any underlying issues, and you practice good eyelid hygiene, you’ll likely have fewer flare-ups.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s ophthalmologists and optometrists have the highest training available. We provide exams, vision correction and care for many eye conditions.
