A barium swallow (esophagram) involves drinking a liquid that contains a small amount of barium. Barium makes your body parts show up more clearly on an X-ray. A fluoroscopic X-ray using short bursts of an X-ray beam provides footage of your esophagus as you swallow. The test is one of the ways your provider may diagnose issues with your esophagus.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
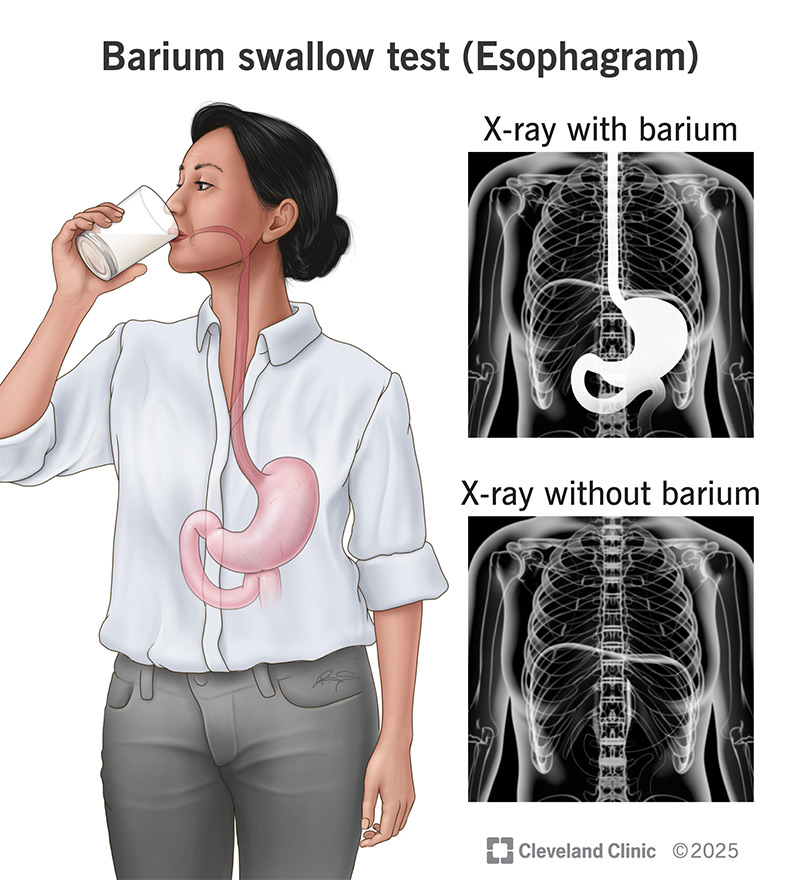
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/22766-esophagram.jpg)
A barium swallow is a test that shows what’s happening inside your esophagus when you swallow. It’s also called an esophagram.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
During a barium swallow test, you’ll drink a liquid with a small amount of barium in it. Barium is a substance that makes your body parts show up more clearly on X-rays. This type of X-ray is called a fluoroscopy. It uses short bursts of an X-ray beam to record your esophagus in action.
You may have this test if your healthcare provider thinks you might have a disorder affecting your esophagus. Common disorders include:
In a barium swallow (esophagram), a safe substance called barium gives your healthcare provider a view of the inside of your esophagus. As you swallow, video images of your esophagus appear on a computer screen.
Your technician may use a solution that contains barium and baking soda crystals (“effervescent granules”). The crystals produce gas, which helps inflate your esophagus. This makes it easier to see its lining. It also helps your radiologist better see narrowing, strictures and hernias.
Advertisement
Your technician may give you a barium tablet to swallow. This helps your radiologist spot narrowing and strictures.
You’ll meet with your healthcare provider so they can explain the esophagram procedure. They’ll ask if you’re allergic to barium. If you are, they’ll plan on using iodine (a mineral) as the contrast agent instead.
The test exposes you to a small, safe amount of radiation. But radiation exposure from X-rays can build up. It’s important that your provider knows about any recent X-rays. That way, they can schedule the barium swallow at the right time. Be sure to let them know if there’s a chance you may be pregnant.
The radiology department may ask you to:
This is an outpatient procedure with no sedation involved. That means you’ll go home the same day. Part of the test involves lying on a table that will tilt. So, you should wear comfortable clothes. The test steps are:
The barium swallow process takes about 20 to 30 minutes. At the end of the test, your provider may ask you to swallow a barium tablet with water. This is to check for esophageal strictures.
The barium solution may make your belly feel bloated or cause cramps. You may have constipation. These side effects should ease up as barium passes out of your body when you poop. Drinking lots of water after the test may help move things along. Don’t be alarmed if your poop is white. That’s just the barium leaving your body.
Your healthcare provider will let you know the test results. In a follow-up visit, they’ll explain what the results mean. They’ll discuss any next steps, like other tests or treatment.
Call your healthcare provider if you have test side effects that won’t go away, like a bloated belly. A barium swallow may not be the cause. But it’s always a good idea to notify your care team about esophagus or gut issues that don’t go away.
Difficulty swallowing or indigestion may mean there’s something going on in your esophagus. A barium swallow test (esophagram) is one way to find out what that something is. The test gives your healthcare provider a view of your esophagus in action. It doesn’t hurt, doesn’t involve sedation and doesn’t take long. And what your providers learn may be the first step toward helping you feel better.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Esophageal disorders can cause many symptoms, including heartburn or trouble swallowing. At Cleveland Clinic, we’ll find a treatment that works for you.
