Restless legs syndrome (RLS) is a movement condition that causes a strong urge to move your legs when you’re resting. You may also feel sensations like itching, pulling, crawling or throbbing. There isn’t a cure for RLS, but treatment is available.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Restless legs syndrome (RLS) is a brain, nerve and sleep condition that causes a strong, nearly irresistible urge to move your legs that’s at least partially relieved by movement. Symptoms are more common when your body is at rest in the evening. It usually occurs in addition to uncomfortable sensations in your legs like throbbing or aching. The urge to constantly move can interfere with your ability to relax or fall asleep.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
You may hear your healthcare provider call RLS restless leg syndrome or Willis-Ekbom disease.
There are two types of RLS:
Between 7% and 10% of the United States population has restless legs syndrome. It’s more common among white people and females. Your risk of developing it increases as you get older.
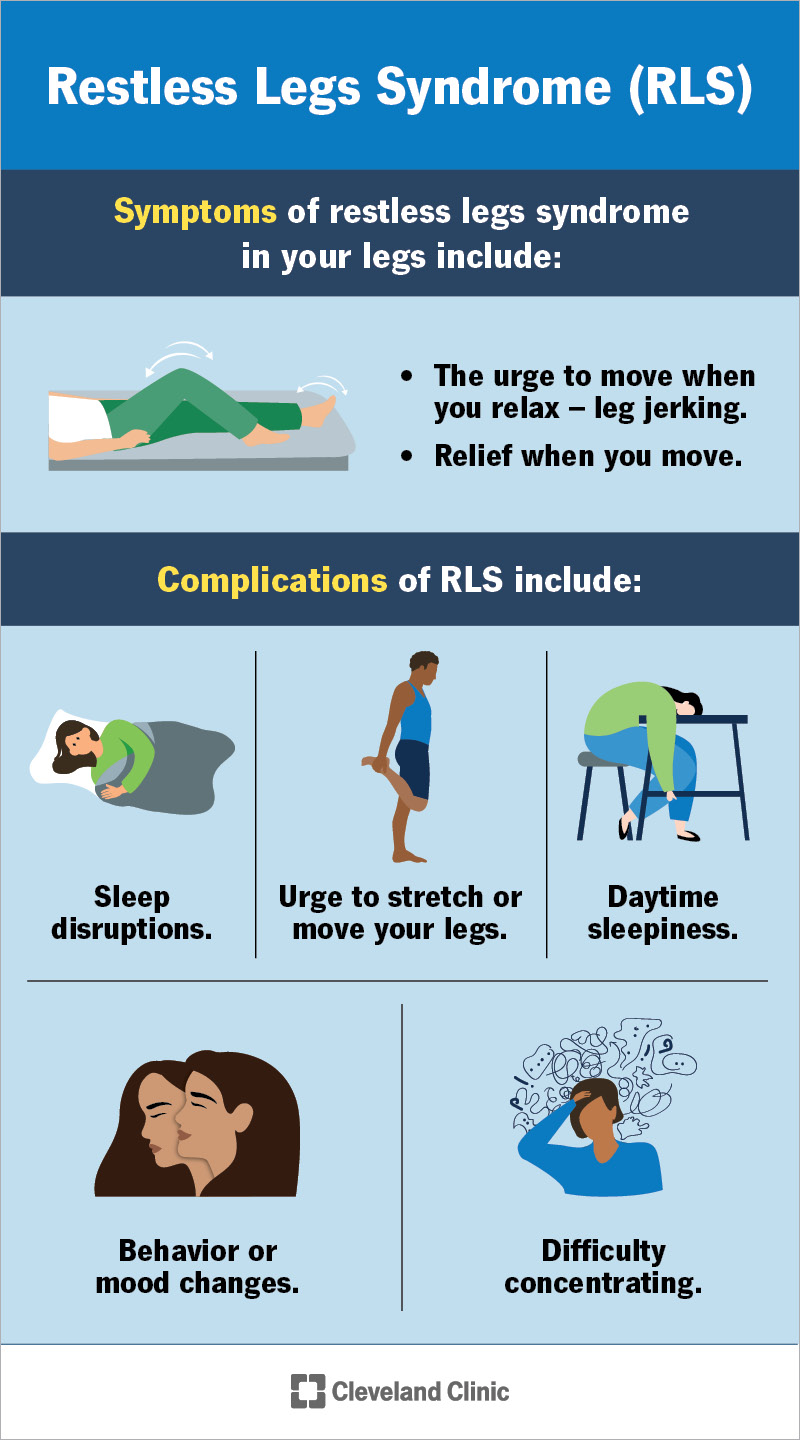
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/9497-restless-legs-syndrome)
Symptoms of restless legs syndrome include:
Symptoms of restless legs syndrome can affect your sleep. This can cause:
Restless legs syndrome causes sensations that make you want to move your legs. These sensations most often happen in your legs, but they can also affect your arms or your entire body. You may experience the following feelings:
Advertisement
Sensations can happen on one side of your body, but more commonly affect both sides equally, like both legs.
The cause of restless legs syndrome isn’t well understood. It may relate to how the part of your brain that causes movement (basal ganglia) functions. The basal ganglia use dopamine to regulate how your body moves. If this part of your brain doesn’t get enough dopamine, it isn’t able to regulate your movement as efficiently as it should. This can lead to RLS symptoms.
Research suggests the following may contribute to RLS:
Some medical conditions can happen in addition to RLS, including:
Triggers are things that make your RLS symptoms worse. Possible triggers can vary but could include:
If you experience these triggers or use/take them before you rest or go to bed, they’re more likely to set off your symptoms. In addition, a lack of sleep can lead to worsening symptoms. This means that your symptoms can trigger worsening symptoms. If you need help identifying what triggers your symptoms, talk to a healthcare provider.
Restless legs syndrome can affect anyone, including children, adolescents and adults. It’s more common to affect people after age 50. Symptoms tend to get worse as you age.
A healthcare provider will diagnose RLS after a physical exam to review your symptoms. During the exam, they’ll take a complete medical history and family medical history.
As there isn’t a test to diagnose RLS, a healthcare provider may offer a neurological exam and blood tests to rule out other conditions or determine the cause of your symptoms. Your provider may recommend an overnight sleep study to evaluate other possible sleep conditions. However, RLS is a clinical diagnosis that doesn’t require sleep testing.
To confirm a diagnosis of RLS, a healthcare provider will look for the following criteria:
Advertisement
Yes, it’s sometimes difficult for healthcare providers to diagnose RLS in children. This is because a child may not be able to describe their symptoms or what they feel. It’s common for RLS in children to look like attention-deficit/hyperactivity disorder (ADHD) or growing pains.
Treatment for RLS may include taking medications or changing your routine at home to help relieve your symptoms. Some people may reduce their symptoms if they work with their healthcare provider to manage other underlying health conditions. You and your healthcare provider will discuss the treatment options that might be best for you, as well as any side effects to look out for.
Certain medications can help relieve your symptoms of RLS. Your healthcare provider may recommend or prescribe the following:
Advertisement
Certain medications like benzodiazepines (clonazepam), hypnotics (zolpidem) or opioids (methadone, buprenorphine) may help with severe cases if all other forms of treatment are ineffective. The side effects of these medications may be harmful and can lead to dependence on the medication.
There are many types of iron supplements. Blood tests can help to identify the best type for you. When levels of iron in your brain are suspected to be very low and RLS symptoms are severe, an iron infusion may help.
Medications that increase dopamine can worsen RLS symptoms over time (augmentation). Close monitoring is required.
If you have mild RLS symptoms, a healthcare provider may recommend the following at-home therapies to help you feel more comfortable and fall asleep with restless legs. These may include:
Advertisement
Moving your legs can temporarily relieve restless legs immediately, but your symptoms often return when you stop moving. You can also try massaging your legs, walking around or stretching.
Restless legs syndrome doesn’t affect your life expectancy, but it can affect your overall wellness. Symptoms may be mild to severe. Even mild symptoms can have a major impact on your life. Depending on what your definition of a “serious” medical condition is, your symptoms may fall into this category.
There’s no cure available for RLS, but treatment can help manage your symptoms.
There’s no known way to prevent restless legs syndrome. You can reduce your risk of experiencing worsening symptoms by treating any underlying health conditions or avoiding triggers like caffeine and alcohol.
Visit a healthcare provider if you have symptoms of RLS that:
Living with restless legs syndrome (RLS) can be a constant annoyance. It interferes with your ability to fall asleep and stay asleep. When your alarm goes off in the morning, you may wish you could hit the snooze button a few more times. Drinking coffee (caffeine) to cope in the morning may make your symptoms worse at night. While there isn’t a cure available for RLS, treatment can help you manage your symptoms, feel better and get back to a regular sleeping routine.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Sleep-movement disorders cause involuntary muscle spasms, twitches and cramps. Cleveland Clinic’s sleep specialists treat these conditions so you can rest easy.
