Hip fractures (broken hips) are medical emergencies. Even though they’re very common, they can be life-changing injuries for people — especially adults older than 65. Almost everyone who breaks a hip needs surgery to repair the fracture. Many people need a hip replacement. It usually takes a few months to recover after surgery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
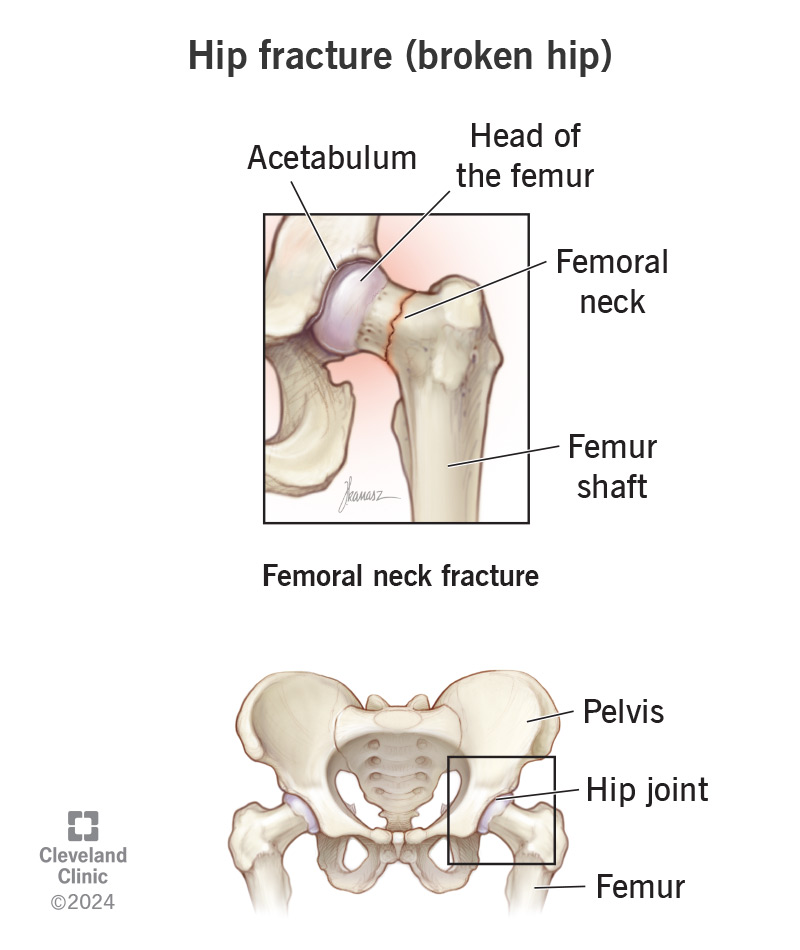
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17101-hip-fracture)
A hip fracture is the medical name for breaking the upper part of your thigh bone (femur) near your hip joint.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Your femur is the longest and strongest bone in your body, so it usually takes a serious fall, car accident or other trauma to break it. You’ll almost always need surgery to repair a hip fracture.
People sometimes joke about broken hips as shorthand for a friend getting older. This is usually just playful teasing, but it’s important to remember that broken hips are serious, potentially life-changing injuries.
Your hip is a ball-and-socket joint. The ball-shaped top (the head) of your femur fits into a socket (the acetabulum) in your pelvis. A broken hip is a broad category that means any type of bone fracture that affects the upper part of your femur.
Healthcare providers classify broken hips based on where the femur breaks:
Advertisement
Providers may also give a hip fracture a name based on the fracture’s pattern (its shape or direction), including:
The most common hip fracture symptoms include:
It usually takes severe trauma to break your hip. The most common causes of hip fractures include:
Anyone can experience sudden trauma and break a hip, but some people are more likely to, including:
It usually takes a fall from a big height (like off a ladder or roof) to fracture your hip. But adults older than 65 or people with health conditions that weaken their bones are much more likely to break a hip after minor slips and falls at home or in their daily routines.
Any health condition that affects your balance, stability or ability to walk and move (your gait) can increase your risk of breaking a hip. Some conditions that can reduce your stability include:
A healthcare provider will diagnose a broken hip with a physical exam and imaging tests. Providers in the emergency room might diagnose the fracture in the ER if you experience a severe fall or other trauma.
Your provider will use at least one of the following types of imaging test to take pictures of your hip and the area around it:
Almost everyone with a hip fracture needs surgery. Which type of surgery you’ll need depends on the fracture’s severity and type, and if you have any other injuries or health conditions. The two most common surgeries for hip fractures include:
Advertisement
Hip fracture surgery complications can include:
It usually takes at least a few months to recover from a broken hip. You may feel and notice improvements gradually over a year after treatment. How long it takes you to recover will depend on a few factors, including:
Your surgeon will tell you what to expect and give you a recovery timeline that matches your unique needs.
You’ll start physical therapy (PT) soon after surgery. You may need PT for several months to help you regain your ability to move and walk. A physical therapist will give you exercises and stretches to strengthen the muscles around your hip.
You may need a walker, cane or crutches while you recover from surgery. Some people need them for longer. Ask your surgeon or physical therapist how long you should use mobility aids.
Advertisement
Hip fractures are emergencies. In addition to the damage to your femur and hip joint, hip fractures often happen alongside other major injuries. That’s especially true if you experience a severe fall or car accident.
Any injury severe enough to break your femur may also damage your femoral artery. This can cause a fatal amount of blood loss if a healthcare provider doesn’t treat it immediately. A broken hip can also increase your risk of blood clots.
The kinds of trauma that cause hip fractures can be especially dangerous for adults older than 65. The older you are, the longer it takes your body to heal any injury, and that’s especially true when you have a major one like a hip fracture. The surgery to treat a hip fracture (and the recovery from it) can be harder for an older adult, too.
Studies have found that adults older than 65 who’ve experienced a hip fracture are more likely to reduce or stop physical activity like walking and to cut back on social activities and hobbies, even after they recover. This isolation can impact your overall health. Talk to your provider about how to stay active after you’ve had a hip fracture. They can suggest safe ways to stay engaged with your loved ones and favorite activities.
Advertisement
You may not always be able to prevent hip fractures, especially because sudden falls or other trauma you can’t plan for cause them. Follow these general safety tips to reduce your risk of falls and injuries:
All hip fractures are medical emergencies. Call 911 (or your local emergency services number) if you think you have a broken hip. Call emergency services if you experience a fall, car accident or another trauma and experience any of the following symptoms:
Questions you may want to ask your provider include:
You can’t stand, walk or put weight on a broken hip. Putting pressure on your hip can make the fracture worse and cause other complications and injuries.
Your surgeon or healthcare provider will show you how to safely stand, walk and move after surgery and while you recover.
Call 911 (or your local emergency services number) if you think someone has a broken hip. Only trained healthcare professionals should move, lift or transport someone who has a broken hip. Try to keep the person’s hip stable and supported. Don’t put any pressure on their leg or try to get them to stand or walk.
Ask the dispatcher or operator who answers your emergency call for tips on keeping the person safe and stable while you wait for help to arrive.
A hip fracture can be a scary, shocking injury. That’s especially true because they usually happen in a split second in a sudden fall or car accident. Recovering from hip surgery can be long and hard work. Celebrate each milestone along the way during your recovery journey. Tell your provider or physical therapist if you’re struggling with any type of movement or exercise. They’ll help you work through any challenges you face.
You don’t need to live in fear of a hip fracture, but it’s important to know what can cause one and how to reduce your risk. Talk to your healthcare provider about regular screenings that can catch changes in your bone density or overall health before they cause an injury.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
From sudden injuries to chronic conditions, Cleveland Clinic’s orthopaedic providers can guide you through testing, treatment and beyond.
