Shoulder tendonitis (tendinitis) is inflammation in your rotator cuff or biceps tendon. The condition frequently occurs due to sports injuries and overuse or repetitive motions. Symptoms range from mild to severe. Treatment starts with noninvasive measures like rest, ice and pain medications. Surgery may be necessary for more severe cases.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
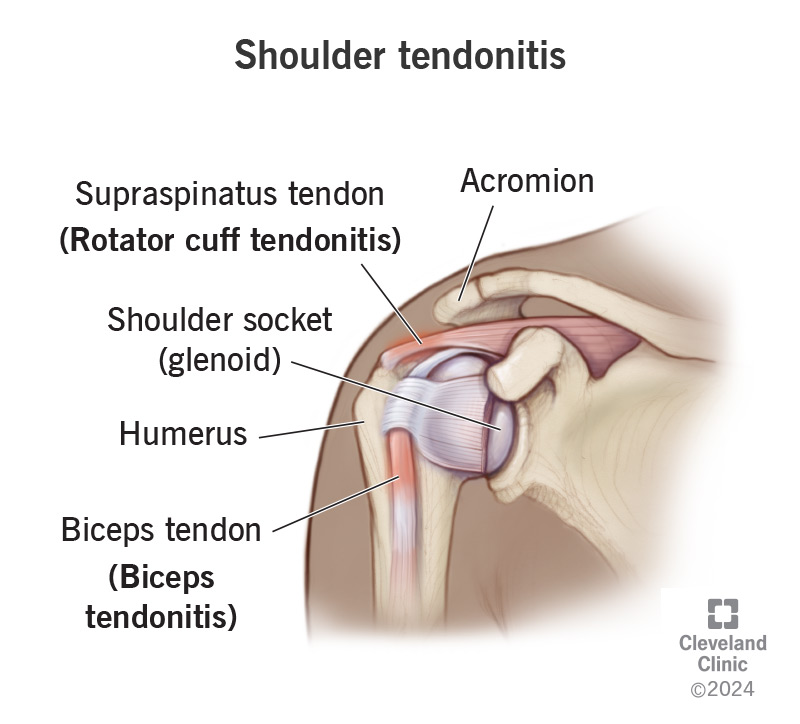
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/shoulder-tendonitis)
Shoulder tendonitis (tendonitis) is inflammation that affects an area within your shoulder joint. Your shoulder joint is kept stable by a group of muscles called the rotator cuff, as well as the biceps tendon. These muscles and tendons keep your upper arm bone (humerus) within your shoulder socket (glenoid).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Tendonitis in your shoulder occurs when inflammation traps or pinches the muscles and tendons against the top bone in your shoulder (acromion). When your rotator cuff tendons become inflamed and irritated, it’s called rotator cuff tendonitis. When your biceps tendon becomes inflamed and irritated, it’s called biceps tendonitis.
Shoulder tendonitis symptoms range from mild stiffness to severe pain. You may feel pain at the tip of your shoulder or radiating down your arm. You may feel the pain when you lift your arm overhead or twist it. Other symptoms may include:
Shoulder tendonitis often occurs as a result of sports injuries, where an athlete must move their arm over their head repeatedly. Sports where this frequently occurs include:
Improper technique in any sport is one of the primary causes of overload on tissues, including tendons, which can contribute to tendonitis.
But you don’t have to be a professional athlete to develop this condition. People with jobs that require overhead work (such as assembly work or an overhead pressing machine) or heavy lifting are at risk of tendonitis, but any person can develop tendonitis from repetitive use of these tendons. A direct blow to your shoulder area or falling on an outstretched arm can also cause shoulder tendonitis.
Advertisement
As we age, our tendons naturally become less flexible, so your risk of shoulder tendonitis goes up. Other risk factors include:
If left untreated, shoulder tendonitis can lead to complications, including:
A healthcare provider will ask about your medical history and perform a physical exam. Depending on their findings, they may also order tests, including:
Your healthcare provider may use the following stages to classify your condition:
Shoulder tendonitis treatment depends on several factors, including your age, symptoms and severity of your condition. Your healthcare provider may recommend a combination of rest, wraps and ice packs for recent or severe injuries. Other nonsurgical treatment options include:
Your provider may recommend surgery if either your rotator cuff or biceps tendon has partially or completely torn and your symptoms don’t improve with other treatments. Surgery repairs the damaged tendon or tendons and removes inflamed bursae that may also be irritating your shoulder.
The time it takes shoulder tendonitis to heal depends on the severity of your injury. Mild cases may start to heal with nonsurgical treatment methods within two to four weeks. But it can take several months in more severe situations. Your healthcare provider can give you a clearer picture of your prognosis.
Advertisement
You should rest your shoulder until you no longer have any pain or other symptoms. When you do go back to work, sports or other activities, take it easy. Make sure to warm up your shoulder with flexibility exercises. Try to avoid lifting your arm over your head, and don’t participate in the activity for too long. Make sure to get plenty of rest. Take your time, and gradually increase your level of activity.
Because most cases of shoulder tendonitis are caused by overuse, the best treatment is prevention. It’s important to avoid or modify the activities that cause the problem. You must correct underlying conditions, like improper posture or poor technique in sports or work.
Apply these basic rules when performing activities:
Most cases of shoulder tendonitis go away on their own over time. It may take weeks to months to recover, depending on the severity. See your healthcare provider if you:
Advertisement
If you have shoulder tendonitis, you may want to ask your provider:
Having tendonitis in your shoulder can be frustrating, especially when it prevents you from participating in a sport you love. You’ll need to rest your shoulder for several weeks to allow your tendon to heal. This can be challenging, but it’s important not to return to the playing field until your healthcare provider gives you the go-ahead. You don’t want to risk further injury. Follow your provider’s instructions, and you’ll be back at it in no time.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic experts are here to treat your tendinopathy (tendon pain) and get you back to doing the things you love.
