Shingles is nerve pain and a rash caused by the varicella-zoster virus, the same virus that causes chickenpox. If you’ve had chickenpox in the past, you could get shingles. Early symptoms include burning pain, tingling and discoloration. You might get a headache or fever not long before the rash appears.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
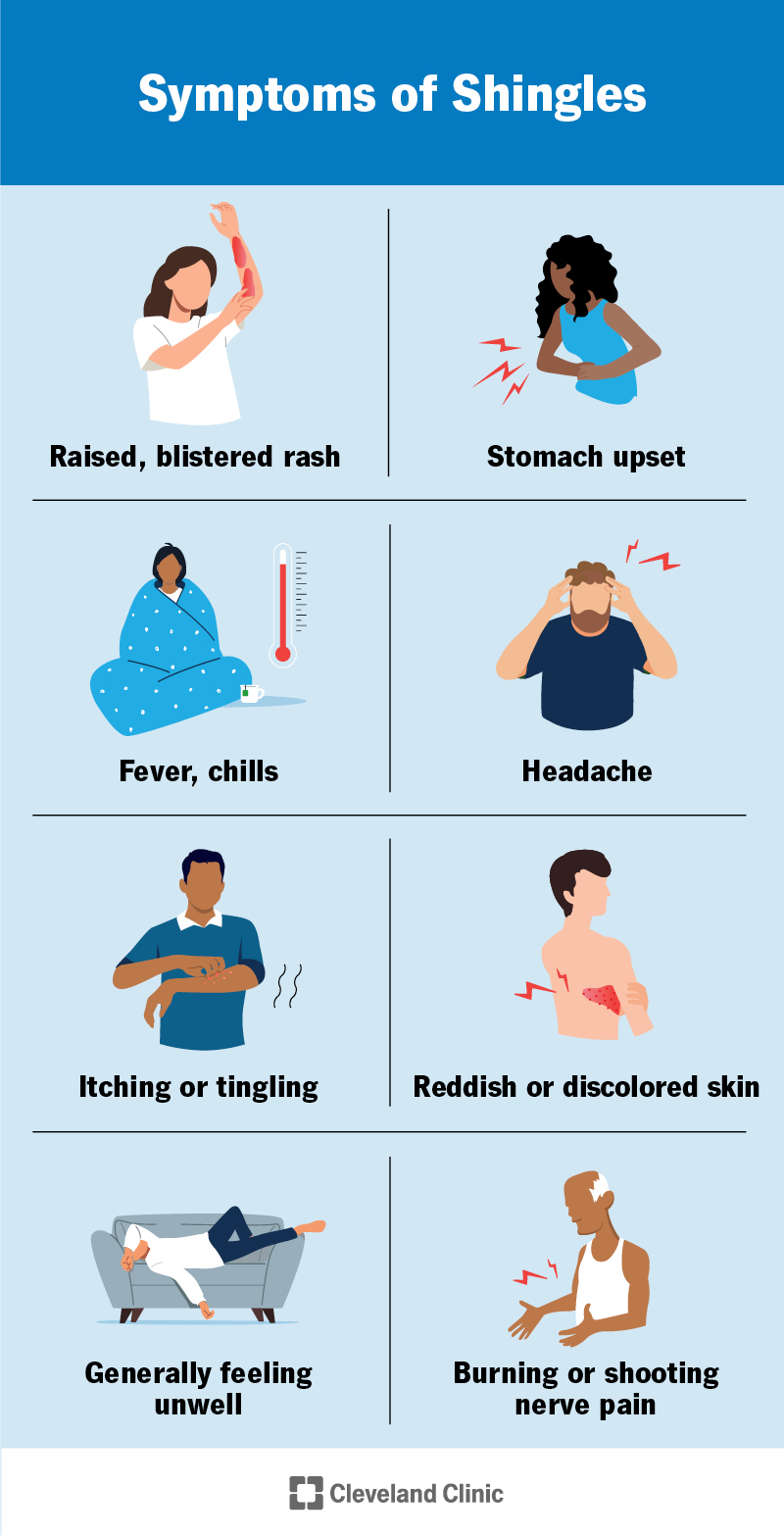
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/shingles)
Shingles is a viral infection that causes a painful rash and nerve damage. It’s also called herpes zoster.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Shingles is caused by the same virus that causes chickenpox. It stays inactive in your body and can reactivate in your nerves later in life. So, if you’ve had chickenpox before, you could get shingles.
A painful, raised or blistered rash is the most common symptom of shingles. It might appear near your waist or on one side of your face, neck, chest, belly or back. Sometimes, it shows up on other parts of your body.
Other symptoms that can appear before or along with the rash include:
Some early symptoms, like nerve pain and discoloration, can appear weeks before the rash. Others might show up in the days leading up to it. The rash turns into blisters about three to four days after it appears. Within about 10 days, the blisters dry out and crust over into scabs. The scabs may take a few weeks to completely go away.
Some people don’t get a rash with shingles. See a healthcare provider if you have symptoms of shingles, even if you don’t have the rash.
Varicella-zoster virus (VZV) causes shingles. After having chickenpox, VZV stays in your body after your symptoms go away. It hides in your nerve cells, inactive (dormant). Sometimes, the virus reactivates later in life, causing shingles.
Advertisement
Experts aren’t always sure why the virus gets reactivated. But it tends to happen as you get older and your immune system naturally starts to weaken.
You can’t spread shingles to someone else, but you could give them chickenpox if you have shingles. Varicella-zoster virus can spread through direct skin-to-skin contact with fluid from the blisters or from breathing in particles from the blisters. Someone who hasn’t had chickenpox before can get infected with the virus.
Anyone who’s had chickenpox can develop shingles. But you’re at a higher risk if you:
Some experts think that stress plays a role in developing shingles, but this is hard to prove.
The most common complication of shingles is nerve pain that doesn’t go away when the rash does (postherpetic neuralgia). This can last for months or years and can be extremely painful.
Other complications include:
Rarely, shingles is fatal.
Healthcare providers diagnose shingles by learning about your symptoms and looking at the rash. If the rash follows the line of dermatomes (areas of skin along a nerve) and doesn’t cross the midline of your body, that’s a clue that it’s shingles. Your provider may also send scrapings or a swab of the fluid from the blisters to a lab for diagnosis.
There’s no cure for shingles. Your provider might recommend managing the symptoms with:
If you have symptoms of shingles, see your healthcare provider right away. Starting antiviral medications as soon as possible can help you feel better faster.
Go to the emergency room if you have symptoms of serious complications, including:
It can take three to five weeks from the time your first symptoms start until the rash totally disappears. Your other symptoms might start getting better in seven to 10 days.
Advertisement
Most people with shingles get better without any complications. Taking antivirals within three days of the start of your symptoms might help you feel better sooner. But some people get very sick and have to stay in the hospital to recover. Up to 1 in 5 people with shingles experience long-term nerve pain.
If you’ve had chickenpox, you can reduce your risk of shingles by getting a shingles vaccine (Shingrix®). It’s recommended even if you’ve already had shingles or if you’ve already gotten Zostavax®.
Until the rash has gone away completely, keep it covered and avoid being around people so you don’t spread the chickenpox virus.
Yes, you can get shingles more than once. But it’s not common unless you have a weakened immune system. If you get shingles again, you usually don’t get the rash in the same place.
No, you can’t get shingles if you haven’t had chickenpox. Rarely, people who got the chickenpox vaccine can get shingles years later.
Just when you thought chickenpox was a distant childhood memory, it comes back with a painful reminder. Not only is it unpleasant for you; it also risks spreading chickenpox to those who haven’t been exposed to the virus, like infants and young kids.
Advertisement
Most people get through shingles without long-term complications. But it’s important to keep an eye on your symptoms and know when to seek emergency medical care, especially if you have a weakened immune system. Talk to a healthcare provider as soon as your symptoms start. They might be able to help ease your symptoms while you get better.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Need care fast? Cleveland Clinic’s Express Care and Urgent Care locations treat everything from sprains to sinus infections — no appointment needed.
