Sam Drinnon first “met” her unborn son, Rylan, about 10 weeks before she gave birth. Deeply anesthetized, Sam underwent a fetal interventional surgery at Cleveland Clinic on May 7, 2021, during which Rylan’s arms and shoulders were gently lifted out of her uterus while his head remained inside. That enabled a multidisciplinary surgical team led by Darrell Cass, MD, to gain access to the chest of the 26-week-old fetus. Surgeons performed a life-saving procedure by removing the tumor growing on his heart.
Few studies about the rare condition – an intrapericardial teratoma with fetal hydrops (fluid accumulation) leading to fetal heart failure – have been reported in medical journals. Dr. Cass states Cleveland Clinic is the second academic medical center in the world to have performed this fetal surgery successfully with continued pregnancy and delivery.
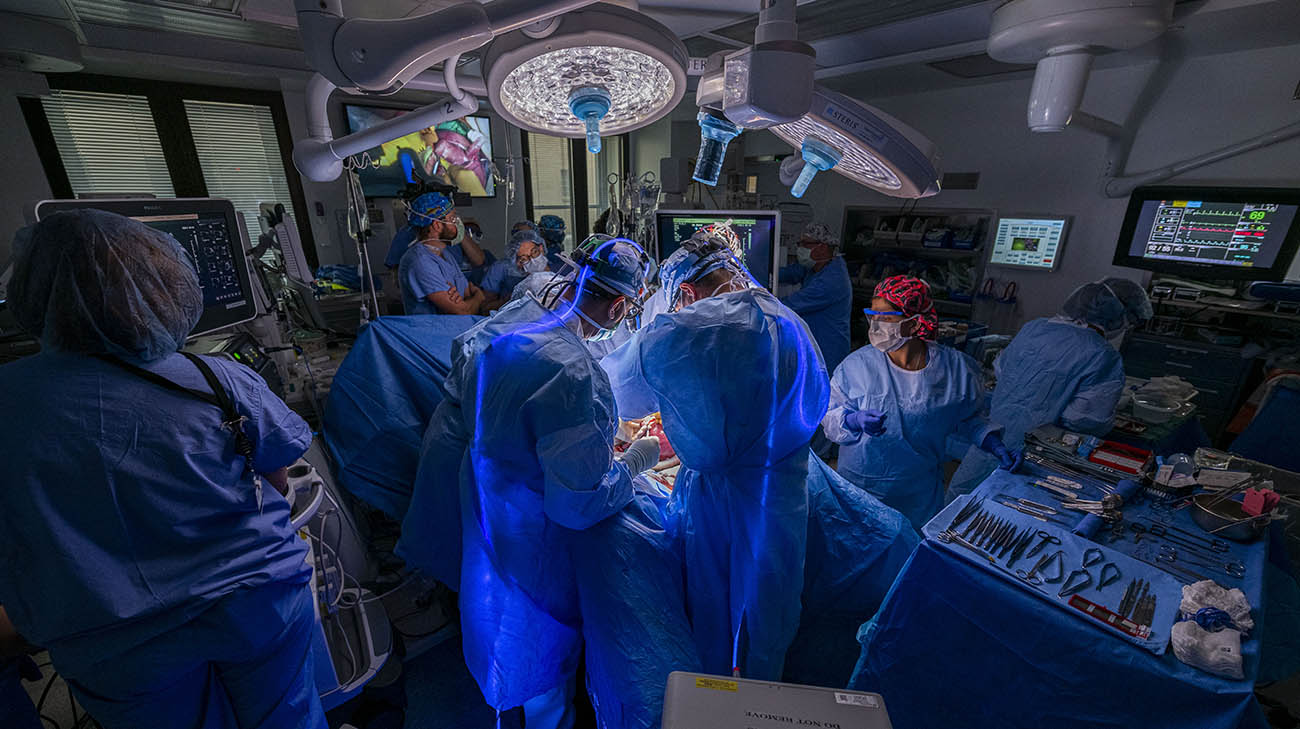
A multidisciplinary team of Cleveland Clinic and Cleveland Clinic Children’s doctors and nurses performed a rare and complex lifesaving fetal surgery to remove a tumor attached to the heart of a 26-week-old fetus. (Courtesy: Cleveland Clinic)
“It is certainly an amazing story,” says Dr. Cass, director of Cleveland Clinic’s Fetal Surgery and Fetal Care Center. “We see this condition in less than one in 100,000 pregnancies. These tumors can occur in the central portion of the chest, outside of the pericardial sac, which surrounds the heart, or they can be on the inside. Rylan’s was on the inside, which is a worse situation as you might imagine.”
A week before the surgery Sam had experienced a fairly uneventful second pregnancy until a routine ultrasound, in late April 2021, at a doctor’s office close to home, revealed a mass inside his heart.
“A lot of emotions came very quickly,” recalls Sam, remembering how she felt breaking the news by phone to Rylan’s father, Dave Drinnon. “I thought I was going to lose my baby, but the doctors said they would get me to the best team to get it taken care of.”

When Sam Custer was 25 weeks pregnant, doctors discovered a large tumor attached to the heart of her unborn baby. (Courtesy: Ed and Cassie Custer)
Doctors referred Sam to Cleveland Clinic, where Dr. Cass quickly assembled a team of experts to determine if and how they could treat the incredibly rare condition. Based on input from pediatric and congenital heart surgeons Hani Najm, MD, (who ultimately removed the tumor) and Alistair Phillips, MD, pediatric cardiologist, Francine Erenberg, MD, maternal-fetal medicine specialist, Amanda Kalan, MD, and obstetric and pediatric anesthesiologists McCallum Hoyt, MD, Tara Hata, MD, and Yael Dahan, MD, the team decided the best treatment to save Rylan’s life was open fetal resection of the tumor.
Imaging revealed the tumor was compressing the left side of the fetus’s heart and impairing circulation. For several days, the team followed Sam very closely with consistent evaluations of the pregnancy and fetal heart function. Unfortunately, the tumor continued to grow and the situation became more critical. Fluid progressively accumulated around the heart and other organs, a condition called fetal hydrops. Rylan’s heart function showed signs of worsening. The team considered other options, including draining the fluid, but knew the problem would soon recur if the tumor remained and results of the intervention were poor.
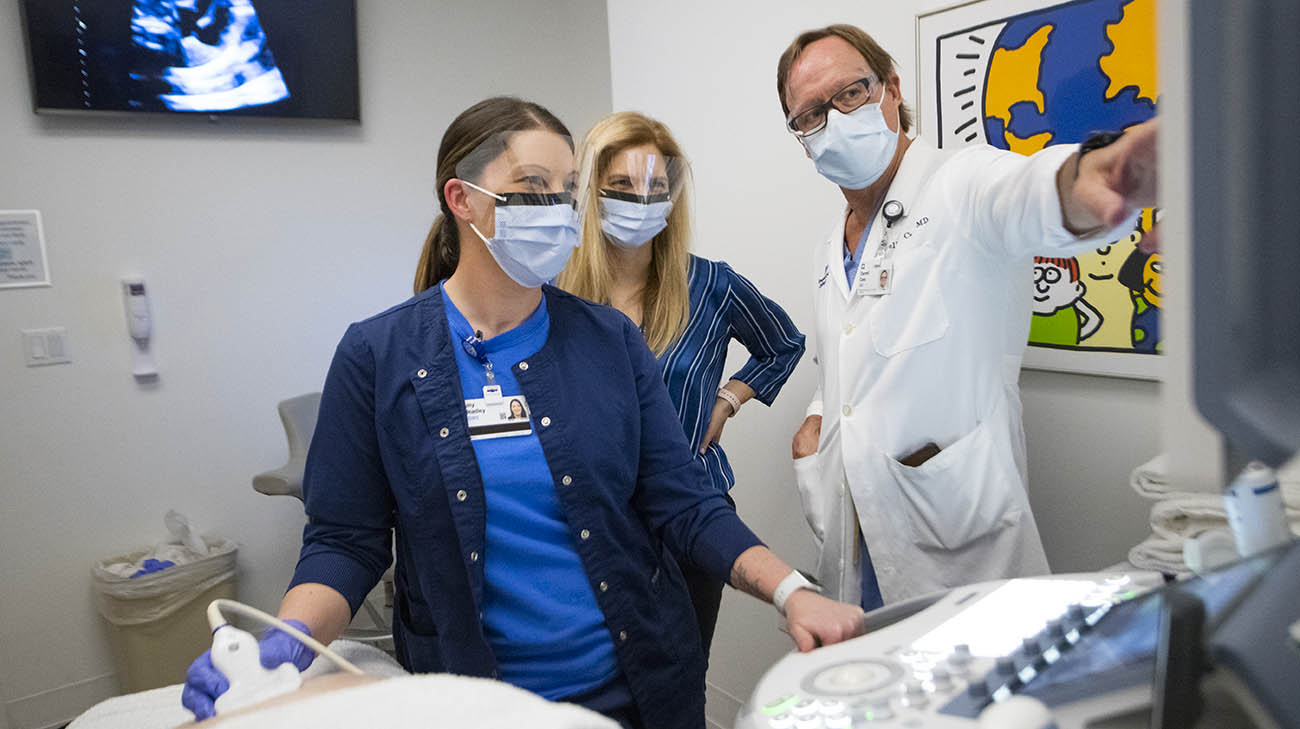
Drs. Cass and Kalan review scans during Sam's ultrasound appointment, after she underwent fetal surgery. (Courtesy: Cleveland Clinic)
According to Dr. Najm, who had successfully resected intrapericardial teratomas in babies but had never attempted the procedure on a fetus, time was of the essence. “From the imaging, I could see that the tumor was getting bigger, and fluid was collecting in his pericardium and lungs, which is an indication of heart failure. Even though this had rarely been done before, the fact we have a life that may not survive otherwise makes me always want to do something.”
After numerous discussions among the team members, the surgery was scheduled within 36 hours. While Sam and Dave were nervous, they knew the procedure would be the best chance they had at a favorable outcome. “It was very nerve-racking,” Dave says, “because there is so much uncertainty going into that kind of a surgery. But Dr. Cass and the team showed so much confidence, it was very reassuring.”

Sam's care team gathers in pre-op to reassure her they're going to do everything they can to get the best possible outcome. (Courtesy: Cleveland Clinic)
The procedure began similar to a Caesarean section delivery, with Dr. Cass first making an incision to expose Sam’s uterus. Using ultrasound to pinpoint the exact location of the placenta and fetus, the surgeons opened her uterus with a 12 cm incision. Then, they carefully removed enough of the fetus’s body for Dr. Najm to gain access to the tiny chest and heart.
“I did ask Dr. Cass a simple question: ‘Can you actually get me access to his chest safely?’ He said, ‘Yes. I can.’ And I said, ‘I will do my part.’ That’s why it ended up being a great surgery,” observes Dr. Najm.
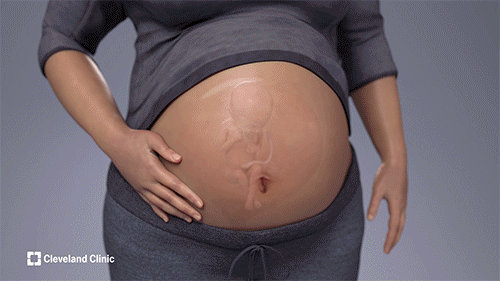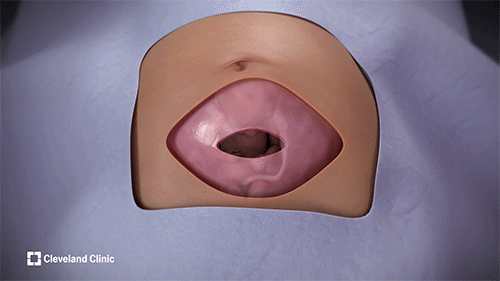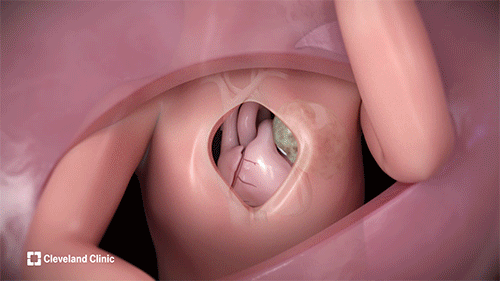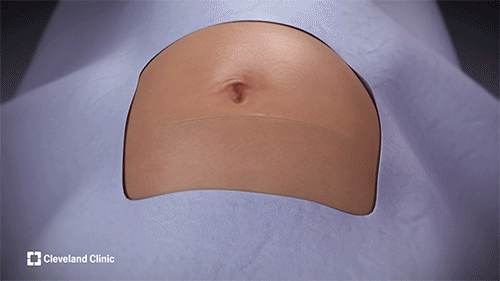
During fetal intrapericardial teratoma resection, surgeons intricately remove the tumor, which had been compressing the left side of the fetus’s heart and impairing circulation, leading to fluid accumulation around the heart and other organs of the fetus. (Courtesy: Cleveland Clinic)
Since fetal tissue at 26 weeks gestation is delicate and fragile, Dr. Najm had to proceed meticulously. First, he managed to insert an IV line into the fetus’s right arm in order to deliver anesthesia, fluids and medications, if needed. Then, he carefully opened the chest through a tiny incision.
Working as expeditiously as possible, as the fetus’s heart rate was declining, Dr. Najm drained the fluid in the pericardium and removed the tumor. He saw immediate results. “All of a sudden, the heart actually got back to normal beating,” he says. “The compression of the left atrium disappeared and there was nice blood flow.” He then inserted a temporary drain and closed the chest and skin.
His task completed, Dr. Najm stepped aside and Drs. Cass and Kalan took over, reinserting the fetus fully inside the uterus and then closing the incisions in Sam’s uterus and abdomen.
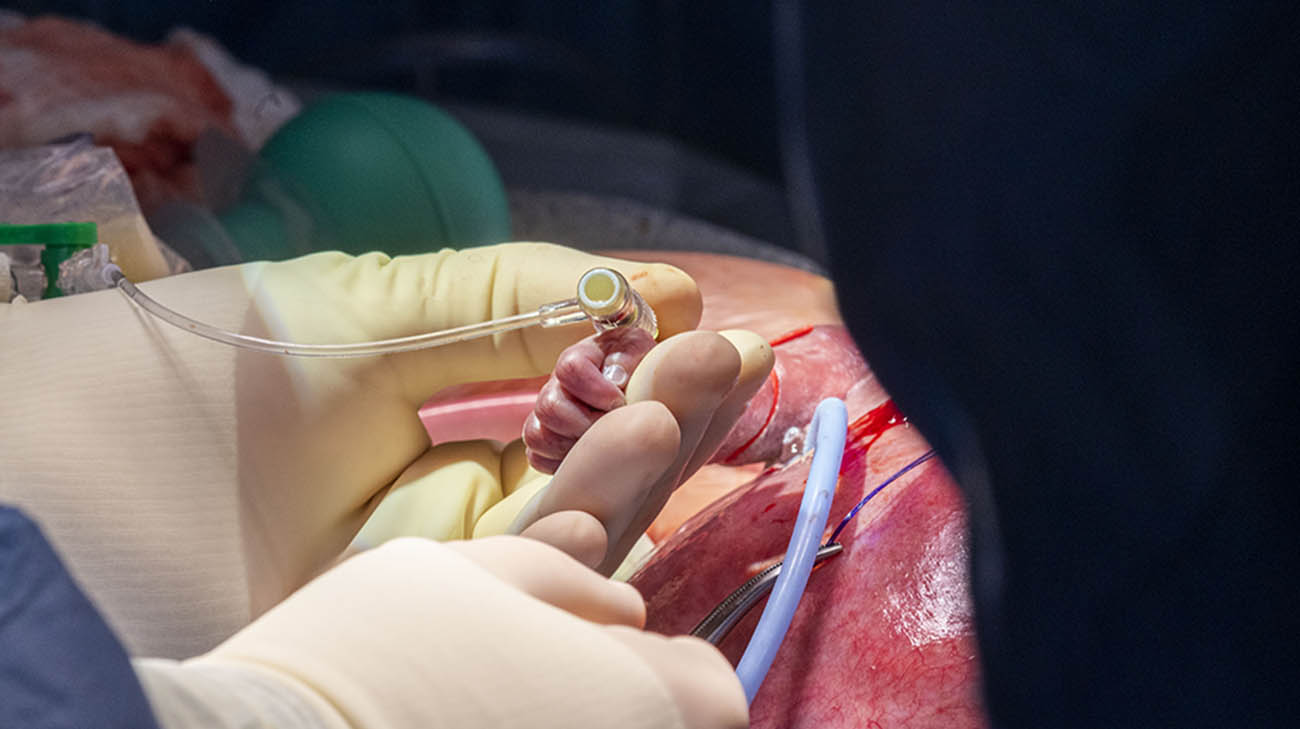
Dr. Najm inserts an IV line in the fetus’s right arm to deliver fluids and medications as needed. (Courtesy: Cleveland Clinic)
“I remember them wheeling me back into my room and asking them if he was still inside of me,” says Sam. “They told me that he was, and that made me feel a lot better.”
Home a few days later, Sam maintained a healthy pregnancy for about 10 weeks. At 36 weeks and two days (nearly full term), “I texted him (Dave) right before he's about to leave for work, and I go, ‘I think I'm in labor,’” Sam recalls. Rylan Harrison Drinnon was delivered by C-Section on July 13, 2021, weighing 6 pounds, 4 ounces.
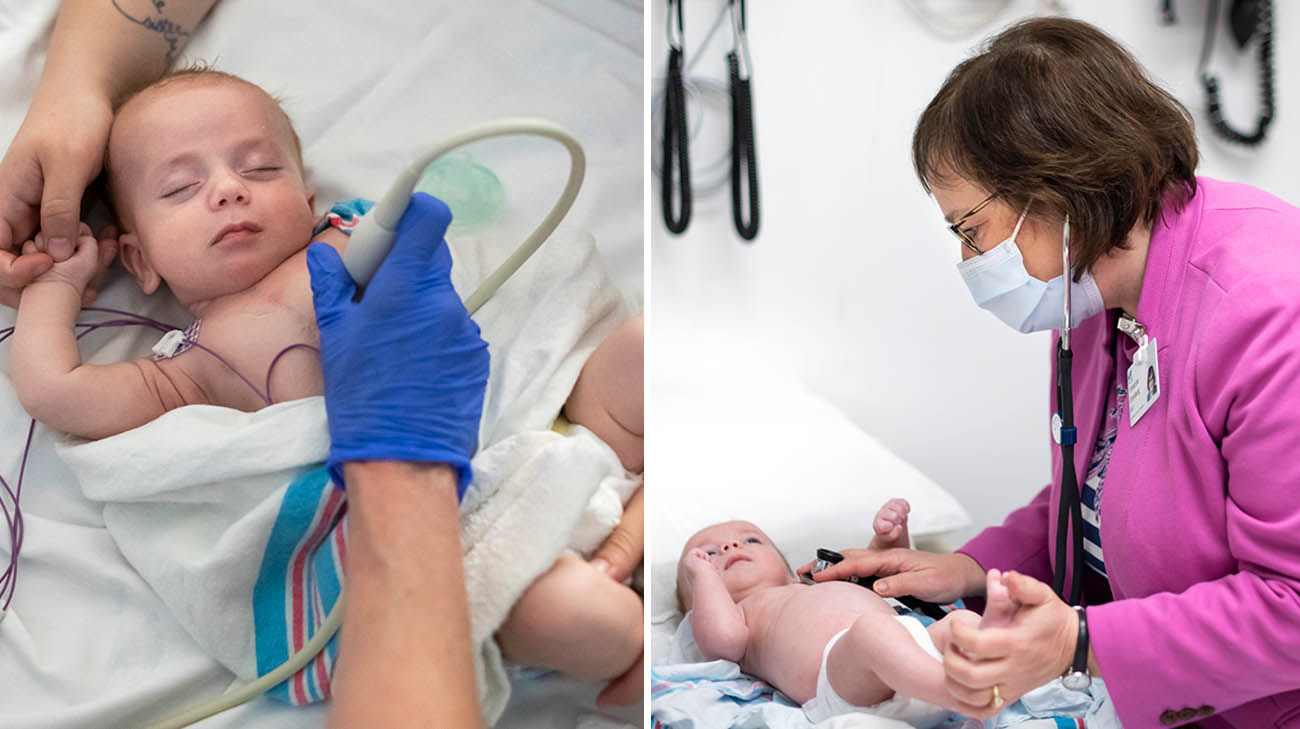
Rylan undergoing an echocardiogram (left) and during a follow-up appointment with Cleveland Clinic Children's cardiologist, Dr. Erenberg (right). (Courtesy: Cleveland Clinic)
Closely observed for a few days in Cleveland Clinic Children’s neonatal and pediatric intensive care units, Rylan went home and has experienced only minor complications. Eventually, he will need an operation to reposition the area of his sternum impacted by the operation. “We're going to continue to monitor him, make sure things are OK. But there's no sign of any problem,” adds Dr. Cass.
Dr. Phillips, the pediatric and congenital heart surgeon who assisted Dr. Najm, says seeing joy on the faces of Rylan’s parents, upon his delivery, will be a lasting memory for him. “For this family to have such a healthy baby was the culmination of meticulous planning, amazing teamwork and the incredible skills of so many.”

Rylan Harrison Drinnon was born on July 13, 2021, weighing six pounds, four ounces. (Courtesy: Cleveland Clinic)
Sam is grateful that Rylan – who, coincidentally, shares his middle name, Harrison, with the first name of Dr. Cass’ son – beat the odds and is thriving. “Hopefully, he gets to live the life of a normal kid, just with a scar on his chest,” Sam says. Adds Dave, “I get to come home from work every day and see my son. He's already had to go through a lot to get to where he is now. Hopefully when he's older, he looks back on this and thinks, I can do anything.”
Related Institutes: Digestive Disease & Surgery Institute , Ob/Gyn & Women's Health Institute, Cleveland Clinic Children's

