
To hear her husband, Gerald, tell it, Sarah Keil loves her job. But the 43-year-old Berea, Ohio, resident doesn’t remember working at a bank. Nor is Sarah aware of the specific duties or even the title of the job she’s currently on leave from.
In fact, Sarah has little memory of the 18 months or so before she contracted a severe case of COVID-19 in June 2021. The disease left her on the precipice of death on more than one occasion over the ensuing two months she spent at the hospital. She spent weeks on a ventilator at Fairview Hospital, weeks more at a critical illness recovery hospital and extensive time in rehab at Cleveland Clinic Rehabilitation Hospital in Avon, Ohio.
“I don’t leave the house much,” admits Sarah. “I’m kind of scared to, because I have a lot of anxiety. I can’t be around big groups of people because I’m scared to death of getting COVID again.”
Sarah had considered getting one of the COVID-19 vaccines earlier in 2021, but hesitated because she has a mild form of multiple sclerosis (MS), an autoimmune disease. While the Centers for Disease Control and Prevention and the National Multiple Sclerosis Society issued guidance recommending MS patients get vaccinated, Sarah was concerned there could be side effects.

When Sarah's oxygen levels and ability to breathe started declining, caregivers put her on a ventilator. (Courtesy: Sarah Keil)
“I didn’t get vaccinated because I was worried about what kind of neurological side effects I could get because of my MS,” she explains. “I wanted to research more into the shot before getting it. I have a lot of regret, not only for myself but for everything I put my family through.”
In late May, when Sarah started experiencing flu-like symptoms (body aches, dry cough, fever and difficulty breathing), she wasn’t surprised when test results revealed she had COVID-19. Her 20-year-old daughter, Alexzandrea, who worked in healthcare at the time, had already had a mild form of the virus.
“I figured I’m just going to stay quarantined, and hopefully, I’ll get through this, like my daughter did,” she recalls. “But that’s not what happened.”
Days later, her labored breathing continued to worsen so Gerald took her to the hospital, where she received a steroid shot and went home. However, her condition deteriorated. On June 9, Sarah went to the emergency department at Fairview Hospital. She didn’t make it back home for nearly two months.
Shortly after being admitted, Sarah was transferred to the intensive care unit (ICU), where her care was overseen by critical care intensivists who have become all-too familiar with COVID-19.
They followed the Cleveland Clinic treatment protocol for patients with severe COVID-19, including rounds of medications found to be effective in serious cases. But Sarah’s oxygen levels and ability to breathe plummeted. Soon, she underwent a tracheostomy where caregivers inserted a breathing tube into her neck. She was placed on a ventilator and heavily sedated to allow her struggling body to rest.
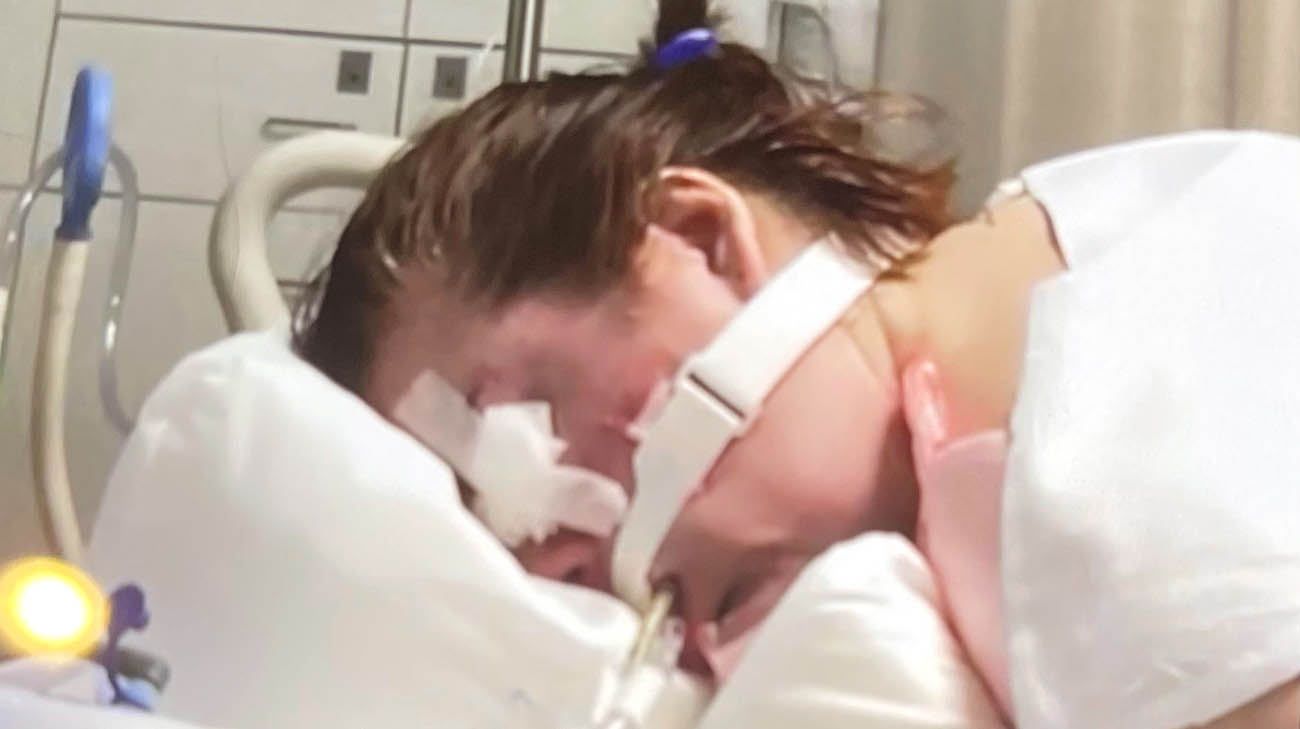
Sarah's treatments included medications and 16 hours daily of proning, a technique in which the patient is turned onto his or her stomach to keep fluid from collecting in the lungs (Courtesy: Sarah Keil)
According to Narendrakumar Alappan, MD, a critical care specialist and director of the Fairview Hospital ICU, Sarah’s rapid decline – despite constant medical intervention – is unfortunately not unusual for many unvaccinated COVID-19 patients.
“She was very sick with the most severe form of COVID infection that one could suffer from,” observes Dr. Alappan. “We know fully vaccinated people with a vaccine breakthrough infection are less likely to develop serious illness than those who are unvaccinated and get COVID-19.”
While Sarah remembers little of her time in the ICU, she learned later from her husband that medical staff called him on two occasions, requesting he come to her bedside because they feared she was at end of life.
Fortunately, her treatments – including medications and 16 hours daily of proning, a technique in which the patient is turned onto his or her stomach to keep fluid from collecting in the lungs -- slowly took effect.
“There were a lot of times where I didn’t think I was going to make it,” says Sarah.
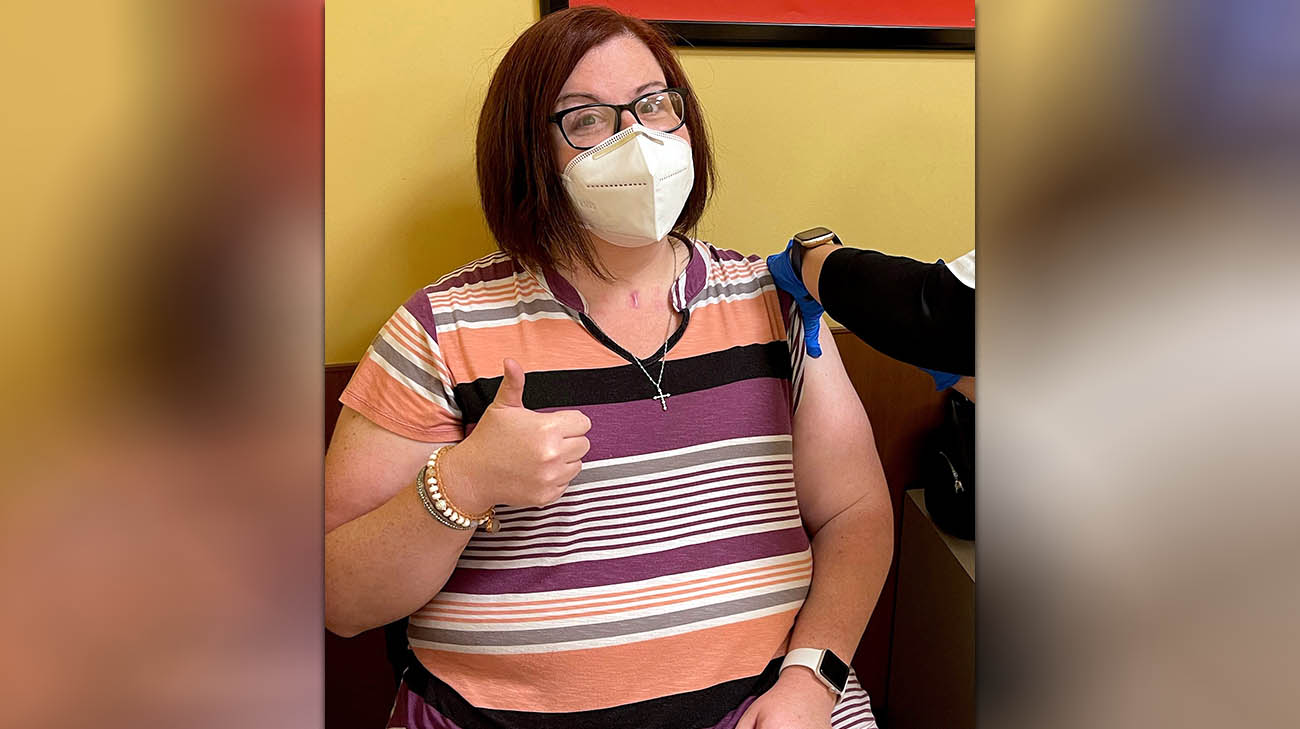
Sarah has received her first and second doses of the COVID-19 vaccine. (Courtesy: Sarah Keil)
Finally, after time in the critical illness recovery hospital, Sarah was transferred to the rehab hospital in Avon, Ohio, on July 23. Ultimately, she was removed from the ventilator and given a voice box to communicate until she could regain her ability to talk. Motivated to get home, she worked diligently and relearned how to walk and eat on her own. She went home on August 4 and has continued rehabilitation.
Sarah has also gotten the first and second doses of her COVID-19 vaccine regimen. Her family members have now been vaccinated, too.
“Don’t be like me,” she implores. “I encourage people to go get the vaccine. The little side effects, if you do get them, are far less than what you go through with COVID. I want people to know how important it is to get vaccinated. Protect yourself and protect others.”
Related Institutes: Respiratory Institute, Neurological Institute

