
Heart surgery saved Victor Young’s life in August 2019. The 64-year-old Cleveland Heights, Ohio, resident is convinced it saved him once again, in the spring of 2020, when he became among the first Ohio residents to contract the novel coronavirus.
“I have a theory. I actually think the heart surgery saved me,” says Victor, who contracted the disease from his wife, Marguerite. “It’s the only reason I made it through COVID.”
Eric Roselli, MD, the Cleveland Clinic heart surgeon who replaced Victor’s bicuspid aortic valve and aortic root via open-heart surgery in August 2019, believes his patient may be right.
“If Victor had gotten COVID without having his heart issues addressed, he might not have recovered,” notes Dr. Roselli. “Even though the way COVID affected him was primarily a pulmonary issue, I don’t think -- with the shape his heart was in before his surgery – he would have been able to tolerate it.”
Victor still had an uphill battle. During the early days of the pandemic, he had a high fever, difficulty breathing and viral pneumonia. Victor was the first patient admitted to Cleveland Clinic’s COVID-19 intensive care unit (ICU), which was established at Marymount Hospital.
As he called 911 that morning, barely able to breathe, he told his wife (who was dealing with a milder case of COVID-19 at the time) he was going to the hospital. “It was the last time I saw her until I was discharged more than three weeks later,” Victor recalls.
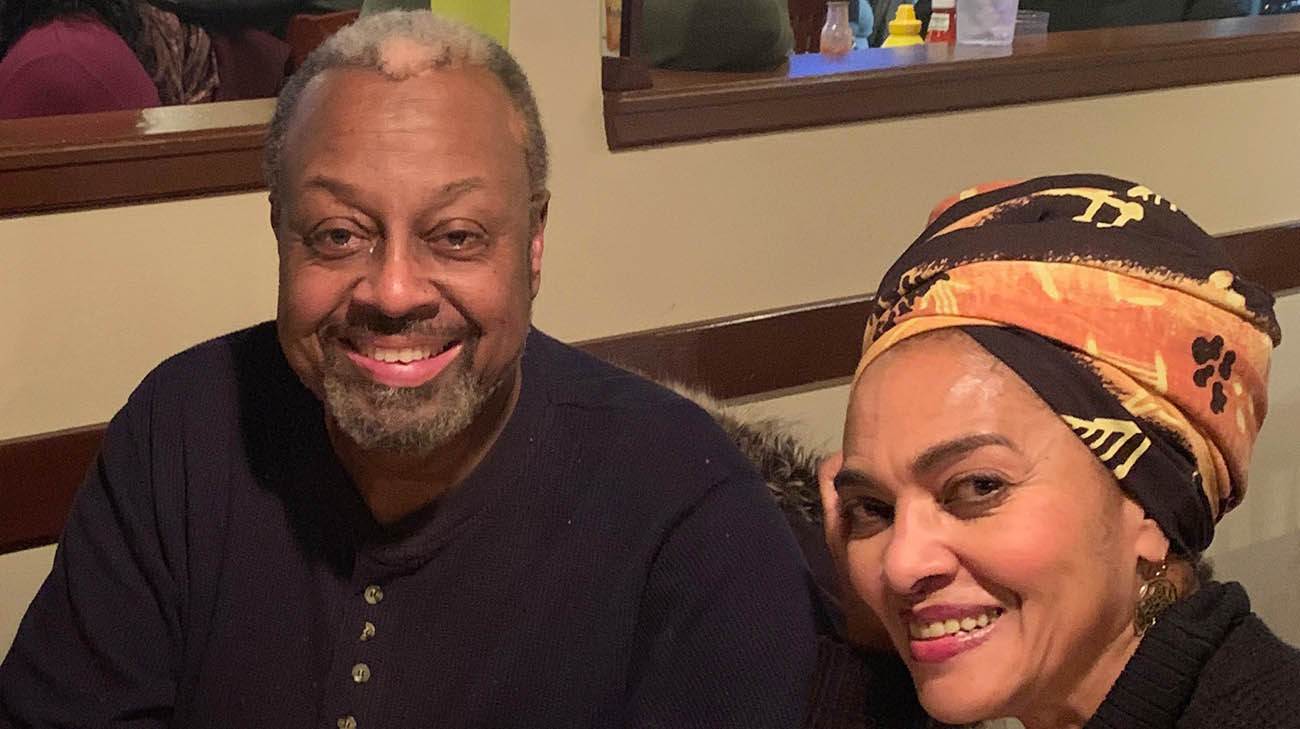
Victor and his wife, Marguerite, after Victor underwent heart surgery. (Courtesy: Victor Young)
Pulmonologist and critical care specialist Debasis Sahoo, MD, remembers the team still making protocols at that time, while trying to find the right course of treatment for Victor, especially since he and other physicians were only beginning to understand the nuances of the confounding disease.
“He was quite sick,” Dr. Sahoo states. “We started him on high-flow oxygen and began treating him with an immunosuppressive drug. But unfortunately, within two days, his breathing got worse and we had to put him on mechanical ventilation.”
Victor spent 10 days on a ventilator. Despite being heavily sedated, he has a few clear memories of that time. “I remember awakening in the ICU, and I could hear (nurses) talking about me being in a coma. I opened my eyes wide, and (a nurse) looked at me and said, ‘I don’t think he’s in a coma.’”
Still, sleep was a sanctuary for Victor during this trying time. Weak and disoriented, and with his mouth propped open to accommodate the breathing apparatus and tube extending into his lungs, Victor could do nothing. “I could hear, but I couldn’t talk. Ten minutes felt like an hour,” he says. “It was a weird and very difficult time. Like being trapped in your own body.”
In an attempt to take pressure off his struggling lungs, the Marymount team used a technique called “proning” on Victor. As Dr. Sahoo explains, it involves carefully flipping the patient from his back to his stomach, and leaving him in that position for as many as 16 hours at a time.
“It takes a team of five to seven nurses, a therapist and a physician to prone a patient,” says Dr. Sahoo, who notes the process can be quite intricate to ensure the breathing and feeding lines attached to the patient aren’t dislodged. “It worked, and (Victor’s) oxygenation improved.”
Finally off the ventilator and moved out of the ICU, Victor remained hospitalized for several more days before embarking on a pulmonary rehabilitation program at home, since many of those facilities were forced to close during the pandemic.

After a resilient recovery, Victor has been able to resume his 10-mile bike rides. (Courtesy: Victor Young)
Initially, the expectation was Victor would require constant use of oxygen and need as much as a year to get his lungs – which were severely damaged – functioning at a level approaching normal. However, he beat the odds and was able to get off oxygen in just a few months. He also was able to return to work.
“You can’t quit,” says Victor, who has resumed the 10-mile bike rides he enjoyed before his medical problems emerged. “You have to do things one step, one day at a time. A lot of times, you don’t feel like it’s going to get better because the progress is so incremental. Without putting in the work, you won’t get better.”
Victor’s tenacity and strong will to live were apparent to Dr. Roselli in late 2019, during the time Victor recovered from his open-heart surgery to rectify two congenital heart defects. “Open-heart surgery is a big deal,” says Dr. Roselli. “Having seen how well he did with that, I’m not surprised he’s been able to recover from a potentially even bigger problem, just a few months later.”
Victor credits his faith, the enduring support of his wife, family and friends and his dedicated Cleveland Clinic caregivers for his speedy recovery. “The care I received was exceptional, both medically and on a human level. My journey from March to where I am now has been incredible.”
Related Institutes: Heart, Vascular & Thoracic Institute (Miller Family), Respiratory Institute

