VA-ECMO (veno-arterial extracorporeal membrane oxygenation) is a type of life support that takes over for your heart and lungs. It can help in certain cases when your heart suddenly can’t pump enough blood to meet your body’s needs. A machine adds oxygen to your blood and removes carbon dioxide. This lets your organs and tissues stay alive.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
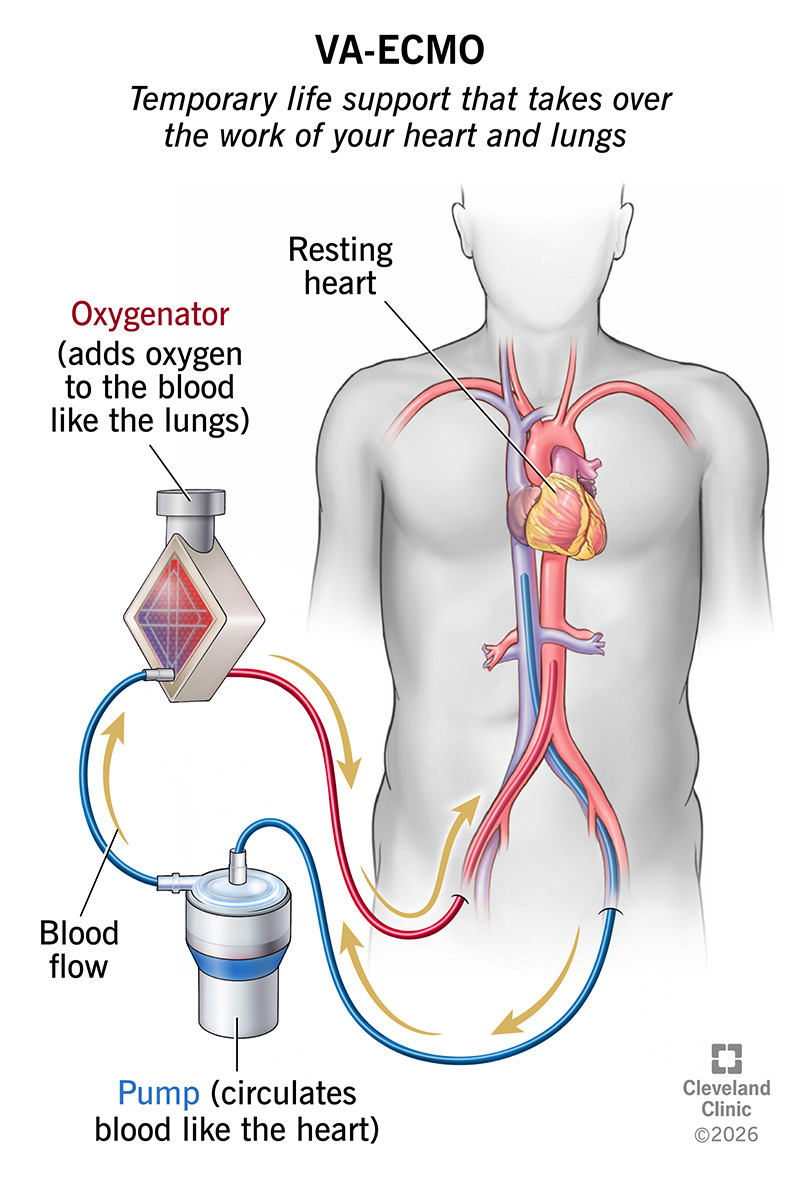
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/va-ecmo-illustration)
VA-ECMO (veno-arterial extracorporeal membrane oxygenation) is a type of temporary life support that takes over the work of your heart and lungs. Healthcare providers connect you to a machine that adds oxygen to your blood and removes carbon dioxide. The machine then sends the blood back into your body, where it flows to your organs and tissues, keeping you alive.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
On its own, VA-ECMO isn’t a treatment. But it can serve as a “bridge” until you receive treatment for:
VA-ECMO isn’t common. Providers only use it when your chance of recovery is good enough that the risks are worth it. Possible complications of VA-ECMO include:
Hospitals that offer ECMO have dedicated teams that assess each person’s case and decide if it’s an option for them.
To understand how VA-ECMO works, it helps to know what each part of the name means:
Advertisement
VA-ECMO provides both cardiac (heart) and respiratory (lung) support. The machine takes on the burden of your native heart and lungs, allowing them to rest and recover.
A team of highly trained healthcare professionals initiates and manages VA-ECMO. These teams typically include physicians, surgeons, nurses, respiratory therapists and other specialists.
Your care team connects you to an ECMO machine, which stays right next to your bed. You can think of the machine like an extension of your body. Tubes connect your body to the machine. Your team will also connect you to other monitors that track your vital signs and show how your body is responding to treatment.
These are the basic steps for VA-ECMO:
You can typically stay on VA-ECMO for up to five to seven days. Meanwhile, you’ll receive medications to support your heart function. Your care team may begin weaning you off the machine when your heart and lungs are strong enough to take over again. Weaning means they gradually reduce blood flow from the machine. Your heart and lungs slowly return to their normal duties.
If weaning doesn’t go well, your care team will discuss possible next steps with you and/or your loved ones. These include:
It depends on the severity of the underlying condition and any organ damage that’s already occurred. Your care team will explain what to expect in your case.
Some research shows that about 4 in 10 people who receive VA-ECMO for cardiogenic shock survive and leave the hospital. Long-term survival and quality of life can vary widely.
Because VA-ECMO helps people who are already very ill, it’s hard to know what might happen. Care teams understand this difficult reality. They’ll do everything possible to support you and your loved ones.
Advertisement
VA-ECMO (veno-arterial extracorporeal membrane oxygenation) offers some hope to many people who have serious medical conditions. But it’s not a guarantee of survival, and it comes with risks. Lean on your care team for guidance. Let them know if you have any questions or need more information to help make decisions.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Whether you need stitches, a broken bone set or think your appendix might be causing your abdominal pain, Cleveland Clinic’s emergency medicine team is here to help.
