A baclofen pump is a device that delivers baclofen, a muscle relaxant medicine, to the fluid in your spinal canal. It manages severe spasticity from various brain and spinal cord conditions. A surgeon will implant the pump and a catheter into your body to administer the liquid medication directly into your spinal canal.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
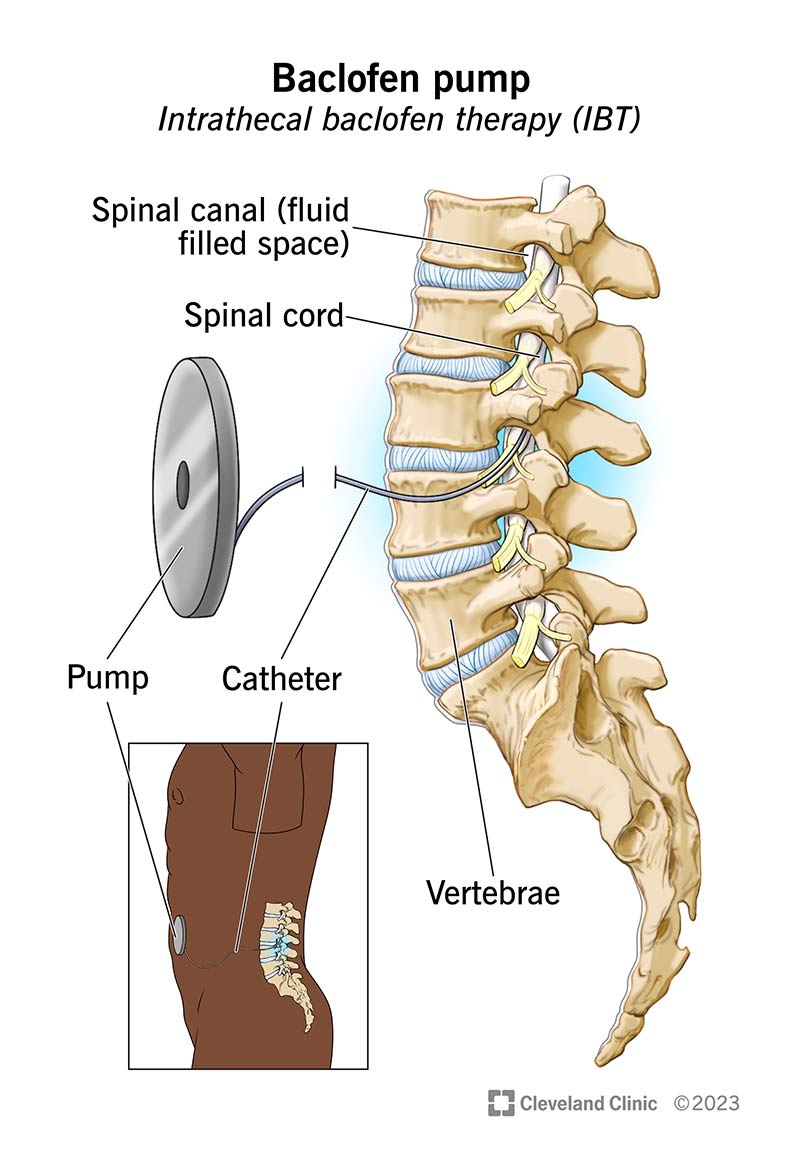
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/8997-intrathecal-baclofen-pump)
A baclofen pump is a surgically implanted device that continuously delivers baclofen, a medication, to your spinal canal. Your spinal canal is a fluid-filled space between your spinal cord and vertebrae.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The baclofen pump consists of a pump and a catheter. The catheter is a thin, flexible tube that brings the medication from the pump to the fluid in your spinal canal.
The pump is a round metallic disc (about 1 inch wide and 3 inches in diameter). A surgeon will perform a procedure to implant this device under the skin of your abdomen.
The pump contains a battery, a reservoir for the medication and a microprocessor. Your healthcare provider will program the pump with a small computer that communicates with the pump via a wand placed over the device in your skin. The programming tells the pump to give you medication on schedule. Your provider will also refill the medication periodically in the reservoir by inserting a needle into the pump and injecting medication into it.
You may hear your healthcare provider refer to a baclofen pump as intrathecal baclofen therapy (ITB).
Baclofen is a skeletal muscle relaxant medication. It’s a common medication to treat spasticity (muscle stiffness) and other spinal cord conditions. Within your spinal cord, baclofen:
A baclofen pump can help you manage spasticity caused by many conditions affecting the brain or spinal cord, like
Advertisement
The baclofen pump isn’t the most commonly used treatment for spasticity. One study found that healthcare providers prescribe a baclofen pump to just over 1,480 children (under age 18) and more than 7,080 adults (ages 18 to 64) annually in the United States.
A healthcare provider might recommend a baclofen pump if you have severe spasticity and oral medications aren’t helpful. They may refer you for a consultation to evaluate if a baclofen pump could be a good option.
The evaluation consists of a test injection of baclofen into your spinal canal. Your provider will perform a spinal tap and inject a small dose of baclofen into your spinal fluid during the test. Your care team will evaluate the effects of the injection after a few hours. The effects of the medication are temporary but provide very useful information that helps with the decision process.
Baclofen pump surgery is a procedure to permanently implant a device into your body so it can administer baclofen medicine into the fluid in your spinal column. A neurosurgeon or a pain management physician performs this procedure.
On the day of surgery, you’ll receive general anesthesia. This puts you to sleep so you won’t feel pain. Your surgeon will:
The surgery can take up to two hours.
After the surgery, you’ll stay in the hospital for a short time. In some cases, your surgeon will recommend inpatient rehabilitation to help you adjust to the pump before returning home.
The most common placement for a baclofen pump is underneath the skin in your abdomen beside your belly button. Your surgeon will determine the best placement for your pump based on your age, body composition and general health.
Your provider will educate you on the device so you’re informed about how it works and what you need to do to maintain it.
The pump needs to be refilled at regular intervals (usually every one to six months) by a trained provider. They’ll refill the pump by inserting a needle through your skin into a refill port on the pump. In some cases, refills can be done at home, but follow-up visits with a provider are necessary one to two times per year to ensure that the therapy is working appropriately.
Advertisement
Your provider can adjust the dose of baclofen at any time during a visit. Missing a pump refill appointment may lead to baclofen withdrawal.
When the pump battery approaches the end of its life, the pump needs to be replaced (but not the catheter). When there’s a problem with the baclofen pump or the catheter, they may also need to be surgically replaced or repositioned.
Seek medical attention as soon as possible if you suspect the pump isn’t working as it should.
The benefits of a baclofen pump include:
The baclofen pump needs to be surgically implanted into your body under anesthesia. The following complications are possible after surgery:
The most common side effect of a baclofen pump is increased weakness. Weakness may improve by reducing the dose of baclofen from the pump.
Complications more specific to the pump and catheter are rare but could include:
Advertisement
Serious complications aren’t common but some can be life-threatening. In most cases, they’re reversible as long as a healthcare provider treats them quickly.
Baclofen withdrawal happens if you experience an interruption of the delivery of baclofen via the pump or catheter. You’ll also likely experience withdrawal symptoms if your baclofen pump runs out of baclofen. The following symptoms may be suggestive of baclofen withdrawal:
In some cases, baclofen withdrawal can be life-threatening. Talk to your healthcare provider about how to maintain your pump so you can prevent these side effects. Seek help from a healthcare provider immediately if you suspect you have baclofen withdrawal.
Baclofen overdose is a rare complication of the baclofen pump. Baclofen overdose generally happens close to a baclofen pump refill or change in programming. Symptoms of baclofen overdose can also happen when you have another acute medical condition. They include:
Advertisement
Baclofen overdose can also be life-threatening. You should seek medical attention as soon as possible if you suspect you have a baclofen overdose.
The average recovery time after baclofen pump surgery is six to eight weeks. Your surgeon will give you a more specific timeframe based on your situation.
After surgery, avoid strenuous physical activities until given the “all clear,” and get plenty of rest.
You may be asked to wear an abdominal binder for a few weeks after the surgery. You may need to stay a few days in the hospital after the implant procedure and participate in rehabilitation.
Yes. A surgeon will permanently implant a baclofen pump and catheter into your body. If necessary, your surgeon can remove the pump and catheter.
A baclofen pump battery usually lasts around six to seven years. The timeframe may vary. Your provider will get an estimated battery duration when reading the information from the pump.
You’ll need another surgery to replace the pump before the battery expires. This surgery is usually faster than the initial placement surgery, as the catheter is already in place, and in most cases, you’ll be able to go home the same day.
Contact your healthcare provider if you notice symptoms of an infection like:
Contact 911 or your local emergency services number right away if you experience symptoms suggestive of the following:
Because baclofen is an approved treatment by the U.S. Food & Drug Administration (FDA), health insurance usually covers this cost or a portion of it, including Medicare and Medicaid. However, as coverage varies greatly between individual insurance plans, check with your insurance provider to learn more.
The main difference between the two types of baclofen is how you take the medication. Oral baclofen is typically the initial form of treatment for mild to moderate forms of spasticity. You can take this medication by mouth several times per day.
A baclofen pump delivers a liquid form of baclofen directly into your spinal fluid, using a device implanted into your body. A baclofen pump is FDA-approved for the treatment of severe spasticity.
It can be frustrating to manage symptoms of spasticity, especially when oral medications fall short and don’t work well with your body’s needs. Your healthcare provider will determine with you if you’re a good candidate for a baclofen pump. Your care team will educate you on how it works and what you can do to take care of yourself. You’ll need regular follow-up visits with your provider to refill the pump and adjust the dosage, if necessary.
You likely have a lot of questions about whether this type of treatment is right for you. Don’t hesitate to let your provider know if you have any questions.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Comprehensive pain recovery treatment plans can help you manage your pain levels and symptoms more easily.
