PVOD (pulmonary veno-occlusive disease) is a rare lung disease. Scars in small pulmonary veins create blockages. This leads to high blood pressure in your pulmonary arteries. Heart failure is a complication. A lung transplant is the only treatment with a solid track record. Without a transplant, PVOD is often fatal.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
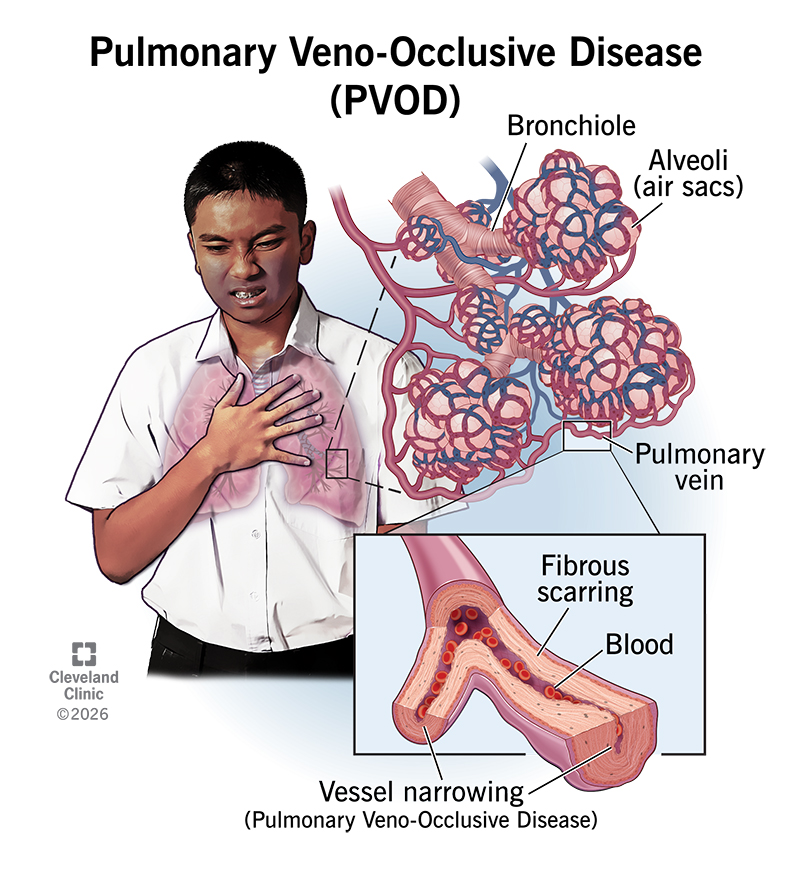
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/pvod.jpg)
PVOD (pulmonary veno-occlusive disease) is a rare disease that affects the blood vessels in your lungs. In PVOD, small veins in your lungs become scarred and narrowed, making it hard for blood to move through them.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Although it starts in your pulmonary veins, PVOD raises blood pressure in your pulmonary arteries. That’s why healthcare providers consider it a form of pulmonary arterial hypertension. PVOD causes shortness of breath and can lead to heart failure. Without a lung transplant, PVOD is often fatal.
PVOD affects 1 or 2 people in a million. Most people get a diagnosis as a child or young adult. But you can receive a diagnosis as late as your 60s. People who get PVOD from a genetic variation tend to be at the younger end. Those who don’t have a genetic variation are more likely to be male.
PVOD symptoms can include shortness of breath that can happen when you exert yourself or even when you’re lying down. Over time, this gets worse. You can also have weakness, low oxygen levels or a heart murmur. Symptoms include:
PVOD can come from genetic variants, certain disorders or medical treatments. You can also get it from exposure to certain substances. PVOD has a link to the following possible causes:
Advertisement
PVOD complications may include:
A biopsy is the gold standard for making a diagnosis, but a lung biopsy can also put you at a higher risk of dangerous bleeding. For this reason, healthcare providers often prefer other tests, like imaging, which can show the effects of blood vessel blockages.
Tests may include:
A lung transplant (for both lungs) is the only known treatment for PVOD. It can even cure it. Although your healthcare team can’t control when or if a lung is available, they can be there to support you. They can offer other treatments that may help you feel better while you wait for a lung transplant. Treatments you receive may include:
You should contact a provider if you have the following symptoms:
Questions to ask your provider may include:
Because the gold standard test can be too risky to perform, it can be difficult to diagnose this condition. This means the disease can become more advanced by the time you get a diagnosis.
PVOD has a poor prognosis. The condition can continue to get worse, even with treatment. Without a lung transplant, most people live two years or less after they start having symptoms.
But after you get a lung transplant, it’s very rare for PVOD to happen again.
It can be very hard to accept a diagnosis that has a poor outlook. But you aren’t in this alone. Seeking healthcare providers who have experience with PVOD (pulmonary veno-occlusive disease) can give you peace of mind. It can also be helpful to talk about your feelings with a counselor or support group.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When your heart needs some help, the cardiology experts at Cleveland Clinic are here for you. We diagnose and treat the full spectrum of cardiovascular diseases.
