Cold urticaria is a rare condition that causes an allergic reaction to cold temperatures. It usually triggers a rash or hives after exposure to cold air, water, food or drink. But symptoms can be more severe. The condition is sometimes associated with an underlying blood cancer or infectious disease.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
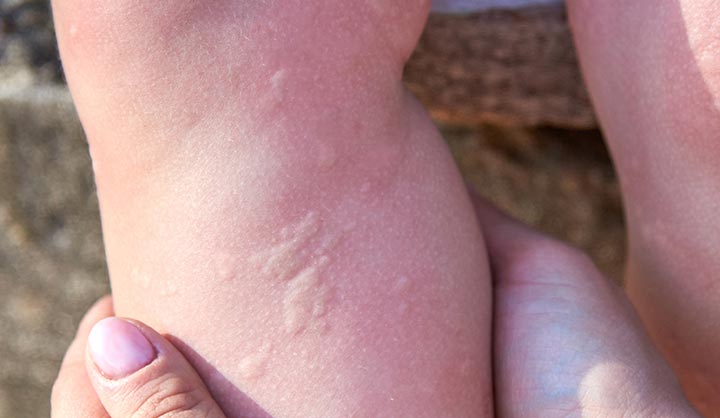
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/24629-cold-urticaria)
Cold urticaria is a condition that causes an allergic reaction to cold temperatures. A person with cold urticaria may develop a rash or hives after:
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Severe reactions may involve more serious symptoms.
There are two types of cold urticaria:
Cold urticaria can affect anyone. Although the disorder is sometimes inherited, most cases occur in people with no family history of the disease.
It’s sometimes associated with other health conditions, such as:
Cold urticaria is a rare disorder. The familial form is especially rare.
Advertisement
Cold urticaria occurs when the body releases histamines in reaction to cold. Histamines are chemicals made by your immune system in response to an allergen. But the reason for the histamine release is unknown.
Some cases of cold urticaria may be a symptom of autoimmune disorders. Autoimmune disorders involve your body’s immune system attacking healthy cells or tissue for unknown reasons.
The signs and symptoms of cold urticaria vary from person to person. They can be mild to severe. They may affect a small area of your skin or your entire body.
The main symptom is a skin rash after exposure to something cold. The rash generally occurs after the exposure is over, as your skin’s temperature rises.
The rash may involve:
Other symptoms might include:
In very rare, severe cases, a person may also experience a systemic reaction that affects their entire body, such as:
Cold urticaria isn’t contagious. But the condition is sometimes associated with viral or other infections, which can spread from person to person.
A healthcare professional can usually diagnose the condition with a quick cold urticaria test. The provider places an ice cube on your skin (such as your arm) for a few minutes, then removes it. If you develop a hive or rash several minutes later, that’s considered a positive test.
However, diagnosing familial urticaria may require exposure to cold air for a longer period of time.
Your healthcare provider also might recommend blood tests to identify any underlying disease or infection.
One of the most effective ways to manage cold urticaria is to avoid cold. Other common treatment strategies include:
Advertisement
Additional options include omalizumab injection and antibiotics.
If cold urticaria is associated with another disease or infection, your healthcare provider will also treat that accordingly.
An episode of cold urticaria can last a few minutes to several hours. The symptoms usually go away on their own after you’ve recovered from cold exposure. But sometimes an episode requires treatment to go away.
The long-term prognosis with cold urticaria varies widely. Sometimes, the condition stops occurring in a few years, but it can last a lifetime. Many people manage the condition well by making lifestyle changes.
Cold urticaria often recurs (happens again) after successful treatment of an episode.
Because scientists don’t fully understand the causes of urticaria, there aren’t any proven strategies to prevent it.
If you have the condition, you can prevent reactions and episodes by avoiding cold temperatures, including cold food and drinks.
Your healthcare provider will educate you about ways to protect yourself. Strategies include:
Advertisement
Cold urticaria is a condition that causes an allergic reaction to cold temperatures. If you get a rash after exposure to something cold, talk to your healthcare provider. They can help you protect yourself and offer possible treatments.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s primary care providers offer lifelong medical care. From sinus infections and high blood pressure to preventive screening, we’re here for you.
