Tympanosclerosis is scarring of your eardrum. It can happen after an injury or surgery on your eardrum. Some people never develop symptoms. In some cases, it can result in hearing loss. Treatments include hearing aids or surgery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
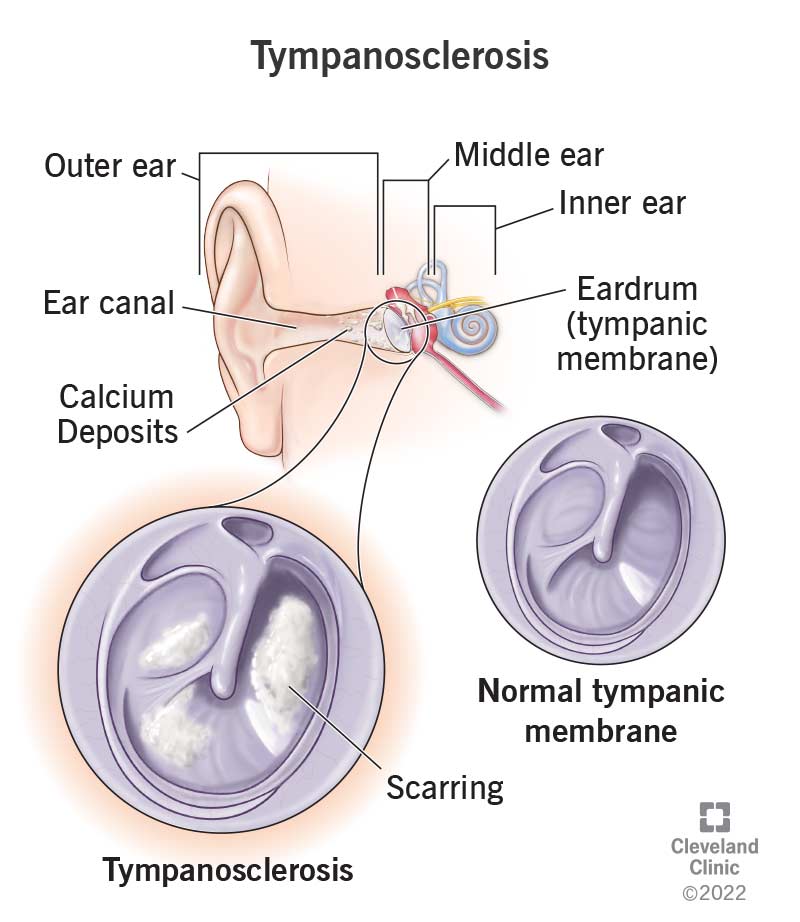
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/24265-tympanosclerosis)
“Tympanosclerosis” is the medical term for scarring of your eardrum (tympanic membrane). Your eardrum is a thin, translucent membrane that separates your outer ear from your middle ear. When your eardrum becomes damaged — by either injury or surgery — calcium deposits can cause your eardrum to harden, thicken and become rigid. Scarring on your eardrum looks like bright, chalky white lesions (spots).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Healthcare providers may refer to the condition as tympanosclerosis or myringosclerosis. These conditions are very similar. Both refer to calcium deposits affecting your eardrum. The only difference is that people with tympanosclerosis have calcium deposits on their middle ear structures in addition to their eardrum.
Anyone can get tympanosclerosis. But it’s more likely to develop in people with a history of ear injuries or infections.
In mild cases, tympanosclerosis may not cause significant side effects. If the scar tissue in your eardrum doesn’t affect your hearing, you won’t need treatment.
As mentioned, it’s possible for people with severe scarring to develop hearing loss in their affected ear(s). Depending on your situation, surgery can often improve or totally reverse tympanosclerosis-related hearing loss.
Yes. Many people with tympanosclerosis develop hearing loss as a result of tympanosclerosis. Hearing loss may be mild, moderate or severe. Surgery can repair scar tissue in your eardrum and, in many cases, restore hearing.
Tympanosclerosis symptoms and signs may include:
Advertisement
If scarring only affects your eardrum (and not your middle ear structures), you may not develop pain or hearing loss.
While tympanosclerosis is a common ear condition, healthcare providers don’t fully understand why it happens. Many experts believe it’s related to an abnormal healing response.
Health conditions that might contribute to the development of tympanosclerosis include:
No. You can’t pass tympanosclerosis to another person. But it’s possible to transmit infections that cause tympanosclerosis. To reduce your risk of infections, wash your hands frequently and don’t share personal items with someone who is sick.
If your healthcare provider suspects tympanosclerosis, they’ll refer you to an otolaryngologist (ENT) for further evaluation and testing. (An otolaryngologist is a doctor who specializes in diagnosing and treating conditions of the ear, nose and throat.)
An otolaryngologist will ask about your symptoms and review your medical history in detail. Next, they’ll look inside your ears with an otoscope (a tool that uses light and magnification to show detail). In some cases, they might need to use an endoscope to look inside your ear. (An endoscope is a flexible tube with a light and tiny camera attached.) They’ll also perform hearing tests to check for hearing loss.
Once you develop tympanosclerosis, the scar tissue doesn’t just go away. But unless you have hearing loss, you probably don’t need to do anything at all.
However, people with hearing loss due to tympanosclerosis usually need treatment. Depending on your situation, tympanosclerosis treatment may include surgery or hearing aids.
Surgery to repair your damaged eardrum is the most common tympanosclerosis treatment. Some people need myringoplasty, which repairs a ruptured eardrum. Others will need tympanoplasty, which repairs their eardrum and any damaged middle ear bones.
During tympanoplasty, a surgeon will remove scarred or hardened portions of your eardrum. If your middle ear bones (ossicles) have sustained damage, your surgeon will repair those as well. They’ll use a graft made of your own cartilage or a synthetic material to patch any holes. Finally, they’ll pack your ear canal with cotton and place a bandage on the outside of your ear.
If surgical tympanosclerosis treatment doesn’t fully restore hearing, then hearing aids can help. Ask your healthcare provider which type of hearing aid is right for you.
In most cases, people recover from surgical tympanosclerosis treatment in about one to two weeks. If you have a physically demanding job — such as one that requires a lot of heavy lifting — you may need to wait a week or two longer before returning to work. Ask your healthcare provider when it’s safe to resume normal activities.
Advertisement
Scar tissue on your eardrum doesn’t go away on its own. People with tympanosclerosis-related hearing loss may need surgery to correct the issue.
It’s important to note that just because your eardrum has scarring, it doesn’t mean you’ll definitely have hearing loss.
Generally, the only way to reverse tympanosclerosis is with surgery. If you’ve developed hearing loss as a result of eardrum scarring, then your healthcare provider will talk with you about your options.
You can’t prevent tympanosclerosis altogether. But you may be able to reduce your risk by following these guidelines:
If you develop hearing loss, ear pain or other related symptoms, schedule an appointment with a healthcare provider. They can determine the cause of your symptoms and help you find appropriate treatment.
If you or your child has tympanosclerosis, here are some questions you may want to ask a healthcare provider:
Advertisement
When your eardrum or middle ear structures develop scar tissue, it’s called tympanosclerosis. People with this condition don’t always have symptoms, but hearing loss and ear pain are possible warning signs. Surgery is usually the recommended treatment for tympanosclerosis-related hearing loss. If surgery doesn’t fully restore hearing, then hearing aids can help. If you’ve developed hearing loss or other related symptoms, visit your healthcare provider. Prompt diagnosis and treatment can get you on track to healing and a better quality of life.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
If you have conditions affecting your ears, nose and throat, you want experts you can trust. Cleveland Clinic’s otolaryngology specialists can help.
