A septate uterus is when your uterus is divided into two parts by a membrane called the septum. It’s a condition present at birth that can only be corrected with surgery. A septate uterus can cause pregnancy complications like miscarriage.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
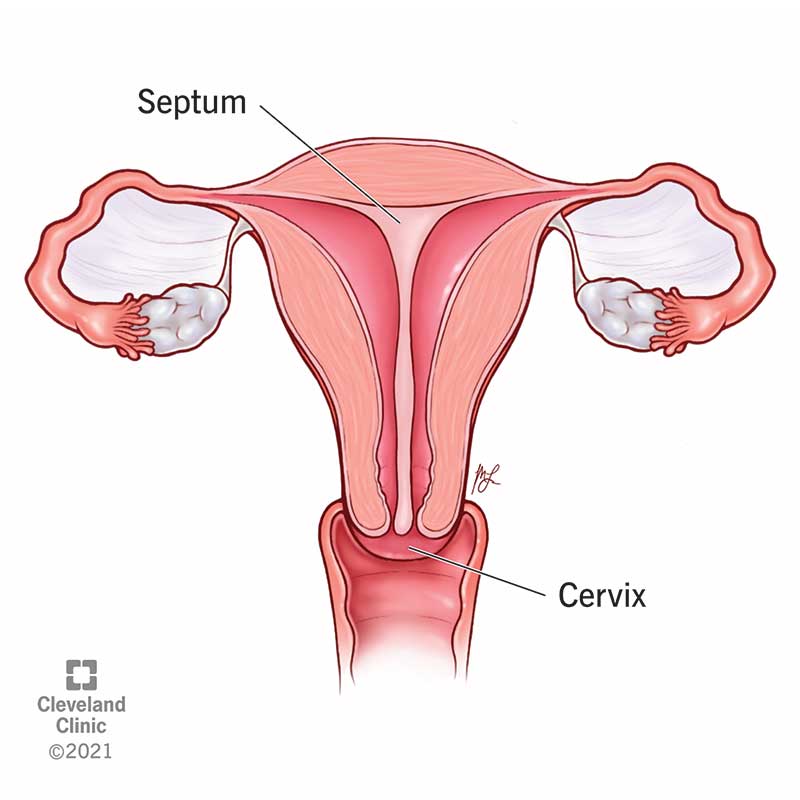
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22809-septate-uterus)
A septate uterus is when your uterus is divided into two parts by a membrane called a septum. A typical uterus is one hollow or open space. With a septate uterus, your uterus has two smaller spaces instead of one. The septum acts as a wall or barrier. This condition is sometimes called a uterine septum.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
You may not know you have this type of uterus until you’re pregnant or trying to get pregnant. If you have a septate uterus, it’s still possible to have a healthy pregnancy and delivery.
A septate uterus is rare, but it’s one of the more common uterine abnormalities. Uterine septum affects about 1.5 in 100 women.
You usually don’t have symptoms of a septate uterus. Your healthcare provider sometimes finds it while they’re investigating the cause of repeat miscarriage or infertility.
A septate uterus is congenital (something you’re born with). It happens during fetal development. Instead of forming one open uterus, a tissue wall (called a septum) stays in the middle, dividing the uterus into two parts. A septum can vary in size and length.
There’s nothing you can do to prevent having a septate uterus. And there isn’t any evidence that a septate uterus is genetic.
A septate uterus shouldn’t affect your period.
A septate uterus usually doesn’t cause health problems. During pregnancy, it may lead to certain risks, like:
You may also be at a higher risk for endometriosis.
Advertisement
A healthcare provider will usually start with a pelvic exam. But unless the septum extends into your vagina, it won’t give them enough information. Instead, your provider will use imaging tests to clearly see the septum — its size, thickness and location.
Your healthcare provider may use any of the following:
After that, they may classify your septate uterus as:
Uterine septum doesn’t always need treatment. It depends on your symptoms, pregnancy history and plans for pregnancy.
Surgery is the only way to fix a septate uterus. The surgery involves removing the septum. Once this happens, your uterus is one open space (like a typical uterus).
A procedure called hysteroscopic metroplasty is the most common treatment. It’s an outpatient procedure that takes about an hour. You’re asleep for surgery under anesthesia. The steps are:
The risks associated with removing the septum include:
Yes, you can get pregnant after. One study found that 47% of women got pregnant within one year of surgery. Most healthcare providers will recommend at least two months to recover from surgery before trying to conceive.
No, a septate uterus can’t grow back.
If you’re pregnant and have a septate uterus, it’s important to contact your healthcare provider if you experience any of the following:
If you’re not pregnant, the chances of having health complications are rare. Talk to your healthcare provider about any signs or symptoms you should watch for.
If you have a septate uterus, it’s normal to have questions. Some questions you might ask your provider are:
Having a septate uterus may not affect your fertility or pregnancy. It depends on the size of the septum and how far it extends. Talk to your healthcare provider about the risks of becoming pregnant and if they recommend surgery to fix the septum.
Advertisement
If you have a septate uterus, your provider will want to monitor the fetus’s growth closely throughout your pregnancy.
Yes. You’re at higher risk for pregnancy complications, but most likely, your baby will be born healthy. Your pregnancy care provider will monitor your pregnancy and watch for any signs of problems.
Your baby is more likely to be in a breech position. This is because the fetus has less room to rotate into a head-down position. You’ll need a C-section if your baby is breech.
Hearing that you have an irregular uterus can be surprising. But it could also explain your symptoms, like infertility or recurring miscarriages. Discuss your chances for a successful pregnancy with your healthcare provider. They may recommend surgery to fix the septum. Most people with a septate uterus can have healthy pregnancies.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
From routine pelvic exams to high-risk pregnancies, Cleveland Clinic’s Ob/Gyns are here for you at any point in life.
