Angioedema is swelling in the tissue under your skin. It’s most common in your lips, eyelids, tongue, genitals, hands and feet. Causes include allergies, medication side effects, vibrations, inherited gene changes and some health conditions. Call 911 (or your local emergency services number) or go to the ER if you’re having trouble breathing or have a sudden drop in blood pressure.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
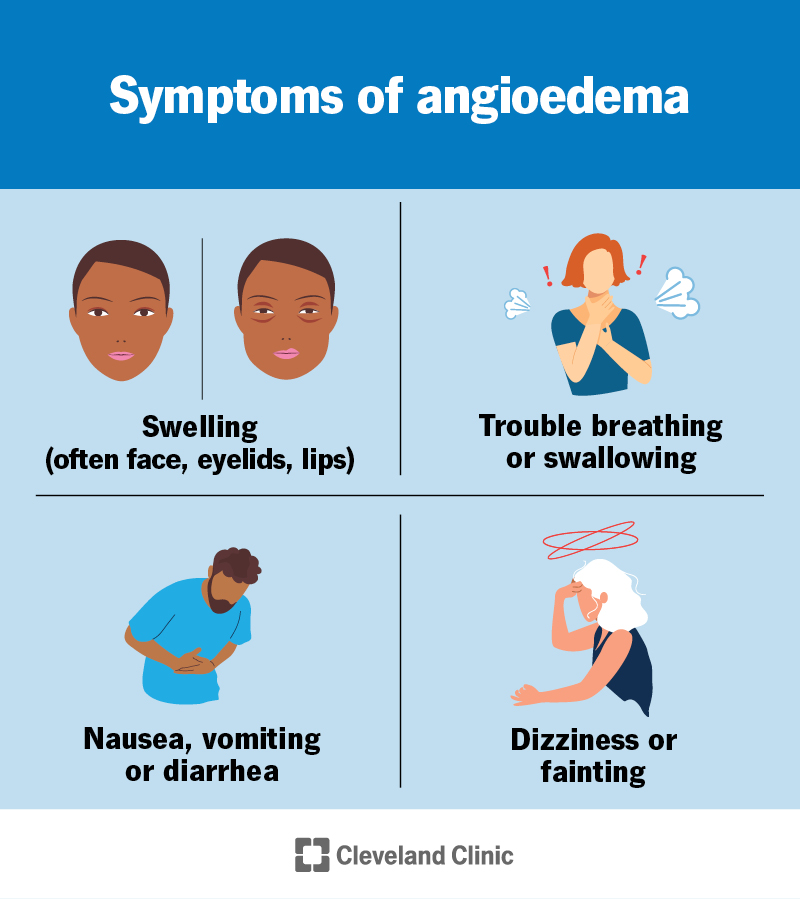
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/angioedema)
Angioedema is a reaction that causes swelling in the tissue below your skin. It most often affects your lips and eyelids. But it can affect any body part. It usually comes on quickly and lasts a few hours to a couple of days.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Swelling from angioedema can happen when your body reacts to something like food, medicine or even vibrations. Sometimes, it happens for no clear reason. It may be due to a health problem you were born with or another issue that makes the swelling come and go without warning. Your provider might consider other causes if the swelling lasts longer than two or three days.
Angioedema can be serious, even fatal, if your airways swell or your blood pressure drops too low. Call 911 (or your local emergency number) or get to an emergency room if you’re having trouble breathing or feeling weak or dizzy.
Angioedema causes swelling, most commonly in your:
Other symptoms include:
Hives often happen at the same time as angioedema. But you can have angioedema without hives.
It can be. Angioedema can sometimes cause severe airway swelling or a sudden drop in blood pressure. Call 911 (or your local emergency number) or get to an emergency room if you’re having trouble breathing or feeling weak or dizzy.
Angioedema happens when liquid from small blood vessels escapes and fills up tissues, causing swelling. It often happens in response to allergies, drug side effects or vibrations. Inherited gene changes, cancer, autoimmune diseases and infections can also cause it without a predictable trigger. Sometimes, it happens for no known reason (idiopathic angioedema).
Advertisement
Specific causes of angioedema include:
Sometimes. If you have idiopathic or hereditary angioedema, stress might make swelling more likely.
You’re at higher risk for angioedema if you:
Your healthcare provider will begin with a physical examination. They’ll ask you questions about:
Allergy skin tests and allergy blood tests can help determine if the swelling is an allergic reaction. If there’s no known trigger, genetic testing and other blood tests can help determine if another health condition is causing the swelling.
If you have allergic angioedema, you should avoid food, medications and other substances that cause swelling. Check with your provider before stopping prescription medications. If the swelling is a medication side effect, your provider will help you find a medication to replace the one that’s causing you to swell. They might also recommend applying ice or taking cool showers to reduce swelling.
Advertisement
Medications your provider might recommend to prevent or treat angioedema depend on the cause. They include:
Talk to a healthcare provider if you have repeated episodes of swelling, especially if you don’t know the cause. Call 911 (or your local emergency services number) or go to the ER if you or someone you’re with experiences:
Most of the time, angioedema is manageable by avoiding things that cause it or taking medications that help prevent it. But don’t stop taking medication prescribed by your doctor unless they say it’s OK. Your provider might also recommend keeping an epinephrine autoinjector or other emergency medications with you in case of unexpected swelling.
Advertisement
There are medications that can reduce your risk of swelling if you have HAE, acquired C1-inhibitor deficiency or chronic idiopathic angioedema. If you have allergy-related angioedema, you can prevent swelling by avoiding the food, medication or other triggers that cause allergic reactions. If you have non-allergic angioedema as a drug side effect, you’ll need to work with your healthcare provider to find another medication.
Whether it’s a known allergy or out of the blue, swelling in your body can be scary. Fortunately, most causes of angioedema are manageable. A healthcare provider can help you determine the cause and make recommendations to reduce your risk of swelling. They can also make a plan for what to do if you have an episode. Being prepared with this plan can be reassuring and help you feel empowered to manage any unexpected symptoms.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Allergies can wreak havoc on your life. At Cleveland Clinic, our team of experts can help create a treatment plan that’ll help you breathe easier.
