If you’re an athlete experiencing aching or sharp pain on the outside of your knee or hip, you might have a tight iliotibial band. Your iliotibial band is a tendon that can rub against your hip or knee bones. The swelling and irritation can cause several symptoms. You might need physical therapy, medications or, rarely, surgery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
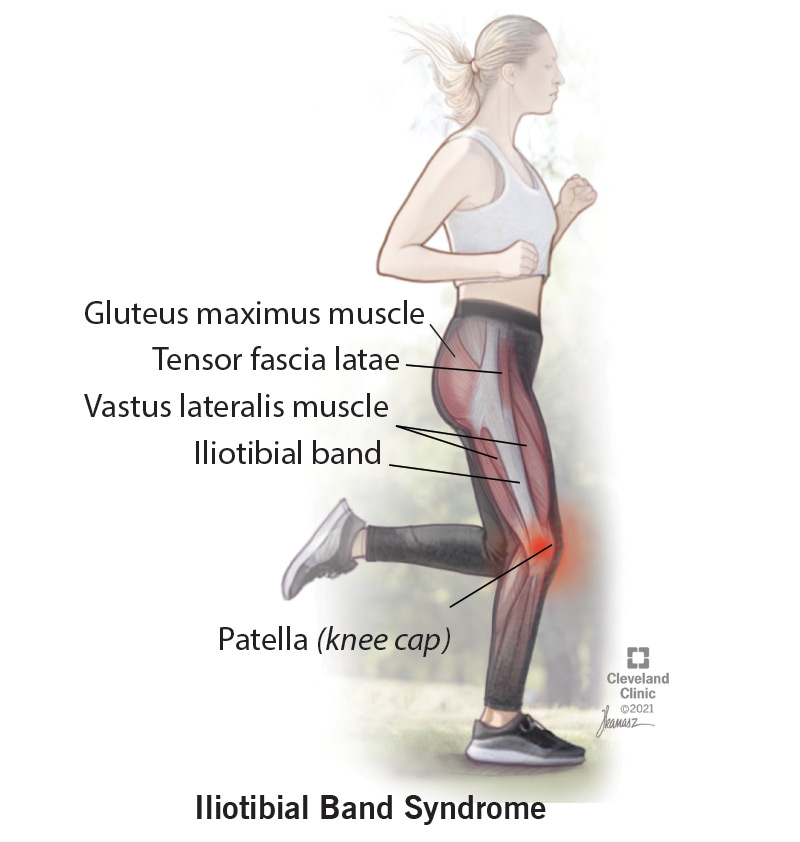
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/21967-Iliotibial-band-syndrome)
Iliotibial band syndrome is where a tendon called the iliotibial band gets irritated or swollen from rubbing against your hip or knee bones. The tendon is on the outside of your leg, and it goes from the top of your pelvic bone down to your knee. It rubs against your bones when it gets too tense (tight). There are many reasons why your iliotibial band might tighten.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Tendons are flexible, elastic-like fibrous tissues that connect your muscles to your bones. Your tendon pulls on the bone when you squeeze a muscle, and that makes your bone move.
You can have iliotibial band syndrome in one leg, or you can have it in both legs. When you have ITBS in both legs, it's called bilateral iliotibial band syndrome.
You’re at a higher risk for iliotibial band syndrome if you’re young and exercise frequently. Examples of athletes who are most prone to ITBS include:
Even if you're not an athlete, there are still some traits that give you a slightly above average chance of getting iliotibial band syndrome. Reasons include:
Experts note that iliotibial band syndrome often affects U.S. Marines during training. More than 20% get iliotibial band syndrome. Frequent runners, especially long-distance runners, are also prone. Iliotibial band syndrome accounts for about 12% of running injuries. More females than males have iliotibial band syndrome.
Advertisement
Knee pain — of which iliotibial band syndrome is one of many causes — affects as many as 25% of adults.
Your iliotibial band gets irritated and swollen when it’s stretched too tight and rubs against bone. Possible causes of a tight iliotibial band include:
Your tight iliotibial band might rub against your bones for reasons that include:
A tense iliotibial band can cause several symptoms:
At first, the pain will start after you exercise. As the syndrome worsens, you’ll feel it the whole time you exercise and, eventually, also when you’re resting.
People with iliotibial band syndrome describe the initial pain as aching and burning. The more they exercise their leg, and the worse the syndrome gets, the sharper the pain turns. Tell your healthcare provider not just where the iliotibial band syndrome pain is but what it feels like.
Advertisement
Your healthcare provider might diagnose you with iliotibial band syndrome after discussing your history of exercise and symptoms and performing a physical examination. Your provider should check for the following signs of ITBS:
Your healthcare provider might perform a test called the Noble and Ober test. There are several steps that include:
Correct diagnosis of iliotibial band syndrome also requires imaging tests, including:
Advertisement
Your healthcare provider will want to fully understand what you’re experiencing so that you receive the best care possible. Questions they might ask include:
There are some treatments for iliotibial band syndrome that you can do at home, while others require a healthcare provider. Common treatments include:
Advertisement
Your iliotibial band syndrome might heal after treatments such as rest, physical therapy and medications. The pain will likely increase if you don’t receive treatment. Discuss your options with your healthcare provider.
With treatment, specifically nonsurgical treatment, about 50 to 90% of people with ITBS improve after about four to eight weeks. Some studies show that it happens within two to six weeks.
Iliotibial band syndrome can worsen without treatment. Talk to your healthcare provider about psychical therapy, medications and other treatments.
Iliotibial band syndrome can sometimes cause patellofemoral pain syndrome (PFPS). You might feel pain around and under your kneecap (patella) in addition to the knee and hip pain. Be sure to let your healthcare provider know if you have more symptoms. There are treatments for PFPS.
Preventing iliotibial band syndrome might be difficult if you’re an athlete such as a skier, cyclist or long-distance runner. But you might try changing some of the ways you do those activities to reduce your risk of ITBS. Examples include:
Once you're pain-free, you can slowly get back to your regular activities with your healthcare provider's permission. Make a plan with your provider. Together you can figure out what activities you can do and when you can safely do them.
Contact your healthcare provider if you have knee or hip pain that either doesn't get better after a few weeks or gets even worse.
If you’re part of the 25% of adults who experience knee pain, you might have iliotibial band syndrome. When the tendon rubs against your hip or knee bones, it gets swollen and irritated, causing several symptoms. Athletes have an above-average chance at getting ITBS.
You might have to hop off your bike if you have iliotibial band syndrome. The pain might take you off the court, field or track. But, likely, you'll just have to take a break from your favorite sports, not give them up forever. ITBS is treatable. With your healthcare providers' help, you can recover from iliotibial band syndrome.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic experts are here to treat your tendinopathy (tendon pain) and get you back to doing the things you love.
