Ear eczema is a common skin condition that causes discoloration, dry skin and itchiness in, on and around your ears. It isn’t contagious, but you have a higher risk of developing it if you have a family history of eczema, asthma or allergies.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
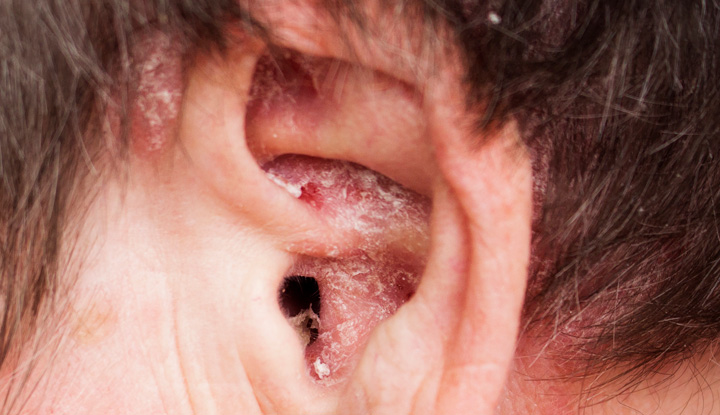
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/21842-ear-eczema-546460492)
Ear eczema (atopic dermatitis) is a condition that causes your skin to become dry, discolored, itchy and bumpy. It may appear on the outside of your ear or inside your ear canal.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Eczema damages the skin barrier function (the “glue” of your skin). As a result, your skin becomes more sensitive and more prone to infection and dryness.
Psoriasis and ear eczema are two different skin conditions. They differ in where the disease appears on your body, how much it itches and how it looks.
Psoriasis is a chronic skin disorder, which means it’s a skin condition that doesn’t go away. People with psoriasis have thick, discolored patches of skin (plaques) covered with white or silvery scales.
Ear eczema affects the skin in, on and around your ears. Eczema also causes more intense itching than psoriasis. Many people, especially children, can get both eczema and psoriasis.
Ear eczema can affect anyone with ears. However, it’s more common in people with:
Eczema is very common, and any part of your skin can develop it, including your ears. Approximately 15% to 30% of children have eczema, and 2% to 10% of adults have it.
Ear eczema affects your ears, including:
Advertisement
Your skin may itch, change color, develop bumps, dry out or thicken.
In severe cases of ear eczema, your skin may crack or leak (weep) a thick, yellow or white fluid (pus). You may also experience a ringing noise (tinnitus) or hearing loss if you have a severe case of ear eczema in your ear canals.
Symptoms of ear eczema include:
Ear eczema doesn’t hurt. However, if you scratch your ear eczema, you may break your skin, leading to an infection that can cause pain.
Eczema can develop anywhere on your skin, including your ears. Different types of eczema can develop in your ears, including:
Ear eczema isn’t contagious. You can’t spread ear eczema to another person through skin-to-skin contact.
Your healthcare provider will examine your ears. They’ll look for common signs of eczema, including discoloration and dryness. They may use a lighted instrument (otoscope) to look inside your ear. They’ll also ask about your symptoms.
Your healthcare provider can typically diagnose ear eczema after a physical exam. However, if there’s any doubt, they may perform the following tests:
To get rid of your ear eczema, it’s important to determine what’s causing it. Try to determine what triggers or worsens your ear eczema, and then avoid it. The goal is to reduce itching and discomfort and prevent infection and additional flare-ups.
The following home remedies may relieve your ear eczema:
Advertisement
Petroleum jelly (Vaseline™) or skin care ointments (Aquaphor™) can help treat your ear eczema. These products moisturize and protect your affected skin. They’re hypoallergenic and have antibacterial and antifungal characteristics that help heal your skin.
Gently wash your ears with warm running water and mild soap. Then, use a cotton swab to apply a small amount of petroleum jelly or skin care ointment over your ears. Try to avoid touching your ears to prevent dirt or bacteria from entering the area.
With proper treatment, your ear eczema should go away after one to three weeks. However, no treatment can claim to eliminate the symptoms of ear eczema 100% of the time. You may encounter flare-ups on or in your ears for the rest of your life. Once you determine the cause of your flare-ups, you may prevent flare-ups from happening as often.
If you have ear eczema, it can generally be well-managed with good skin care and treatment. However, flare-ups of symptoms can occur throughout your life.
Ear eczema is a chronic condition, which means there isn’t a cure. However, treatments are very effective in reducing the symptoms of dry, itchy skin.
There are steps you can take that may prevent ear eczema outbreaks:
Advertisement
Many people live with ear eczema. It can be challenging, though.
There may be times when your ear eczema disappears. These times are “remission” periods. The goal of a good skin care routine and treatment is to prevent flare-ups. Be sure to avoid anything that triggers your ear eczema, moisturize, take your medicine and follow your healthcare provider’s recommendations.
See your healthcare provider as soon as you notice symptoms. Get treatment right away.
Advertisement
Ear eczema is annoying and embarrassing, and it can be alarming if it impacts your hearing. It can affect your quality of life or make you feel self-conscious. However, it’s common and very normal. With a proper skin care routine and treatment, you can reduce its impact. See your healthcare provider as soon as you notice signs of ear eczema.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Every day, people see your skin, hair and nails. At Cleveland Clinic, our expert and caring dermatology team will make sure they’re healthy and strong.
