Cholestasis of pregnancy is a liver disease that can develop late in pregnancy. The main symptom of cholestasis is severe itching. It typically goes away after your baby is born.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
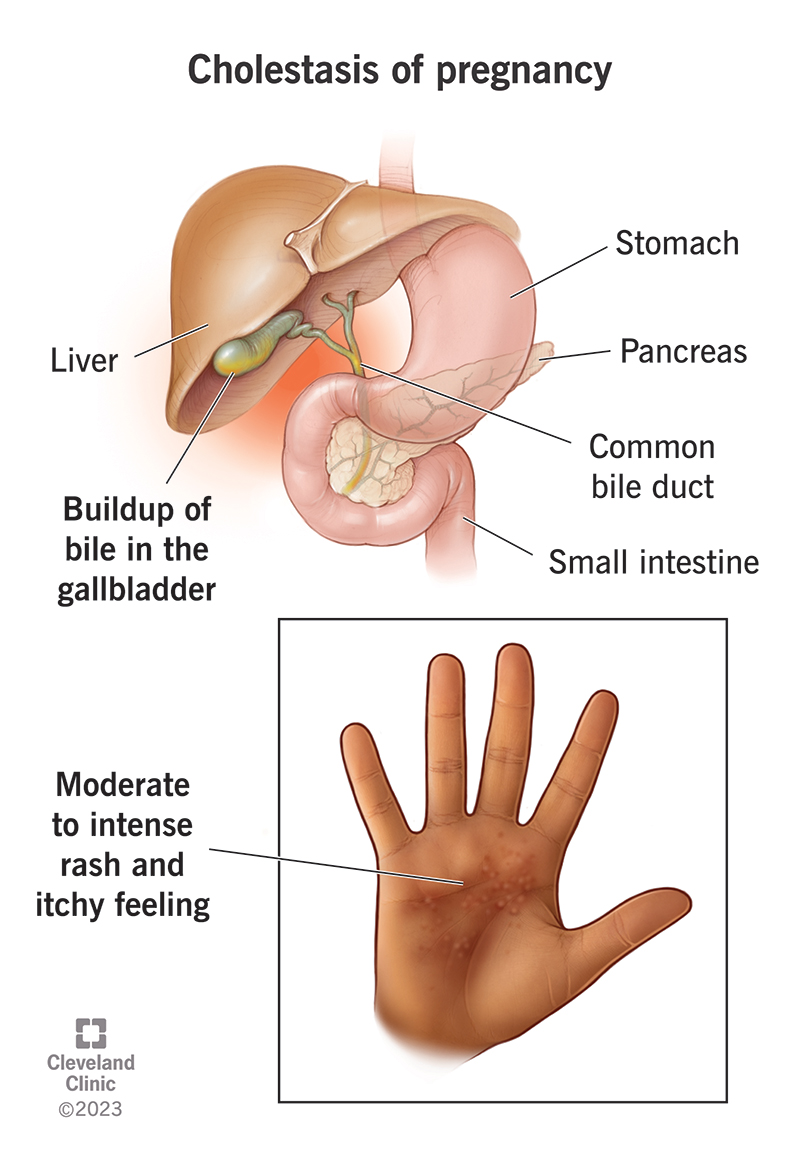
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17901-cholestasis-of-pregnancy)
Cholestasis of pregnancy is a liver condition that causes severe itching during pregnancy. It’s also known as intrahepatic cholestasis of pregnancy (ICP). It typically occurs after the 28th week of pregnancy, but it can start earlier.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
This condition affects how your liver works. It causes bile to build up in your body. Bile is a substance your liver makes to help digest fats. When bile levels get too high, it can cause severe itching.
If your liver isn’t working properly, bile can reach unsafe levels. This may increase the risk of pregnancy complications. Your pregnancy care provider will monitor you closely to help lower these risks.
Cholestasis affects about 1 to 2 in 1,000 pregnancies.
The main symptom is severe itching without a rash. It may start on your hands and feet and spread to other body parts. The itching is usually worse at night.
Less common signs of cholestasis may include:
Bile is a substance your liver makes to help digest fats. During pregnancy, high levels of estrogen and progesterone can affect how your liver moves bile. This means bile doesn’t flow through your body as well.
When bile doesn’t move properly, it builds up in your liver. It can then enter your bloodstream. Bile in your blood can make you feel very itchy.
Cholestasis of pregnancy typically develops in the third trimester, when pregnancy hormone levels are at their highest. It can also be genetic. This means you’re at a higher risk if your biological parents have cholestasis.
Advertisement
You’re at a higher risk for developing cholestasis of pregnancy if you:
You’re at risk for the following complications:
Other complications of cholestasis of pregnancy include:
Your pregnancy care provider may deliver your baby early to decrease the risk of these complications.
Your pregnancy care provider diagnoses cholestasis of pregnancy with a physical exam and blood tests. These tests show how your liver is working. They’ll also measure the level of bile acids in your blood using a serum bile acid test.
If you have this condition, you may need regular blood tests for the rest of your pregnancy. These tests help monitor bile levels in your blood.
Your provider may order other tests. A prothrombin time test checks how well your blood clots. An ultrasound can look at your bile ducts and liver.
Healthcare providers use a medication called ursodeoxycholic acid (UDCA, ursodiol or Actigall®) to treat cholestasis of pregnancy. This medicine helps your liver work better. It also lowers the amount of bile in your blood.
You can try these treatments to help with the itching, too:
If medication doesn’t lower bile levels, your provider may recommend delivering your baby early. It often happens around 37 or 38 weeks of pregnancy. An early delivery may reduce the risk of complications.
If your provider delivers your baby early, they’ll likely give you a steroid that helps mature your baby’s lungs and a vitamin K supplement to prevent severe bleeding.
Call your healthcare provider if you’re pregnant and have intense itching, light-colored poop and extreme fatigue. They may recommend you come in for an exam to check for cholestasis.
Cholestasis of pregnancy usually goes away a few days after your baby is born. Your hormone levels return to pre-pregnancy levels. Your liver can move bile the way it should. You can stop taking medication once your bile levels return to typical levels.
Advertisement
Most people don’t have any more liver problems after pregnancy. But this condition can come back in future pregnancies. One study showed your risk can range from 40% to 90%.
Having IPC doesn’t mean your baby will be unhealthy. Your pregnancy care provider will monitor you closely. They’ll use ultrasounds and blood tests to check your bile levels. These tests help your provider watch for signs of stress. They also help decide the safest time for delivery. The goal is to keep both of you healthy.
The itching cholestasis causes can be hard to ignore. It isn’t usually life-threatening and should go away after your baby is born. Your pregnancy care provider will monitor you closely to ensure there are no complications. Your provider may deliver your baby early if it’s the safest option.
Don’t be afraid to ask your provider questions about your diagnosis. They’re there to listen and reassure you that you and your baby will be OK.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Worried about your high-risk pregnancy? Want the best maternal and fetal health care? Look no further than Cleveland Clinic. We’re here for all your needs.
