Periodontitis is an oral health condition that causes sore, bleeding, swollen gums. Left untreated, periodontitis can lead to tooth loss, bone loss, bad breath and other oral health problems. You can manage mild periodontitis with a deep dental cleaning. More severe cases require surgery. Your outlook is good with treatment.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
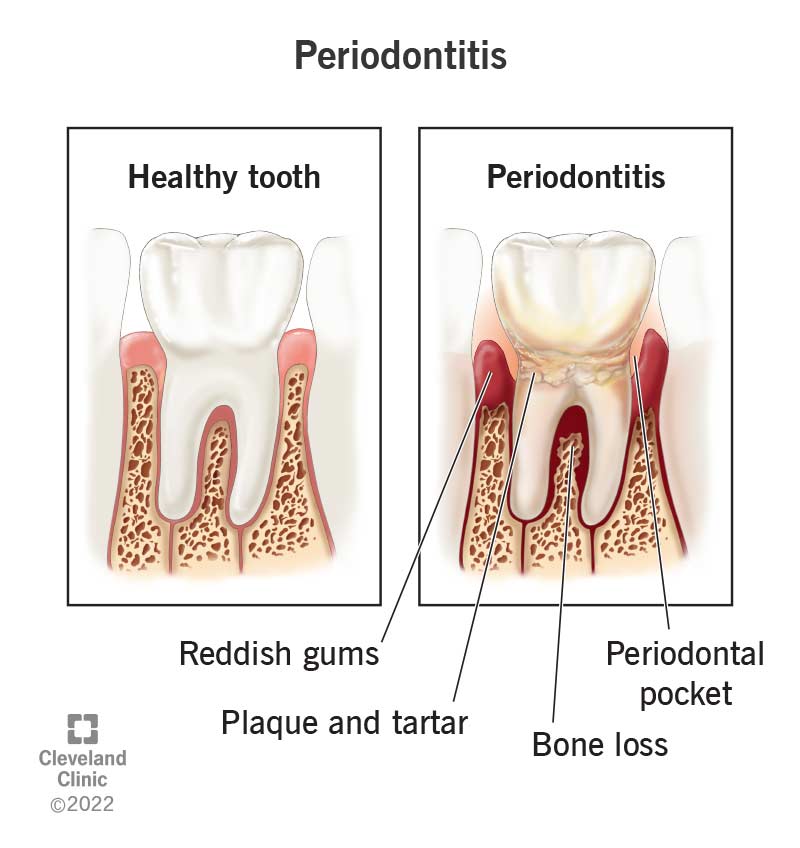
Periodontitis (pronounced “peh-ree-uh-don-TIE-tus”) is a form of gum disease. It’s a bacterial infection that causes your gums to bleed and swell. Eventually, it can damage the bone that supports your teeth, leading to wiggly teeth and tooth loss.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Periodontitis is more likely to happen as you age. It’s most common in people over 30. Still, it can affect anyone with poor oral hygiene. Some people are also more genetically prone to periodontitis than others. If your biological parents or grandparents have a history of gum disease, you’re more likely to develop it as well.
Healthcare providers classify periodontitis as mild, moderate or severe. They base this on how much bone you’ve lost around each tooth and on how much inflammation you have in your gums. There are surgical and nonsurgical treatments that can help treat this oral infection and keep your gums healthy.
Periodontitis symptoms include:
Often, periodontal disease doesn’t hurt, so you may have no idea that you have the disease. Catching periodontitis early helps prevent complications. See a dentist as soon as possible if you have these symptoms, and even if you don’t have any symptoms.
The main cause of periodontitis is poor oral hygiene. Bacteria create plaque and tartar that cling to your teeth surfaces. If you don’t clean your teeth as well or as often as you should, bacteria travel down beneath your gum line, where your toothbrush and floss can’t reach. These harmful bacteria wear away the tissues that support your teeth, leading to infection, bone loss and tooth loss.
Advertisement
The following risk factors can increase your chances of developing periodontitis:
Left untreated, periodontitis could lead to complications like:
Dentists typically diagnose periodontitis during routine examinations. During your appointment, they’ll likely:
Periodontitis treatment depends on the severity of the condition. Options include nonsurgical and surgical procedures. Your dentist should refer you to a gum specialist (periodontist) unless your disease is mild.
Healthcare providers may treat milder cases with nonsurgical procedures or lifestyle changes. These include:
Severe periodontitis usually requires surgery. These treatments include:
Your outlook depends on the severity of your condition and how soon you begin treatment. When you treat periodontitis early, you reduce your risk for long-term damage to your teeth and gums. Severe or untreated periodontitis can lead to bite changes, tooth loss and a host of other oral health problems.
Advertisement
If you already have missing teeth due to periodontitis, talk to your dentist about replacement options. Dental implants or bridges can restore your smile and your oral health.
You can’t cure periodontitis, but you can manage it with treatment. Talk to your dentist or periodontist about a personalized plan.
The best way to prevent periodontitis is to see a dentist regularly and practice good oral hygiene at home. People who are prone to periodontitis may need more frequent cleanings than people without gum disease. Ask your dentist how often you should have cleanings to maintain healthy teeth and gums.
If you develop sore, swollen or bleeding gums, schedule an appointment with a dentist right away. Early intervention is key to getting your oral health back on track.
The longer you wait, the worse the disease may get. As a result, you might need more extensive (and more costly) treatment. For example, you may be able to treat early-stage periodontitis with a deep dental cleaning. But late-stage periodontitis usually requires surgery, which is more expensive and invasive.
If you have periodontitis, here are a few questions you may want to ask your dentist:
Advertisement
No, periodontitis doesn’t directly cause death. But it’s associated with many other health conditions like rheumatoid arthritis, cardiac disease, low birth weight babies, Alzheimer’s disease and even some cancers. Some scientists believe that bacteria in your mouth can travel throughout your body via your bloodstream.
Some of the symptoms that come along with periodontitis, like swollen gums and bad breath, can take a toll on your self-esteem. Maybe you even cover your mouth when you smile or avoid social situations altogether. Most importantly, the infection can cause problems in your mouth and, in some cases, may spread to other parts of your body. You can’t fix periodontitis with brushing and flossing alone. You’ll need a dentist to help you. But don’t worry. Treatment can get rid of the infection and set you on the path to better oral health.
Advertisement
At Cleveland Clinic, we have expert knowledge when it comes to slowing and reversing gum disease. We’ll craft a treatment plan that focuses on you and your needs.

Last reviewed on 12/19/2024.
Learn more about the Health Library and our editorial process.