Cradle cap is a common, harmless skin condition that causes yellow scales and a rash on your baby’s scalp. It usually starts and goes away before your baby’s first birthday. Cradle cap doesn’t need treatment and clears up on its own within a few months. Simple, at-home care (like gently shampooing your baby’s scalp) may help speed things along.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Cradle cap is a harmless skin condition that causes yellow or white scaly patches on your baby’s scalp. The scales are greasy or flaky, and a rash may surround them. Rest assured that your baby isn’t in any danger or discomfort. Cradle cap has no negative effects on your baby’s health and doesn’t affect their eating or sleeping. It doesn’t cause itching or pain for your baby, and it usually clears up within a few weeks or months.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Cradle cap is very common and affects most babies at one point or another. Cradle cap usually starts within three months of birth, and nearly all cases appear during a baby’s first year of life. Because cradle cap usually starts early in an infant’s life, it typically goes away by their first birthday. A few babies develop cradle cap at 1 or 2 years of age.
Most cases of cradle cap are mild. Your baby likely won’t need any treatment, and the condition will go away on its own. You can talk to your pediatrician about your baby’s condition if you have any concerns or questions. And if you’d like, you can dote on your baby with some gentle at-home care to slough away the scaly skin a bit sooner.
Seborrheic dermatitis is the medical term for itchy red patches and greasy scales that can affect you at any age (in adults, you know it as “dandruff”). Cradle cap is a form of seborrheic dermatitis that’s limited to your baby’s scalp and occurs soon after birth. You might hear people call it infantile seborrheic dermatitis (ISD).
Some babies can develop seborrheic dermatitis in other areas besides their scalp (like their face or bottom). If that happens, your pediatrician can offer additional guidance on clearing up your baby’s condition.
Advertisement
You’ll notice patches of scaly skin on your baby’s scalp. When you touch the scales, they may feel fragile and flaky. Or, they may feel waxy and greasy. This scaly skin doesn’t cause your baby any pain or discomfort. Most babies don’t even seem to notice.
When you look at your baby’s scalp, you’ll see yellow or white patches of scales that resemble fish scales. These scales stick to your baby’s head and may:
Cradle cap refers only to the scaly rash on a baby’s scalp. However, some babies have seborrheic dermatitis that extends beyond their scalp, including parts of their face. If this happens, you may notice a rash:
If you notice these signs, tell your pediatrician. They’ll check your baby and see if they need special moisturizers or medicated creams.
Cradle cap isn’t contagious. You don’t need to worry about your baby spreading the rash to others. You can send your baby to daycare or let them have play dates with other babies.
Researchers don’t fully understand why babies get cradle cap. However, they believe it’s likely due to a combination of factors.
For example, glands in your baby’s scalp may produce too much oil (possibly due to hormones they receive from their mother). This causes skin cells that normally shed from your baby’s scalp to stay stuck to their scalp instead. A certain yeast (Malassezia) that naturally lives on your baby’s skin may also play a role, but researchers aren’t sure exactly how.
It can be frustrating not to know the cause of a condition in your baby, even if it’s harmless. But researchers do know it’s nothing you did and not your fault. Many babies get cradle cap, and it doesn’t affect their lives or health (they sleep through most of it, anyway!).
Your healthcare provider can diagnose cradle cap simply by looking at your baby’s scalp. The rash and scales, along with their location on your baby’s head, are easy clues to identifying the condition. Your baby doesn’t need any lab tests or biopsies.
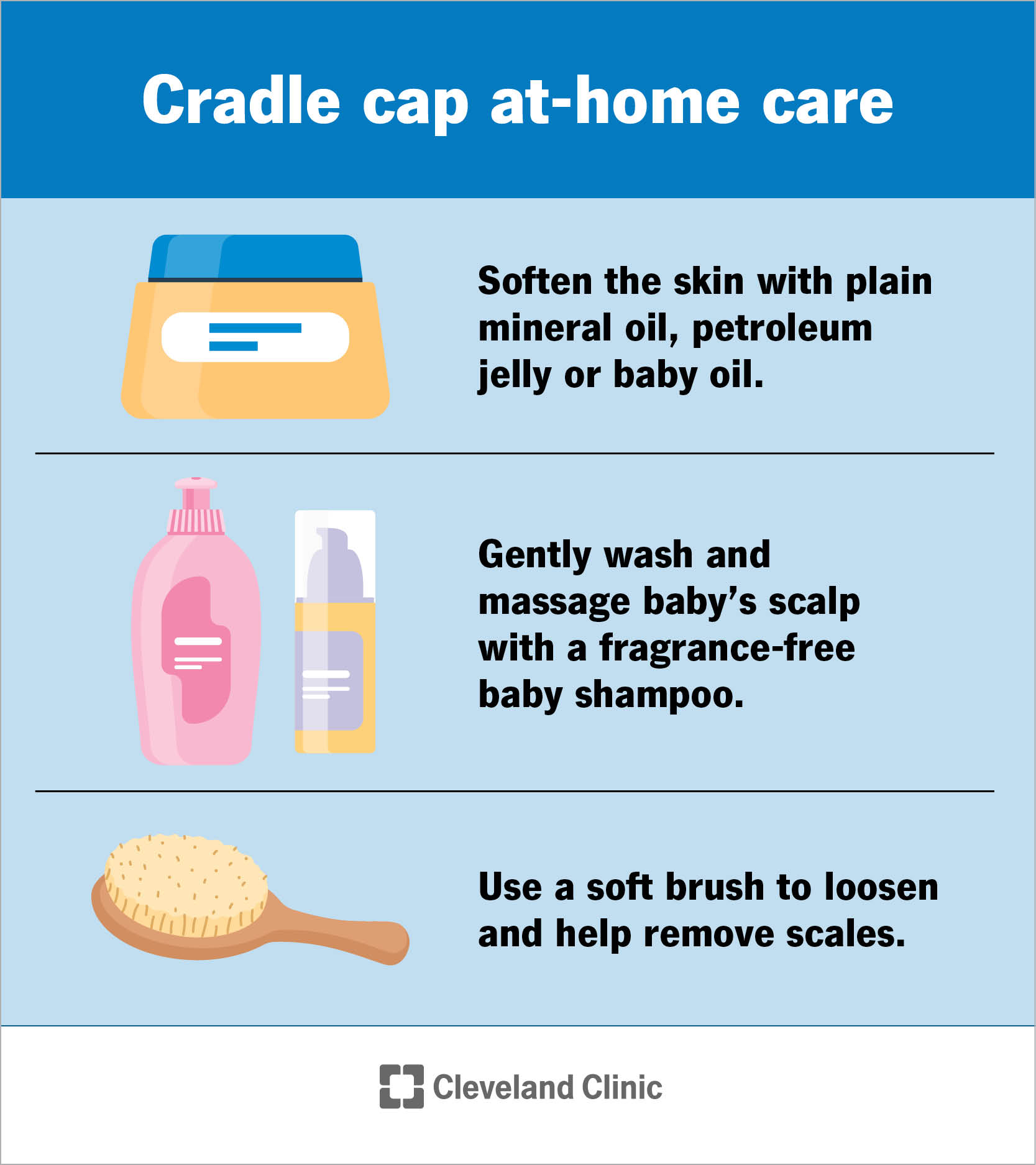
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/15786-cradle-cap)
If your baby only has cradle cap, without rashes elsewhere on their body, they likely don’t need medical treatment. Cradle cap should go away on its own within a few months.
But as a parent, it’s common to want to fix the issue. So, you might wonder, can I do cradle cap self-care at home? Yes, you can absolutely do some things to care for your baby’s scalp and possibly nudge those stubborn scales along. Here are some suggestions for how you can help get rid of cradle cap:
Advertisement
You may wonder what kind of shampoo to use. Sometimes the simplest solution is best. Regular old baby shampoo works just fine to lather up your baby’s scalp. Just make sure the shampoo is mild and unscented. Don’t use shampoos made for adults or designed to treat dandruff (these aren’t meant for a baby’s delicate skin).
Advertisement
If you’d like, you can try a specially-made shampoo for this condition. You’ll find these at the store with “cradle cap” on the label. You can also ask your pediatrician or dermatologist to recommend a shampoo formulated to help with cradle cap.
Cradle cap usually goes away on its own (without treatment) within a few weeks or months. Self-care at home may help move things along.
If cradle cap doesn’t go away in a few months, call your pediatrician. They can check your baby’s scalp and see if they have another skin condition that needs treatment.
Unfortunately, researchers don’t know of any ways to prevent cradle cap. That’s because they don’t fully understand the cause. But they do know it’s harmless and will go away quickly.
It’s a good idea to call your pediatrician if you notice one or more of the following issues:
These signs could mean your baby:
Advertisement
Parents are used to worrying about every little thing while navigating life with a newborn. So, it’s normal to go into panic mode if you see a rash and scales on your baby’s scalp. You may think, what did I do wrong? What’s the matter with my baby’s skin?
Let go of the worries. You did nothing wrong, and your baby is just fine. Cradle cap is common and harmless. Most cases are mild and clear up on their own. But if cradle cap decides to linger a little longer for your baby, or your baby develops rashes elsewhere, it’ll still be OK. Your healthcare provider can look at your baby’s skin and see if they need treatment. They’ll help you learn what’s happening and how to make it better.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
As your child grows, you need healthcare providers by your side to guide you through each step. Cleveland Clinic Children’s is there with care you can trust.
