Mohs surgery is a precise, outpatient procedure to remove high-risk skin cancer while preserving healthy tissue. The process of microscopic examination and layer-by-layer excision allows for complete tumor removal and high cure rates.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Video content: This video is available to watch online.
View video online (https://cdnapisec.kaltura.com/p/2207941/sp/220794100/playManifest/entryId/1_z584h18f/flavorId/1_5f3sgelj/format/url/protocol/https/a.mp4)
What you can expect during Mohs skin cancer surgery.
Mohs surgery (also known as Mohs micrographic surgery) is a method used to remove high-risk skin cancer. It’s very precise. Your surgeon cuts away (excises) the tumor in layers starting with the visible portion of the tumor and a margin of skin cells around it. Then, the sides and deep edges are examined under a microscope. If the skin cancer extends to any of the edges (margins) your surgeon will remove more tissue in the positive areas, and look at the new sample under a microscope. This process continues until all of the cancer is removed.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
One of the advantages of Mohs surgery is that your surgeon only removes cancerous tissue. This means that your healthy tissue is spared, making Mohs a useful approach for skin cancers on your face, scalp, ear, hands, feet and genital areas.
The procedure was developed by Frederic E Mohs, MD, in the 1930s and has since been refined. Originally, Dr. Mohs injected the tumor with a preserving chemical so that when removed (excised), he could inspect the tissue under a microscope. But the initial process of preparing fixed-tissue slides took several days, the use of chemicals to cauterize the tumor was controversial and the procedure was painful.
About 20 years passed before Dr. Mohs and his colleagues tried a new technique to remove carcinoma from an eyelid: the surgery could be done in one day using frozen fresh tissue in slide preparation.
Excision is a procedure through which your surgeon removes the skin cancer and a margin of surrounding skin and the specimen is sent to pathology for processing and interpretation. In general, less than 1% of the margins are checked with wide local excision. . Mohs micrographic surgery involves excision with a smaller margin and the tissue is processed in such a way that your surgeon checks 100% of the deep and side (lateral) margins.
Advertisement
The Mohs surgery procedure treats the most common forms of skin cancer: basal cell carcinoma (BCC) and squamous cell carcinoma (SCC). Mohs surgery is also sometimes used to treat other skin cancers, including certain melanomas, dermatofibrosarcoma protuberans, microcystic adnexal carcinoma, sebaceous carcinoma and extramammary Paget disease, among others.
Mohs surgery is done in a doctor’s office or outpatient surgical center. After each excision, you’ll wait in a waiting room or the operating room while your care team prepares slides of your tumor and your surgeon inspects those slides. If your provider finds tumor at any of the margins, you will be brought back in so your surgeon can remove another layer of tissue for further inspection. This process can take a while, so be sure to bring a book or electronic device to keep you occupied while you wait.
Mohs surgery is a very common treatment for high-risk skin cancer because it has a cure rate of up to 99%. This is the lowest recurrence rate of any other treatment for skin cancer.
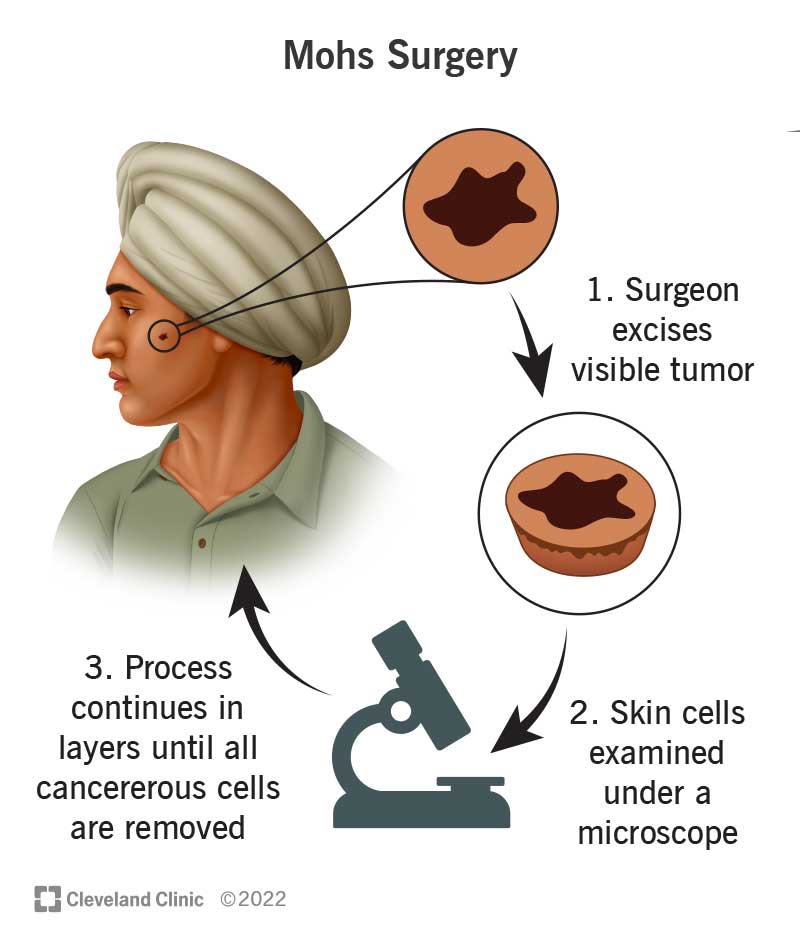
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/13312-mohs-surgery)
Before you have a Mohs surgery for skin cancer, you’ll see your dermatologist for a physical exam of the site and surrounding tissue. Together, you and your dermatologist will review:
Depending on your general health and the location of the surgical site, you may need to take preoperative antibiotics.
The Mohs procedure involves a layer-by-layer removal of skin that contains cancer cells. Here are the typical steps in the procedure:
Advertisement
After complete removal of the skin cancer, your surgeon will discuss the best method of managing your wound. The choices include:
Yes, most people are awake for Mohs surgery. Your surgeon will numb the area with injected medications (anesthetics). You will feel pressure and touch but no pain, and you’ll rest comfortably in the waiting room or in the operating room while they analyze your tissue. If you need more skin removed, you may still be numb from the initial injections, or more injections may be needed.
It’s quite common to feel anxious before a procedure. Your healthcare provider may recommend a variety of techniques to calm your nerves. During the procedure, you may want to listen to music or a guided meditation. Your provider may also give you antianxiety medication before the procedure.
Advertisement
Mohs surgery may take only a few hours, or it may take the whole day. How long the procedure takes depends on the tumor itself: bigger, deeper tumors take longer to remove completely.
Mohs micrographic surgery has the highest cure rate of all treatments for basal cell and squamous cell skin cancers. For basal cell carcinoma, the cure rate is up to 99% for new cases and up to 94% for recurrent cases. For squamous cell carcinoma, the cure rate is 95% to 99% for new cases and 90% for recurrent cases.
The most important advantages of Mohs surgery are the complete microscopic examination, which allows for complete removal of the cancer and high cure rates, and the ability to spare as much normal skin as possible.
Additional advantages of Mohs surgery for skin cancer include:
The risks associated with the Mohs surgery itself are very low. Please discuss your particular health issues and any concerns about the Mohs procedure with your surgeon. Listed below are the usual risks associated with Mohs surgery:
Advertisement
Most patients report mild to moderate pain following Mohs surgery. The pain goes away gradually over a few days and can be effectively managed with acetaminophen (Tylenol®). Individuals who have Mohs surgery on their scalp or whose wound is larger than 3 square centimeters tend to report more pain than those who have the procedure on other areas.
Scars from Mohs surgery continue to heal for 12 to 18 months after your procedure. In the year following Mohs surgery, you’ll want to be patient as your scar matures, then fades. If you’re unhappy with your scar, talk to your surgeon about your options for scar revision.
Following Mohs surgery, you’ll want to take care of yourself to allow for optimal healing. Your surgeon will give you instructions for aftercare following Mohs surgery. When you go home, you’ll have a dressing on your wound. Leave it undisturbed for the first 24 to 48 hours, or as directed by your surgeon. After that initial period of healing, remove the dressing for wound care two times a day or as directed. To care for your wound, cleanse with 3% hydrogen peroxide or a mild soap, then cover your wound with petroleum jelly and cover it with a dressing that won’t stick to your wound. Once the dressing is no longer needed, be sure to protect your scar using sunscreen with a sun protection factor (SPF) of at least 30, as well as protective hats during any sun exposure.
Your surgeon will also instruct you to:
You should cover your wound with petroleum jelly (Vaseline®) at least until your sutures are removed (one to two weeks). At this follow-up visit, your surgeon will take a look at the area to see how your wound is healing. They may instruct you to use petroleum jelly for another couple of weeks.
Following any surgery, you should feel comfortable calling your doctor with questions about the procedure or how you’re healing. You should also call your surgeon if you experience:
It’s normal to have a little bleeding or oozing from the wound, especially in the first few hours after surgery. Applying pressure to the wound should stop the bleeding, but call your surgeon if the bleeding doesn’t stop.
You can expect to have some mild to moderate pain or discomfort following Mohs surgery. Call your surgeon if:
An infected wound can lengthen your recovery time and make your scar heal less optimally. . You may need topical or oral antibiotics. Contact your surgeon if:
Hearing the word “cancer” from you doctor can be scary. But if your skin cancer is caught early — before it spreads to other areas — it’s possible that you’ll be cured in a single day with a precise procedure called Mohs micrographic surgery. In Mohs surgery, your surgeon removes your tumor, layer by layer. Each layer is carefully labeled and examined under a microscope to look for cancer. If cancer cells remain, your surgeon removes and examines another layer until the cancer is completed gone.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Skin cancer doesn’t always need to leave a big scar. Talk to Cleveland Clinic experts about Mohs surgery for the best results.
