Esophageal manometry is a swallowing test that can help determine if your esophagus is able to move food to your stomach normally. Problems with the motor function in your esophagus are called esophageal motility disorders. Test details and preparation are discussed.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
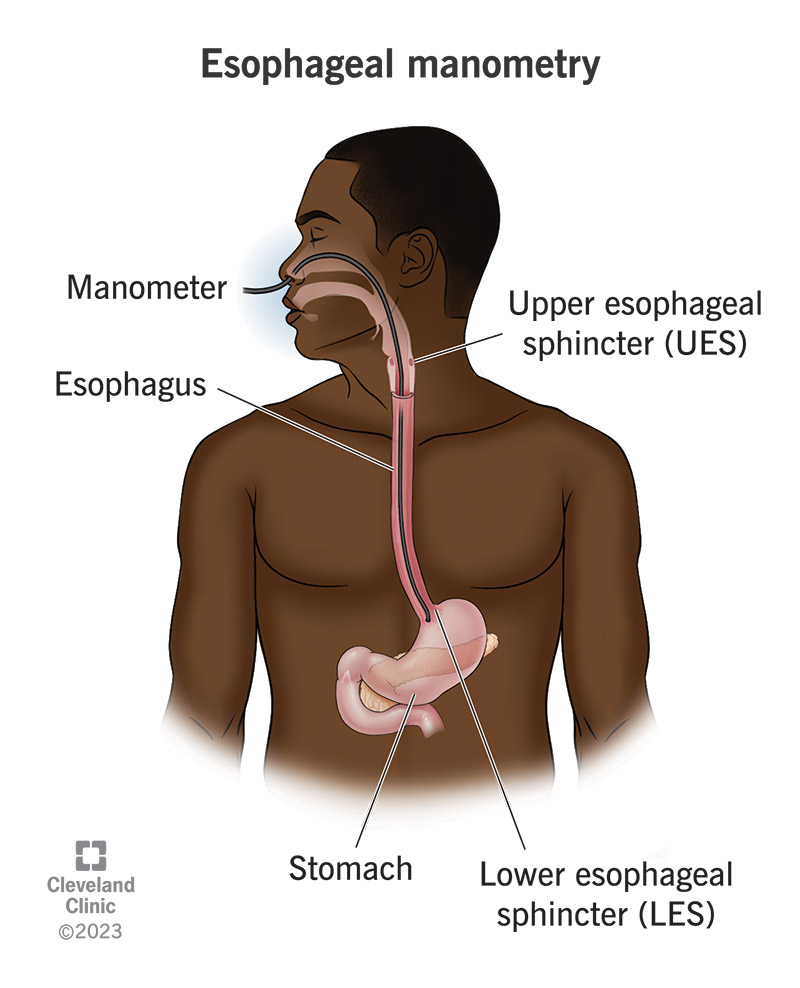
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/4952-esophageal-manometry)
An esophageal manometry test is a study of your esophageal motility (motor function). Your esophagus is the muscular swallowing tube that connects your mouth to your stomach. Muscles in your esophagus move food down to your stomach when you swallow and keep it from coming back up. But certain esophageal disorders can interfere with this process, causing swallowing problems and reflux.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A healthcare provider might want to check your esophageal motility if you’ve been having issues related to swallowing or keeping food and other substances down in your stomach. If you’re having a manometry test, it’s likely you’ve already had an imaging test to look for structural problems in your esophagus. If imaging can’t explain your symptoms, motility testing might be the next step.
Possible symptoms of esophageal motility disorders include:
Manometry is a measurement of pressure, using a pressure-sensing device called a manometer. It detects the pressure that different muscles produce when they activate. An esophageal manometry test measures two types of muscle activity in your esophagus. It measures the movements that carry food downward (peristalsis) and how the valves at the top and bottom of your esophagus open and close.
Abnormal pressure in these muscles might help explain your symptoms and diagnose certain conditions, including:
High-resolution manometry (HRM) works by placing a catheter plotted with high-resolution pressure sensors inside your esophagus. Up to 36 sensors, spaced 1 centimeter apart, span your esophagus and measure your muscle contractions when you swallow. They transmit their data to a computer, which converts it into a topographical pressure map (esophageal pressure topography, or EPT).
Advertisement
You’ll need to avoid eating or drinking within the six hours before the test. Your healthcare provider may also ask you to discontinue certain medications 24 hours before the test, including:
You typically won’t be sedated, though you can discuss sedation with your healthcare provider in advance if you’re very anxious about the test. Esophageal manometry shouldn’t be painful, although you may find the catheter in your esophagus to be a little uncomfortable. You’ll have topical anesthesia to help numb your throat to minimize this discomfort. Your throat might feel a little sore afterward.
To set up the test, a healthcare provider will need to place the catheter with the sensors on it inside your esophagus. They do this by passing it through your nasal cavity and down through your esophagus until it reaches your stomach. Before placing the catheter (nasogastric tube), they’ll lubricate the end and apply a topical anesthetic inside your nose and throat to reduce the discomfort from friction.
Once the tube’s in place, they’ll take a baseline reading while you lie on your back and breathe regularly. Then you’ll swallow some sips of water. For the standard test, you’ll swallow seven to 10 times while lying down or reclining. Your healthcare provider might test some different variations after that. For example, they might have you sit upright, or swallow something thick, like applesauce.
You might feel like coughing, choking or gagging when the catheter is being placed, but this usually passes quickly. Some people have nosebleeds from the nasogastric tube, but this is uncommon.
It shouldn’t take more than 15 minutes.
Your healthcare provider will interpret the results of your esophageal pressure topography map.
The results will show:
Abnormal results might include:
Advertisement
Yes. The results of your esophageal manometry test will show your healthcare provider specifically what’s going on in your esophagus when you swallow. This will allow them to recommend specific treatments. If they’ve already recommended a specific treatment, such as anti-reflux surgery or hiatal hernia repair, this test will tell your provider whether the treatment will be safe and effective for you.
A barium swallow, also called an esophagram, is another test healthcare providers use to study your esophagus. It’s more of an imaging test than a mechanical test, however. For the test, you swallow a contrast solution called barium that coats the inside of your esophagus, which helps it stand out in black and white. A healthcare provider takes real-time video X-rays of your esophagus while you swallow.
An esophagram can help a healthcare provider see defects or obstructions inside your esophagus that might be causing your symptoms. The real-time video might show you struggling to swallow, but it can’t show what’s really going on mechanically in your esophagus. That’s what manometry is for. A healthcare provider will usually take an esophagram first, then follow up with manometry to investigate further.
Advertisement
The function of your esophagus is to swallow solids and liquids and to keep them from coming back up out of your stomach. If either of these functions aren’t working quite right, it can cause uncomfortable symptoms for you. Esophageal manometry can show your healthcare provider exactly where and how these functions are failing. This can lead them to the right diagnosis and treatment for your condition.
Advertisement
Learn more about the Health Library and our editorial process.
Cleveland Clinic's health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability, and up-to-date clinical standards.
Cleveland Clinic's health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability, and up-to-date clinical standards.
Esophageal disorders can cause many symptoms, including heartburn or trouble swallowing. At Cleveland Clinic, we’ll find a treatment that works for you.
